Digestion Overview - The Breakdown Basics
- Digestion: Mechanical & chemical breakdown of food into absorbable units.
- Types:
- Mechanical: Chewing, churning, segmentation.
- Chemical: Enzymatic hydrolysis.
- Key Sites:
- Mouth: Mastication, salivary amylase (starch).
- Stomach: Churning, pepsin (proteins), gastric lipase (fats).
- Small Intestine: Major digestion/absorption; pancreatic & intestinal enzymes, bile (fats).
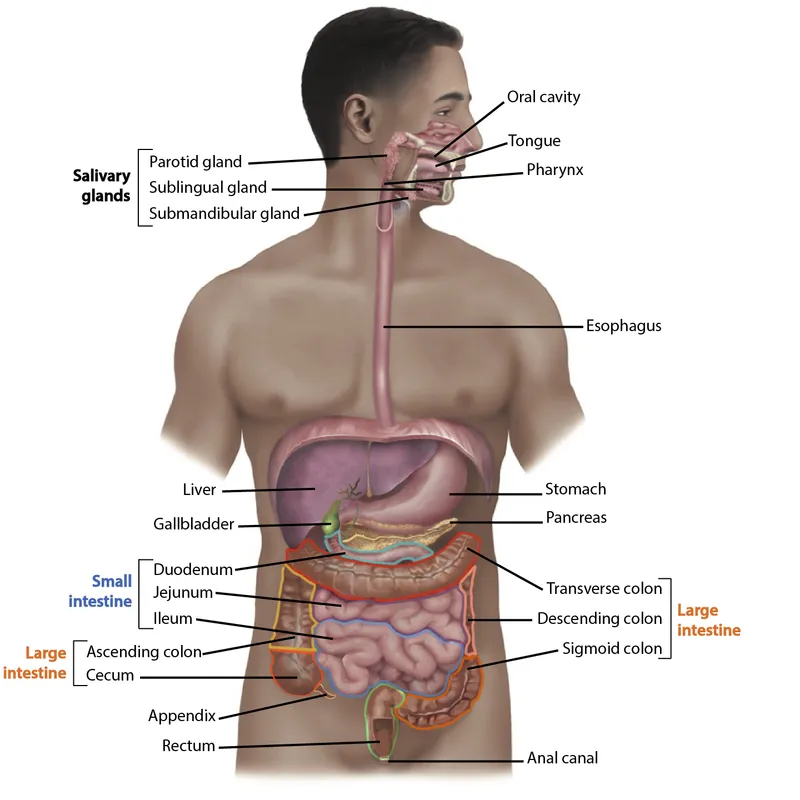
⭐ Brunner's glands in the duodenum secrete alkaline mucus to neutralize acidic chyme from the stomach.
Carbohydrate Digestion - Sweet Surrender
- Oral Cavity: Salivary α-amylase (ptyalin) begins starch breakdown.
- Stomach: Digestion halts; acid inactivates ptyalin.
- Small Intestine (Major Site):
- Pancreatic α-amylase: Converts starch/glycogen to oligosaccharides (maltose, maltotriose, α-limit dextrins).
- Brush Border Disaccharidases:
- Lactase: Lactose → Glucose + Galactose
- Sucrase: Sucrose → Glucose + Fructose
- Maltase/Isomaltase: Maltose/α-limit dextrins → Glucose
- Absorption (Enterocytes):
- Glucose/Galactose: Apical SGLT1 (Na+-cotransport); basolateral GLUT2.
- Fructose: Apical GLUT5 (facilitated); basolateral GLUT2.

⭐ SGLT1 co-transports glucose and galactose with Na+ into enterocytes; its activity is crucial for oral rehydration therapy.
Protein Digestion - Amino Acid Assembly
- Stomach: Pepsinogen (chief cells) $\xrightarrow{HCl}$ Pepsin; initiates protein hydrolysis, cleaving peptide bonds.
- Small Intestine - Pancreatic Proteases (Lumen):
- Endopeptidases: Trypsin, Chymotrypsin, Elastase break proteins into smaller peptides.
- Exopeptidases: Carboxypeptidases A & B remove C-terminal amino acids.
- Activation Cascade:
- Small Intestine - Brush Border Enzymes (Surface): Aminopeptidases, Dipeptidases, Tripeptidases $\rightarrow$ free amino acids, di/tripeptides.
- Absorption (Enterocytes):
- Amino acids: Na+-dependent cotransporters (e.g., for neutral, basic, acidic AAs).
- Di/Tripeptides: PepT1 (H+-cotransporter); intracellularly hydrolyzed to AAs.
