Foundations & Methods - Assay Arsenal
- Immunoassays: Cornerstone for hormone quantification.
- Competitive (e.g., RIA): Labeled hormone competes with patient hormone for antibody binding. Signal inversely proportional to analyte.
- Non-competitive/Sandwich (e.g., IRMA, ELISA, CLIA): Analyte "sandwiched" between two antibodies. Signal directly proportional. Generally higher sensitivity.
- Chromatography (HPLC, GC-MS): Separates & quantifies structurally similar hormones (e.g., steroids, catecholamines).
- Bioassays: Measure biological effect; mainly research.
- Dynamic Function Tests (DFTs): Assess endocrine gland responsiveness.
- Stimulation tests: Evaluate reserve capacity (e.g., ACTH stimulation for adrenal insufficiency).
- Suppression tests: Check feedback integrity & autonomy (e.g., Dexamethasone suppression for Cushing's syndrome).
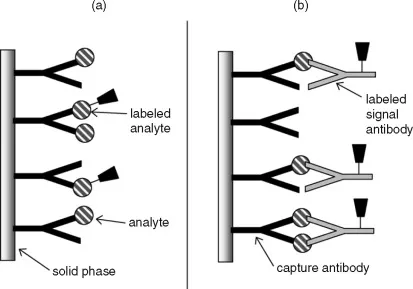
⭐ ELISA is widely used due to its versatility, safety (no radioisotopes), and suitability for automation.
Pituitary Puzzles - Master Gland Checkup
- Strategy: Clinical exam, baseline hormones, dynamic tests, imaging.
- Baseline Hormones:
- Anterior: GH (via IGF-1), PRL, ACTH (8 AM cortisol), TSH (fT4), LH/FSH (sex steroids).
- Posterior: ADH (serum/urine osmolality).
- Dynamic Function Tests:
- Stimulation (hypofunction):
- ITT: GH & ACTH. 📌 "Insulin STRESSES Pituitary to ACT & GROW."
- Glucagon stim: GH & ACTH alt.
- Suppression (hyperfunction):
- OGTT: GH suppression (Acromegaly).
- DST: ACTH (Cushing's).
- Stimulation (hypofunction):
- Imaging: MRI (sella) primary.

⭐ The Insulin Tolerance Test (ITT) is gold standard for GH & ACTH reserve; hypoglycemia (glucose < 2.2 mmol/L or 40 mg/dL) is key for stimulation.
Thyroid & Adrenal Tales - Axis Investigations
Thyroid Axis (HPT):
- TSH: Best initial.
- ↑ TSH, ↓ Free T4: Primary hypothyroidism.
- ↓ TSH, ↑ Free T4/T3: Primary hyperthyroidism.
- Normal/↓ TSH, ↓ Free T4: Central hypothyroidism.
- Antibodies: Anti-TPO Ab (Hashimoto's), TRAb (Graves').
- RAIU Scan: Hot (active) vs. Cold (inactive, ↑ Ca risk) nodules.
Adrenal Axis (HPA):
- Cushing's Syndrome:
- Screening: 24-hr UFC, Late-night salivary cortisol, 1mg ONDST.
- Localization: Plasma ACTH, 8mg HDDST, CRH stimulation.
- Adrenal Insufficiency:
- Basal: Morning cortisol, ACTH.
- Dynamic: ACTH stimulation (Synacthen 250µg); subnormal rise → Addison's.
- Pheochromocytoma: Plasma/Urinary metanephrines & VMA.
- Hyperaldosteronism: Aldosterone-Renin Ratio (ARR). 📌 DST: Low dose screens, High dose differentiates.

⭐ Differentiating Cushing's Disease (pituitary) from ectopic ACTH: HDDST suppresses cortisol in most Cushing's Disease, not ectopic ACTH.
Sugar & Bone Balance - Metabolic Markers
- Glucose Homeostasis Markers
- Fasting Plasma Glucose (FPG): Normal <100; Diabetes ≥126 mg/dL.
- Post-Prandial (2-hr OGTT): Normal <140; Diabetes ≥200 mg/dL.
- HbA1c: Reflects ~3 months glucose. Normal <5.7%; Diabetes ≥6.5%.
- C-peptide: Endogenous insulin; ↓ T1DM.
- Autoantibodies (GAD65, IAA): For T1DM.
- Calcium & Bone Metabolism Markers
- Serum Calcium: Total (8.5-10.5 mg/dL), Ionized. Correct for albumin.
- Serum Phosphate: (2.5-4.5 mg/dL).
- PTH: Regulates Ca & PO₄.
- Vitamin D: 25(OH)D (status, <20 ng/mL deficiency); 1,25(OH)₂D (active).
- Alkaline Phosphatase (ALP): Bone-specific, osteoblast activity.
- Bone Turnover Markers (BTMs):
- Resorption: CTX, NTX.
- Formation: P1NP, Osteocalcin.
⭐ HbA1c reliability is ↓ with altered RBC lifespan (e.g., hemolytic anemia, CKD).
High‑Yield Points - ⚡ Biggest Takeaways
- Dynamic function tests (stimulation/suppression) are superior to basal levels for assessing endocrine reserve and autonomy.
- Free hormone assays (e.g., free T4) are generally preferred over total hormone levels, minimizing binding protein effects.
- 24-hour urine collections (e.g., for cortisol, metanephrines) account for variable secretion patterns like pulsatile or diurnal rhythms.
- Imaging (MRI, CT, USG) is for localization after biochemical diagnosis of endocrine dysfunction, not for screening.
- Specific autoantibody tests are crucial for diagnosing autoimmune endocrinopathies (e.g., Graves' disease, Hashimoto's thyroiditis).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

