Introduction & Principles - Fluid Foundations
- Body Fluid Compartments: Intracellular Fluid (ICF ~2/3), Extracellular Fluid (ECF ~1/3; interstitial, plasma).
- Osmolarity: Total solute concentration. Normal plasma osmolality: 275-295 mOsm/kg.
- Calculated: $2 \times [Na^+] + [Glucose]/18 + [BUN]/2.8$
- Tonicity: Effective osmolality; influences cell volume.
- Electrolyte Imbalance Causes: Abnormal intake, absorption, distribution, or excretion.
⭐ ECF volume is primarily determined by total body sodium content.
Sodium Imbalances - Salty Situations
Hyponatremia (Na+ < 135 mEq/L; Severe < 120 mEq/L): CNS symptoms (confusion, seizures). Max correction 8-10 mEq/L/24h.
⭐ Rapid correction of chronic hyponatremia can lead to Osmotic Demyelination Syndrome (ODS).
| Type | ECF Vol | UNa+ (mEq/L) | Causes | Management |
|---|---|---|---|---|
| Hypovolemic | ↓ | <20 / >20 | Diarrhea, diuretics | Isotonic saline |
| Euvolemic | Normal | >20 (often) | SIADH (📌Surgery, Intracranial, Alveolar, Drugs, Hormonal), polydipsia | Fluid restriction |
| Hypervolemic | ↑ | <20 / >20 | CHF, cirrhosis, nephrotic | Diuretics, Na+/H2O restrict |
- Causes: Water loss (Diabetes Insipidus, fever), Na+ gain (iatrogenic).
- Symptoms: Thirst, CNS (irritability, coma).
- Management: Correct water deficit. Water Deficit = $0.6 \times \text{Wt (kg)} \times [(\text{Serum Na}^+ / 140) - 1]$. Hypotonic fluids.
Potassium Imbalances - K-Drama Central
| Feature | Hypokalemia | Hyperkalemia |
|---|---|---|
| $K^+$ Levels | < 3.5 mEq/L; Severe < 2.5 mEq/L | > 5.0-5.5 mEq/L; Severe > 6.5 mEq/L |
| Causes | Diuretics, GI loss (vomiting/diarrhea), ↓intake, Alkalosis, Insulin excess | Renal failure, ACE-I/ARBs, K-sparing diuretics, Acidosis, Cell lysis (rhabdo, TLS), Addison's disease |
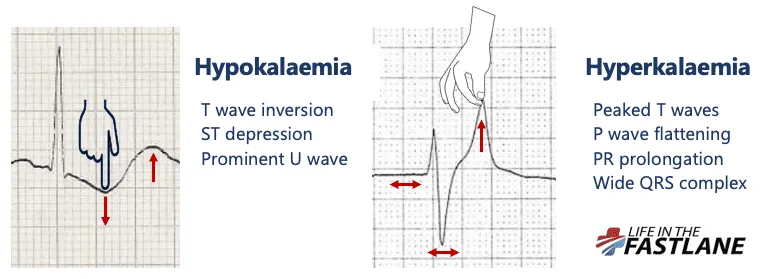
| ECG | U waves, T wave flattening/inversion, ST depression, ↑PR interval | Peaked T waves (earliest), ↑PR interval, Wide QRS, ↓P wave, Sine wave |
| Key Sx | Muscle weakness, fatigue, cramps, paralysis, constipation, arrhythmias | Muscle weakness, flaccid paralysis, paresthesias, arrhythmias, cardiac arrest |
| Management | Oral/IV KCl (IV: 10-20 mEq/hr; max 40 mEq/hr with monitoring). Correct Mg. | 📌 C BIG K DIE: Calcium gluconate (cardioprotection), Beta-agonists/Bicarb, Insulin+$C_6H_{12}O_6$ (shift $K^+$), Kayexalate, Diuretics/Dialysis (eliminate $K^+$) |
Calcium & Phosphate Imbalances - Bone & Beyond Buddies
- Hypocalcemia (Total Ca < 8.5 mg/dL; Ionized Ca < 4.65 mg/dL)
- Causes: Vitamin D deficiency, hypoparathyroidism, CKD.
