Exercise Energetics & O2 - Fueling Up
- O2 Consumption (VO2):
- Resting VO2: ~3.5 ml/kg/min (1 MET).
- VO2 max: Maximal O2 uptake; key fitness indicator.
- Fick Principle: $VO_2 = CO \times (CaO_2 - CvO_2)$.
- Energy Systems Timeline:
- ATP-PCr (Phosphagen): Immediate, ~10-15s.
- Anaerobic Glycolysis: Short-term, up to ~1-2 min.
- Aerobic (Oxidative): Long-term, dominant after ~2 min.
- Fuel Utilization: Carbohydrates for high-intensity; Fats for low-intensity, prolonged exercise.
- O2 Deficit & EPOC (Excess Post-exercise O2 Consumption).

⭐ VO2 max is widely regarded as the single best measure of cardiorespiratory fitness and endurance capacity.
Dynamic Exercise CV Changes - Heart Pumping Hard
Dynamic exercise triggers major CV adaptations:
- Key Adaptations:
- ↑HR: Sympathetic ↑, parasympathetic ↓; towards max (📌 $220 - age$).
- ↑SV: ↑Venous return (Frank-Starling), ↑contractility.
- ↑CO: $CO = HR \times SV$; ↑ significantly (4-8x).
- ↑SBP (workload-proportional); DBP stable/↓; ↑Pulse Pressure; ↑MAP ($MAP \approx DBP + \frac{1}{3}(SBP-DBP)$).
- ↓TPR: Dominant muscle vasodilation overrides systemic vasoconstriction.
- ↑a-vO2 diff: Muscles extract more O2; venous O2 content ↓.
⭐ During dynamic exercise, systolic BP increases proportionally to workload, while diastolic BP typically remains unchanged or slightly decreases due to vasodilation in active muscles, leading to a widened pulse pressure.
Comparison: Rest vs. Max Dynamic Exercise
| Parameter | Rest | Max Exercise |
|---|---|---|
| HR (bpm) | ~70 | ↑↑ ($220 - age## Dynamic Exercise CV Changes - Heart Pumping Hard |
Dynamic exercise triggers major CV adaptations:
- Key Adaptations:
- ↑HR: Sympathetic ↑, parasympathetic ↓; towards max (📌 $220 - age$).
- ↑SV: ↑Venous return (Frank-Starling), ↑contractility.
- ↑CO: $CO = HR \times SV$; ↑ significantly (4-8x).
- ↑SBP (workload-proportional); DBP stable/↓; ↑Pulse Pressure; ↑MAP ($MAP \approx DBP + \frac{1}{3}(SBP-DBP)$).
- ↓TPR: Dominant muscle vasodilation overrides systemic vasoconstriction.
- ↑a-vO2 diff: Muscles extract more O2; venous O2 content ↓.
⭐ During dynamic exercise, systolic BP increases proportionally to workload, while diastolic BP typically remains unchanged or slightly decreases due to vasodilation in active muscles, leading to a widened pulse pressure.
Comparison: Rest vs. Max Dynamic Exercise
) |
| SV (mL) | ~70 | ↑ (100-120+) |
| CO (L/min) | ~5 | ↑↑ (20-25+) |
| SBP (mmHg) | ~120 | ↑ (180-220) |
| DBP (mmHg) | ~80 | ↔ or ↓ |
| MAP (mmHg) | ~93 | ↑ (110-130) |
| TPR | High | ↓↓ |
| a-vO2 diff (mL/dL)| ~5 | ↑↑ (15-18) |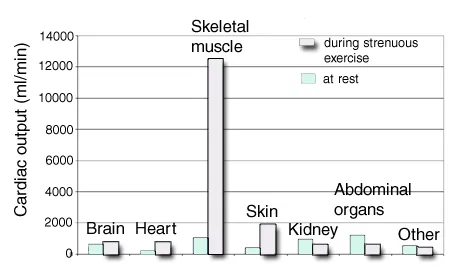
Static Exercise CV Changes - Pressure Challenge
- Nature: Primarily pressure load.
- Mechanisms:
- Mechanical compression of vessels.
- Strong sympathetic reflex.
- CV Response:
- HR: ↑ (moderate)
- SBP, DBP: ↑↑ (marked)
- MAP: ↑↑ (significant)
- CO: ↔ / ↓
- TPR: ↑↑ (significant)
⭐ Static (isometric) exercise causes a disproportionate rise in both systolic and diastolic blood pressure (pressor response) primarily due to mechanical compression of blood vessels within contracting muscles and a strong reflex sympathetic stimulation.
Training & Stress Response - Adapt & React
- Athlete's Heart (Physiological Adaptation):
- Long-term endurance training → cardiac remodeling.
- Key changes: Eccentric Left Ventricular (LV) hypertrophy, ↑ Stroke Volume (SV), ↓ Resting Heart Rate (HR), ↑ cardiac efficiency.
- 📌 Mnemonic: "SHE" - Stroke volume high, Heart rate low, Eccentric hypertrophy.
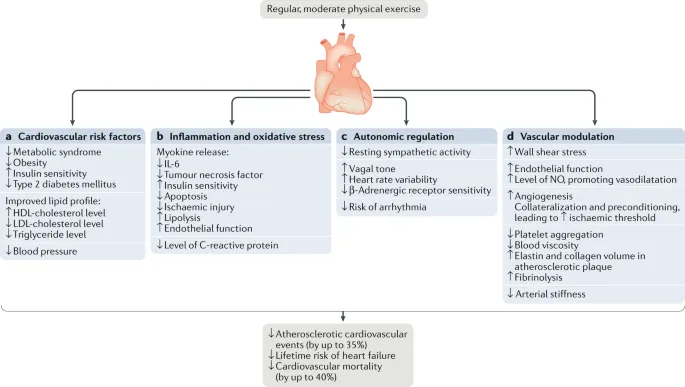
⭐ Athlete's heart is a physiological adaptation characterized by eccentric left ventricular hypertrophy, increased stroke volume, and lower resting heart rate, enhancing cardiac efficiency.
- Psychological Stress Response (Acute):
- Sympathetic activation → ↑ catecholamines.
- Cardiovascular effects: ↑ HR, ↑ Blood Pressure (BP), ↑ contractility.
- Regular exercise can attenuate adverse cardiovascular responses to stress, improving resilience.
CV Control Mechanisms - Brain & Body Talk
- Central Command: Anticipatory signals from higher brain centers (motor cortex, limbic system) initiate CV changes.
- Reflex Control:
- Baroreflex: Modulated (reset) to allow ↑Blood Pressure during exercise.
- Chemoreflex: Senses blood gas changes ($P_O2$, $P_{CO2}$, pH).
- Ergoreflex (Muscle work): Mechanoreceptors (contraction) & metaboreceptors (metabolites) signal CNS.
- Hormonal Modulation: Catecholamines (adrenaline, noradrenaline) ↑cardiac output; RAAS influences volume.
- Local Muscle Factors: Autoregulation via vasodilators ($NO$, adenosine, $K^+$) matches blood flow to metabolic demand.
⭐ Central command, originating from higher brain centers, initiates cardiovascular adjustments at the very onset of exercise, often before significant metabolic changes occur in the muscles.

High‑Yield Points - ⚡ Biggest Takeaways
Error: Failed to generate content for this concept group.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

