Microcirculation Structure - Tiny Tubes, Big Jobs
- Arterioles: "Resistance vessels"; smooth muscle controls diameter, regulating blood flow to capillaries. Major site of peripheral resistance.
- Capillaries: Smallest vessels (5-10 µm diameter); single endothelial layer + basal lamina. Site of nutrient/waste exchange.
- Types:
- Continuous: Most common (muscle, CNS, lungs). Tight junctions; pinocytotic vesicles.
- Fenestrated: Pores (fenestrae) for increased permeability (kidneys, intestines, endocrine glands).
- Sinusoidal (Discontinuous): Large intercellular gaps, incomplete basement membrane (liver, spleen, bone marrow).
- Types:
- Venules: Collect blood from capillaries; thin walls, less smooth muscle than arterioles. Post-capillary venules are key sites for inflammation & leukocyte extravasation.

⭐ Sinusoidal capillaries in the liver, spleen, and bone marrow have large gaps, allowing passage of large molecules and even cells.
Capillary Fluid Exchange - The Great Swap
- Governed by Starling forces: a balance between hydrostatic and colloid osmotic (oncotic) pressures across the capillary wall.
- Starling Equation: $J_v = K_f [ (P_c - P_i) - \sigma (\pi_c - \pi_i) ]$
- $J_v$: Fluid movement rate
- $K_f$: Filtration coefficient (capillary permeability & surface area)
- $P_c$: Capillary hydrostatic pressure (filtration ↑)
- $P_i$: Interstitial fluid hydrostatic pressure (opposes filtration if +ve)
- $\sigma$: Reflection coefficient (protein permeability; 0 to 1)
- $\pi_c$: Capillary oncotic pressure (absorption ↑)
- $\pi_i$: Interstitial fluid oncotic pressure (filtration ↑)
- Net Filtration Pressure (NFP): $(P_c - P_i) - (\pi_c - \pi_i)$ (assuming $\sigma=1$ for simplicity)
- NFP > 0: Net filtration (typically at arteriolar end)
- NFP < 0: Net absorption (typically at venular end)
- Lymphatic System: Crucial for returning excess filtered fluid and any leaked proteins from the interstitium back to the circulation.

⭐ Normally, there is a slight net filtration of fluid into the interstitium, which is then returned to circulation by the lymphatic system.
Microcirculation Regulation - Flow Control Masters
-
Goal: Match blood flow to tissue metabolic needs.
-
Key Players: Arterioles, metarterioles, precapillary sphincters.
-
Local (Intrinsic) Control: Dominant in vital organs (brain, heart).
- Myogenic: ↑Stretch → vasoconstriction; ↓Stretch → vasodilation.
- Metabolic: Active tissues release vasodilators (e.g., ↓O₂, ↑CO₂, ↑H⁺, ↑K⁺, adenosine).
- Endothelial-Derived Factors:
- Vasodilators: Nitric Oxide (NO), Prostacyclin (PGI₂).
- Vasoconstrictors: Endothelin-1.
⭐ Nitric Oxide (NO) is a potent endothelial-derived vasodilator crucial for local blood flow regulation.
- Extrinsic Control:
- Neural: Sympathetic (vasoconstriction via α₁; vasodilation in skeletal muscle via β₂/cholinergic).
- Hormonal:
- Vasoconstrictors: Angiotensin II, Vasopressin (ADH), Epinephrine (α-receptors).
- Vasodilators: Epinephrine (β₂-receptors), ANP.
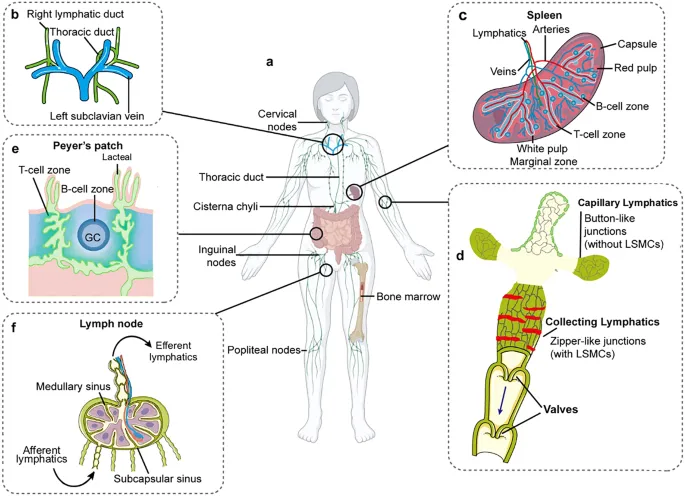
Lymphatic System - Fluid & Defense Drain
- Core Functions:
- Fluid Balance: Returns ~3L/day of excess interstitial fluid & proteins to blood, preventing edema.
- Fat Absorption: Lacteals in intestinal villi absorb dietary fats (chylomicrons).
- Immune Defense: Transports pathogens & immune cells to lymph nodes for immune response.
- Lymphatic Pathway & Propulsion:
- Propulsion: Skeletal muscle pump, respiratory movements, vessel smooth muscle contraction, one-way valves.
- Key Drainage:
⭐ The thoracic duct drains lymph from about 3/4 of the body, while the right lymphatic duct drains the remaining 1/4 (right upper quadrant).
- Clinical Note: Lymphedema: Chronic swelling from impaired lymphatic drainage.
High‑Yield Points - ⚡ Biggest Takeaways
- Starling forces (hydrostatic & oncotic pressures) dictate capillary fluid exchange.
- Capillary hydrostatic pressure (Pc) drives filtration; plasma oncotic pressure (πc) drives absorption.
- Lymphatics are crucial for returning excess interstitial fluid and protein, preventing edema.
- Capillary types: Continuous (muscle, CNS), Fenestrated (kidneys, gut), Sinusoidal (liver, spleen).
- Vasomotion is the intermittent flow via metarterioles & precapillary sphincters.
- Net Filtration Pressure (NFP) positive value indicates net fluid movement OUT of capillaries.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