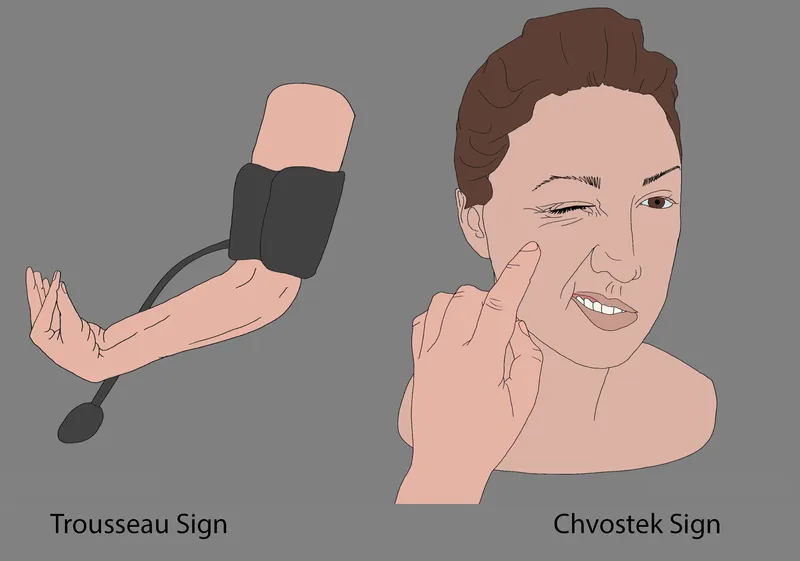
- Sx: Chvostek's, Trousseau's signs, tetany, paresthesias. ECG: QT prolongation.
- Corrected Ca: $Corrected Ca (mg/dL) = Measured Ca + 0.8 \times (4.0 - albumin (g/dL))$.
- Mgmt: IV Calcium gluconate (acute); Oral Ca/Vit D (chronic).
- Hypercalcemia (Total Ca > 10.5 mg/dL)
- Causes: Primary hyperparathyroidism, malignancy (e.g., PTHrP).
⭐ Malignancy and primary hyperparathyroidism are the two most common causes of hypercalcemia in adults.
- Sx: 📌 "Stones (renal calculi), bones (pain, fractures), groans (abdominal pain, constipation), thrones (polyuria, polydipsia), psychiatric overtones (confusion, fatigue)". ECG: Short QT interval.
- Mgmt: IV fluids, bisphosphonates, calcitonin.
- Causes: Primary hyperparathyroidism, malignancy (e.g., PTHrP).
- Phosphate Imbalances
- Hypophosphatemia (< 2.5 mg/dL): Causes (refeeding syndrome, antacids), muscle weakness, rhabdomyolysis. Mgmt: Oral/IV phosphate.
- Hyperphosphatemia (> 4.5 mg/dL): Causes (CKD, hypoparathyroidism), soft tissue calcification. Mgmt: Phosphate binders, dialysis.
- Ca-PO4 Relationship Highlights
Factor Serum Ca Serum PO4 PTH ↑ ↓ Vitamin D (active) ↑ ↑ CKD (severe) ↓ ↑
Magnesium Imbalances - Mighty Mag Moves
- Hypomagnesemia ($Mg^{2+}$ < 1.8 mg/dL or < 0.7 mmol/L)
- Causes: GI/renal loss, PPIs, alcohol.
- Features: Neuromuscular hyperexcitability (tetany, seizures), arrhythmias (📌 Torsades de Pointes - TdP). Often coexists with hypokalemia, hypocalcemia.
- Management: $MgSO_4$.
⭐ Hypomagnesemia can cause refractory hypokalemia and hypocalcemia because magnesium is a cofactor for potassium uptake and PTH release/action.
- Hypermagnesemia ($Mg^{2+}$ > 2.6 mg/dL or > 1.1 mmol/L)
- Causes: Renal failure, iatrogenic Mg administration.
- Features: ↓ DTRs, respiratory depression, hypotension, bradycardia, cardiac arrest.
- Management: IV calcium gluconate, dialysis.
High‑Yield Points - ⚡ Biggest Takeaways
- Hyponatremia (<135 mEq/L): SIADH common; rapid correction risks osmotic demyelination.
- Hypernatremia (>145 mEq/L): Free water loss (DI); slow correction prevents cerebral edema.
- Hypokalemia (<3.5 mEq/L): ECG (U waves, flat T), muscle weakness; potentiates digoxin toxicity.
- Hyperkalemia (>5.5 mEq/L): ECG (peaked T, wide QRS); Ca gluconate for cardiac protection.
- Hypocalcemia (<8.5 mg/dL): Tetany, Chvostek/Trousseau, prolonged QT.
- Hypercalcemia (>10.5 mg/dL): "Stones, bones, groans"; short QT.
- Hypomagnesemia: Causes refractory hypokalemia & hypocalcemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

