Chrono Basics - Time is Medicine
- Chronopharmacology: Study of how drug effects vary with biological timing and endogenous periodicities, optimizing therapy by timing drug administration.
- Key Concepts:
- Chronokinetics: Rhythmic changes in drug ADME (Absorption, Distribution, Metabolism, Excretion).
- Chronodynamics: Rhythmic changes in drug effects on the body.
- Chronesthesy: Rhythmic changes in target tissue sensitivity to drugs.
- Circadian Rhythm: Endogenous biological rhythms with a ~24-hour cycle, influencing drug action.
- Biological Clocks: Internal mechanisms regulating circadian rhythms.
- Suprachiasmatic Nucleus (SCN): The "master clock". 📌 SCN: 'Synchronizing Clock Nucleus'.
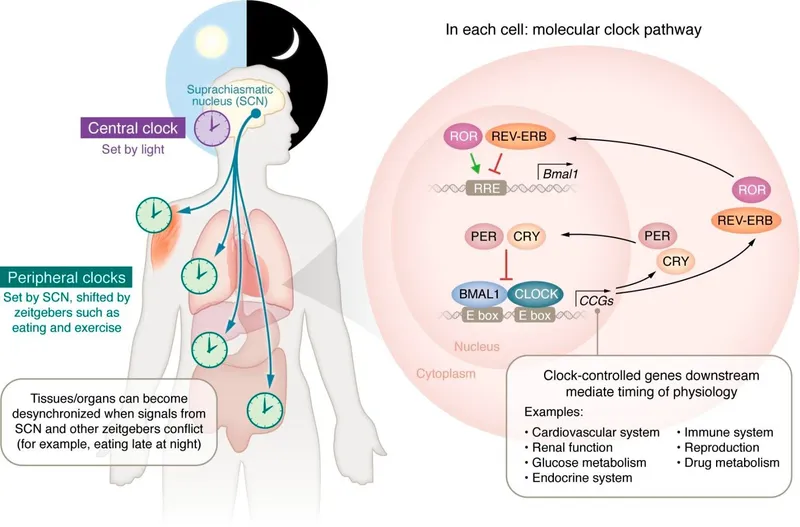
⭐ The Suprachiasmatic Nucleus (SCN) in the hypothalamus is the master circadian pacemaker synchronizing most bodily rhythms, including those relevant to drug action.
Drug Rhythms (ADME) - The Body Clock Effect
Circadian rhythms significantly impact drug efficacy/toxicity by modulating Pharmacokinetics (PK) & Pharmacodynamics (PD), affecting all ADME stages:
- Absorption (A): Gastric emptying, GI motility, blood flow, & P-glycoprotein in gut show daily rhythms, altering drug uptake.
- Distribution (D): Plasma protein binding, tissue perfusion, & P-glycoprotein activity vary, affecting drug distribution.
- Metabolism (M):
⭐ Hepatic metabolism, particularly via Cytochrome P450 enzymes (e.g., CYP3A4, CYP2D6), exhibits significant circadian variation, impacting the clearance of many drugs.
- Key enzyme (e.g., CYP450s, UGTs) expression/activity fluctuates, causing time-dependent metabolism.
- Excretion (E): Renal blood flow, GFR, & tubular functions vary, impacting drug elimination.
- Pharmacodynamics (PD): Receptor density, affinity, & signaling pathways oscillate, altering drug sensitivity.
Timed Therapies - Dosing by Daylight
Chronopharmacology involves timing drug administration to align with the body's circadian rhythms. This approach aims to maximize therapeutic efficacy and minimize adverse effects.
| Drug Class | Condition(s) | Optimal Timing | Rationale |
|---|---|---|---|
| ACEIs, ARBs | Hypertension | Evening/Bedtime | Counteracts morning BP surge; some studies show better CV outcomes. |
| Beta-blockers | Hypertension, Angina | Varies | Drug-specific; match to BP/HR patterns. |
| Statins | Hypercholesterolemia | Evening/Bedtime | 📌 Statins at Sunset: Cholesterol synthesis peaks at night. |
| NSAIDs | Osteoarthritis, RA | Evening/Bedtime | Reduces morning stiffness and pain. |
| Corticosteroids | Asthma, RA, Allergies | Morning | Mimics natural cortisol peak; minimizes adrenal suppression. |
| Bronchodilators (LABA) | Asthma, COPD | Evening | Prevents nocturnal/early morning bronchoconstriction. |
| H2 Blockers / PPIs | GERD, Peptic Ulcers | Evening/Bedtime | Gastric acid secretion is highest at night. |
| Chemotherapy Agents | Various Cancers | Varies | Drug-specific; targets cell cycle phases for ↑efficacy, ↓toxicity. |
Rx Timing Hurdles - Future Clock-Wise Care
- Hurdles:
- Inter-individual variability (e.g., chronotypes: larks/owls).
- Patient compliance with precise dosing schedules.
- Genetic influences impacting rhythmic drug effects.
- Future:
- Personalized chronotherapy tailoring.
- Smart drug delivery systems for controlled release.
⭐ Inter-individual variability in chronotypes (e.g., 'larks' vs. 'owls') poses a significant challenge to standardizing chronotherapeutic regimens.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronopharmacology: How drug effects vary with biological rhythms, aiming to optimize efficacy and reduce toxicity.
- Timed administration is key: corticosteroids (morning), statins (evening).
- NSAIDs (evening for RA), theophylline (evening for nocturnal asthma) show time-dependent benefits.
- Circadian rhythms affect drug ADME (absorption, distribution, metabolism, excretion) and receptor function.
- Chronotherapy is vital for drugs with narrow therapeutic windows or diseases with strong circadian patterns (e.g., asthma, hypertension).
- The SCN (Suprachiasmatic Nucleus) is the master clock governing these rhythms.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

