EPOC & Oxygen Debt - Huffing & Puffing Pays
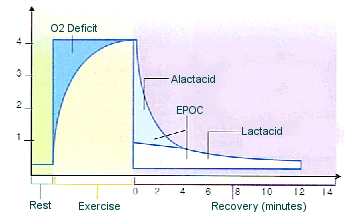
- EPOC (Excess Post-exercise Oxygen Consumption): ↑ O₂ uptake above resting levels after exercise.
- Oxygen Debt: O₂ consumed in recovery minus resting O₂ consumption over same time.
- EPOC is the more current term.
- Two Components:
- Rapid (Alactacid): 2-4 mins. Replenishes ATP/PCr; re-oxygenates myoglobin & hemoglobin.
- Slow (Lactacid): >30 mins - hours. Lactate metabolism (Cori cycle), glycogen resynthesis, ↓ body temp, hormone effects (catecholamines, thyroxine).
- Factors: ↑ Intensity & ↑ duration → ↑ EPOC magnitude & duration.
⭐ The slow component of EPOC, primarily for lactate removal and glycogen resynthesis, can last for several hours and significantly contributes to post-exercise caloric expenditure.
Fuel Replenishment - Refilling the Tank
- Creatine Phosphate (CP): Rapid, aerobic process. Full restoration in ~3-5 min post-exercise. $PCr + ADP + H^+ \leftrightarrow ATP + Cr$. Essential for immediate high-intensity efforts.
- Muscle Glycogen: Critical for endurance.
- Rapid phase (insulin-independent): First 30-60 min.
- Slow phase (insulin-dependent): Lasts hours; optimal CHO intake 0.7-1.5 g/kg/hr.
- Liver Glycogen: Slower than muscle; prioritizes blood glucose homeostasis. Replenished over several hours.
- Myoglobin Reoxygenation: Very rapid; restores intramuscular O₂ stores within 1-2 min of O₂ availability.
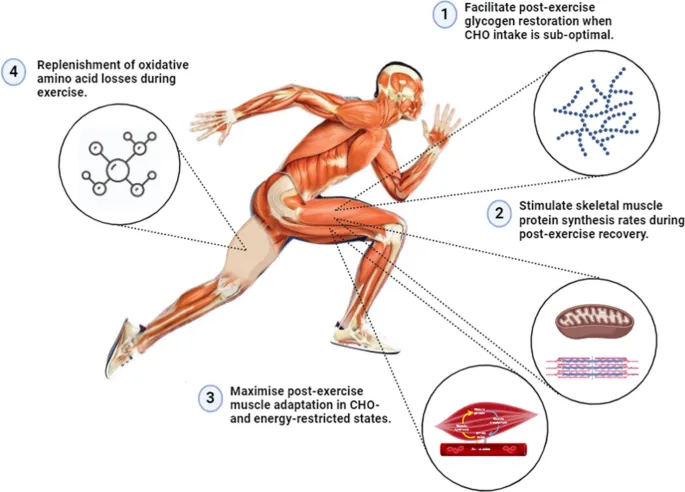
⭐ Glycogen synthase activity is highest immediately post-exercise, making early CHO intake crucial for rapid muscle glycogen repletion.
Muscle Repair & Soreness - Rebuild & Recover
- Exercise-Induced Muscle Damage (EIMD): Microtears in sarcomeres & Z-discs, especially from eccentric contractions.
- Inflammatory Cascade:
- Neutrophils & macrophages clear cellular debris.
- Pro-inflammatory cytokines (e.g., IL-6, TNF-α) released, then anti-inflammatory signals promote healing.
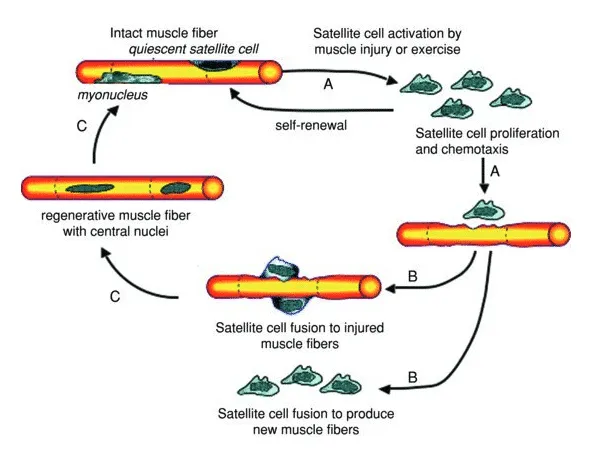
- Satellite Cell Role:
- Activated muscle stem cells proliferate & differentiate.
- Fuse to repair damaged fibers or form new myofibrils (contributing to hypertrophy).
- Delayed Onset Muscle Soreness (DOMS):
- Symptoms: Muscle pain, tenderness, stiffness, swelling, ↓ strength.
- Typically peaks 24-72 hours post-exercise.
- Rebuilding Phase:
- Upregulated muscle protein synthesis (MPS); mTOR pathway is key.
- Net positive protein balance crucial for repair & adaptation.
⭐ DOMS is most intensely induced by novel eccentric exercise, leading to ultrastructural damage (e.g., Z-disk streaming) and an acute inflammatory response, not lactic acid accumulation.
Hormonal & Fluid Reset - Balancing Act
- Hormonal Shifts (Post-Exercise):
- Cortisol: Initial ↑ (stress response), then ↓; anti-inflammatory, mobilizes fuel.
- GH & Testosterone: ↑; crucial for muscle repair, protein synthesis.
- Insulin Sensitivity: ↑ (enhances glucose uptake, glycogen storage); Glucagon: ↓.
- Catecholamines (Adrenaline/Noradrenaline): ↓ from exercise peak.
- Fluid & Electrolyte Restoration:
- Rehydration: Critical to restore plasma volume, support cardiac output.
- Electrolytes: Essential to replace Na+, K+, Cl- lost via sweat.
- Key Regulatory Hormones:
- ADH (Vasopressin): ↑ secretion; promotes renal water reabsorption.
- Aldosterone: ↑ secretion; promotes renal Na+ & water retention.
⭐ Post-exercise ADH (Vasopressin) surge is vital for rapid renal water reabsorption, effectively combating dehydration.
High‑Yield Points - ⚡ Biggest Takeaways
- EPOC (Oxygen Debt) features fast (alactacid) and slow (lactacid) phases for recovery.
- Fast component rapidly restores ATP-PCr and myoglobin O₂.
- Slow component handles lactate clearance (Cori cycle, oxidation) and glycogen replenishment.
- Post-exercise carbohydrate intake is crucial for rapid glycogen resynthesis.
- Active cool-down accelerates lactate removal more than passive recovery.
- Insulin promotes glycogen storage; catecholamines and cortisol levels normalize.
- Fluid and electrolyte balance restoration is essential after strenuous activity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