⭐ Enteropeptidase (enterokinase), a brush border enzyme, is essential for activating trypsinogen to trypsin, which then activates other pancreatic proenzymes.
Lipid Digestion - Fatty Facts Unfurled
- Key Enzymes: Lingual lipase (mouth), gastric lipase (stomach), pancreatic lipase & colipase (SI).
- Bile Salts (Liver): Emulsify fats $ ightarrow$ smaller droplets. Critical for lipase action.
- Pancreatic Lipase: TGs $ ightarrow$ 2-Monoacylglycerol (2-MAG) + 2 Free Fatty Acids (FFAs).
- Micelle Formation: 2-MAG, FFAs, cholesterol, fat-soluble vitamins + bile salts $ ightarrow$ transport to enterocyte.
- Absorption:
- LCFAs & 2-MAG: Enter enterocyte $ ightarrow$ re-esterified to TGs.
- SCFAs/MCFAs: Directly to portal blood.
- Chylomicrons: TGs + ApoB-48 $ ightarrow$ packaged in enterocyte $ ightarrow$ lymph (lacteals) $ ightarrow$ blood.
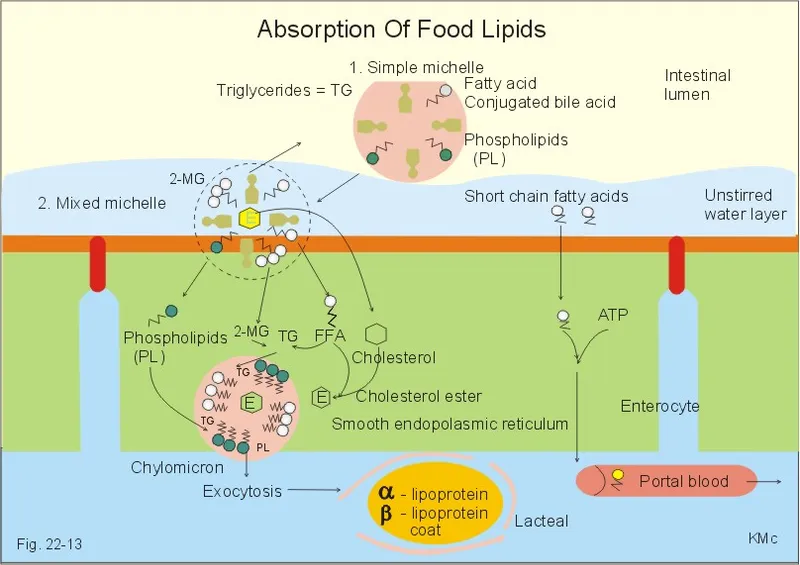
⭐ Abetalipoproteinemia: ApoB-48/ApoB-100 deficiency $ ightarrow$ no chylomicrons $ ightarrow$ severe fat malabsorption.
Vitamin & Mineral Absorption - Tiny Titans' Transport
- Fat-Soluble (A,D,E,K): Absorbed with dietary fats (micelles) in small intestine.
- Water-Soluble:
- B12 (Cobalamin): Binds Intrinsic Factor (IF); absorbed in terminal ileum. 📌 B12-IF: Terminal Team.
- Folate: Jejunum (active transport).
- Vit C (Ascorbic Acid): Na⁺-dependent active transport; ileum.
- Minerals:
- Iron ($Fe^{2+}$): Duodenum (DMT1 transporter). 📌 Iron: Duodenal Doyen.
- Calcium ($Ca^{2+}$): Duodenum, jejunum (Vit D-dependent active transport).

⭐ Pernicious anemia: autoimmune parietal cell destruction → IF deficiency → B12 malabsorption in terminal ileum.
High‑Yield Points - ⚡ Biggest Takeaways
- Carbohydrate digestion: Salivary amylase (mouth), pancreatic amylase & brush border enzymes (small intestine). Absorption: SGLT1 (glucose/galactose), GLUT5 (fructose).
- Protein digestion: Pepsin (stomach), pancreatic proteases & brush border peptidases (small intestine). Absorbed as amino acids, di/tri-peptides.
- Fat digestion: Pancreatic lipase (major); requires bile salts for emulsification. Chylomicrons for lymphatic absorption.
- Iron absorption: Duodenum (Fe2+ form); regulated by hepcidin. Vitamin C enhances.
- Vitamin B12 absorption: Requires intrinsic factor; occurs in terminal ileum.
- Calcium absorption: Duodenum/jejunum; Vitamin D dependent.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

