Neural Adaptations - Brains & Brawn Boost
- Early strength gains (first 4-8 weeks) are largely neural, preceding significant hypertrophy.
- Enhanced Central Drive:
- ↑ Motor Unit (MU) Recruitment: More MUs activated.
- ↑ MU Firing Rate (Rate Coding): MUs fire at higher frequencies.
- ↑ MU Synchronization: Improved coordinated firing of MUs.
- Reduced Neural Inhibition:
- ↓ Golgi Tendon Organ (GTO) autogenic inhibition: Protects less, allows more force.
- ↓ Renshaw cell recurrent inhibition.
- Improved Intermuscular Coordination: Better agonist-antagonist coordination.
⭐ Cross-education effect: Unilateral training can ↑ strength in the contralateral, untrained limb by ~7-22%, due to central neural drive.
Muscle Hypertrophy & Fiber Types - Bulk Up & Switch Up
- Muscle Hypertrophy: ↑ muscle fiber cross-sectional area (CSA).
- Mechanism: ↑ contractile proteins (actin, myosin) via satellite cell activation, myonuclear addition & ↑ protein synthesis (mTOR pathway).
- Primarily Type II fibers show greater hypertrophy.
- Muscle Fiber Types:
- Type I (SO - Slow Oxidative): Red, aerobic, fatigue-resistant, endurance. Low force output.
- Type IIa (FOG - Fast Oxidative Glycolytic): Pink/Red, hybrid (aerobic/anaerobic), adaptable. Moderate force & fatigue resistance.
- Type IIx (FG - Fast Glycolytic): White, anaerobic, high power, fast fatigue. Max effort/sprints.
- Training-Induced Shifts:
- Resistance Training: Significant hypertrophy (esp. Type II), ↑ strength/power.
- Endurance Training: ↑ oxidative capacity (Type I, IIa); common shift from Type IIx → Type IIa.
- Genetics largely determine baseline fiber type proportions.
⭐ Type IIx muscle fibers generally exhibit the most significant increase in cross-sectional area (hypertrophy) in response to resistance training.
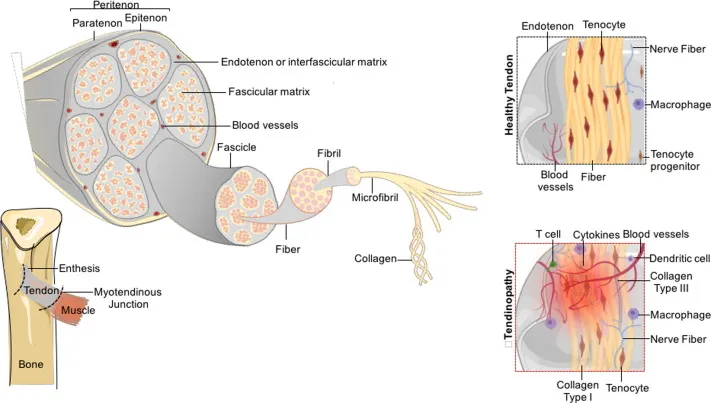
Connective Tissue & Bone - Tougher Tendons, Bolder Bones
- Tendons & Ligaments:
- ↑ Collagen content & cross-linking → ↑ tensile strength, stiffness.
- Hypertrophy at musculotendinous junction & bony insertions.
- ↑ Size & number of collagen fibrils.
- Adaptation slower than muscle; ⚠️ risk of tendinopathy with rapid load progression.
- Bone:
- Wolff's Law: Bone remodels in response to mechanical stress.
- ↑ Bone Mineral Density (BMD), especially with high-impact & resistance training.
- Specificity: Bone formation primarily at sites of stress.
- Osteogenic stimuli: High-magnitude, dynamic, novel loading patterns.
-
⭐ Minimal Effective Strain (MES) is the threshold strain that must be exceeded to stimulate new bone formation.
 oka
oka
Metabolic & Endocrine Changes - Fuel & Hormone Hustle
- Fuel Metabolism Shifts:
- ↑ Muscle glycogen & Intramuscular Triglycerides (IMTG) stores.
- ↑ Fat oxidation, especially at submaximal intensities ("glycogen sparing").
- ↑ GLUT4 expression: better glucose uptake, ↑ insulin sensitivity.
- ↑ Lactate threshold: delayed fatigue; enhanced lactate clearance & utilization (e.g., Cori cycle, intracellular lactate shuttle).
- ↑ Mitochondrial biogenesis & oxidative enzyme capacity (e.g., citrate synthase).
- Endocrine Adaptations:
- Acute Exercise: ↑ Catecholamines (Epinephrine, Norepinephrine), glucagon, Growth Hormone (GH), cortisol; ↓ insulin (promotes fuel mobilization).
- Chronic Training:
- Blunted hormonal response (catecholamines, cortisol) to a given absolute exercise load.
- Improved insulin sensitivity persists.
- Resistance training: promotes net muscle protein synthesis.
⭐ Trained individuals show an earlier and greater reliance on fat oxidation during submaximal exercise, effectively "sparing" limited muscle glycogen stores.
High‑Yield Points - ⚡ Biggest Takeaways
- Initial strength gains are predominantly neural: ↑ motor unit recruitment, firing rate, and synchronization.
- Reduced antagonist co-activation and decreased Golgi Tendon Organ inhibition enhance net force.
- Muscle fiber hypertrophy, particularly of Type II fibers, is a key long-term adaptation.
- Fiber type transitions (e.g., Type IIx to Type IIa) improve metabolic efficiency and fatigue resistance.
- Cross-education effect highlights central nervous system adaptations.
- Increased connective tissue strength (tendons, ligaments) supports force transmission and injury prevention.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


