Hypoxia: Classification & Causes - Breathless States
- Hypoxia: Reduced O₂ availability at tissue level.
- Types & Causes:
- Hypoxemic Hypoxia: ↓$P_aO_2$.
- ↓Inspired $F_iO_2$ (high altitude)
- Hypoventilation (COPD, opioids)
- V/Q mismatch (PE, pneumonia)
- Shunt (cardiac defects)
- Diffusion impairment (ILD)
- Anemic Hypoxia: ↓O₂ carrying capacity of blood.
- Anemia (↓Hb)
- CO poisoning
- Methemoglobinemia
- Stagnant (Ischemic) Hypoxia: ↓Blood flow to tissues.
- Shock, heart failure
- Local obstruction (e.g., thrombus)
- Histotoxic Hypoxia: Cells unable to utilize O₂ effectively.
- Cyanide (cytochrome oxidase inhibitor)
- Alcohol, narcotics
- Hypoxemic Hypoxia: ↓$P_aO_2$.
- Dyspnea: Subjective sensation of difficult breathing.
⭐ Cyanide poisoning (histotoxic hypoxia) causes increased venous oxygen tension as tissues fail to extract oxygen.
Oxygen Transport & OHDC - Hemoglobin's Haul
- O₂ transport: Dissolved (2%), Hb-bound (98%).
- Hb: 4 O₂ sites; cooperative binding.
- 1g Hb carries 1.34 mL O₂.
- Arterial O₂ content ($CaO_2$): $(Hb \times 1.34 \times SaO_2) + (PaO_2 \times 0.003)$.
- OHDC:
- Sigmoid shape (cooperative binding).
- P50: $PO_2$ at 50% Hb saturation (Normal: 26.6 mmHg).
- Right Shift (↓ Affinity, ↑O₂ release): ↑$PCO_2$, ↑H⁺(↓pH), ↑Temp, ↑2,3-DPG. 📌 CADET, face Right!
- Left Shift (↑ Affinity, ↓O₂ release): ↓$PCO_2$, ↓H⁺(↑pH), ↓Temp, ↓2,3-DPG, HbF, COHb, MetHb.
- Bohr Effect: ↑$CO_2$/H⁺ → right shift (O₂ unloading).
- Haldane Effect: DeoxyHb binds more $CO_2$ (facilitates $CO_2$ transport).
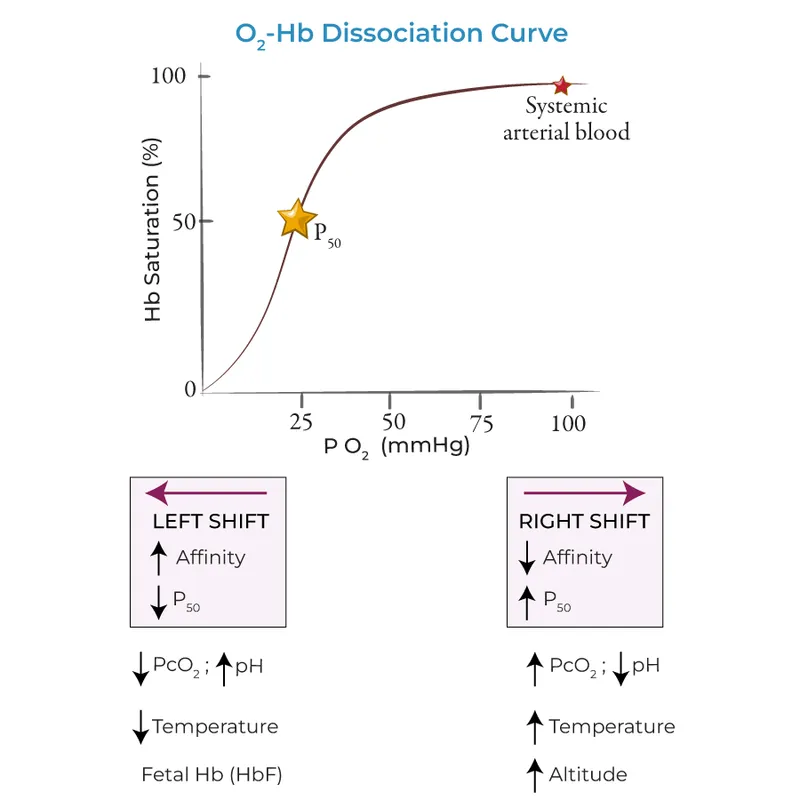
⭐ Fetal hemoglobin (HbF) has higher O₂ affinity (left-shifted curve, P50 ~19-20 mmHg) than adult HbA, aiding maternal O₂ uptake.
Systemic Effects of Hypoxia - Body Under Siege
- CNS: Highly sensitive. Confusion, impaired judgment, ataxia. Severe (PaO₂ < 30 mmHg): Loss of Consciousness (LOC).
- Cardiovascular System (CVS):
- Acute: ↑Heart Rate (HR), ↑Cardiac Output (CO) due to sympathetic drive. Severe/prolonged: Bradycardia, ↓Blood Pressure (BP), arrhythmias.
- Chronic: Pulmonary hypertension, Right Ventricular Hypertrophy (RVH).
- Respiratory System:
- Acute: Hyperventilation (Hypoxic Ventilatory Response - HVR) → Respiratory alkalosis.
- Chronic: Blunted HVR, especially in high-altitude natives.
- Hematologic: Chronic: ↑Erythropoietin (EPO) from kidneys → Polycythemia (Hematocrit > 55%).
- Cellular: Shift to anaerobic glycolysis → ↑Lactic acid production.
⭐ Cyanosis (bluish discoloration of skin & mucous membranes) typically becomes apparent when the mean capillary concentration of deoxygenated hemoglobin exceeds 5 g/dL.
an
Acclimatization to Altitude - Summit Strategy

- Goal: Maximize $O_2$ delivery & utilization for extreme altitudes over weeks/months.
- Hematological:
- ↑ EPO → ↑ RBC mass, Hb (Polycythemia).
- ↑ 2,3-DPG → Right shift ODC (aids $O_2$ unloading).
- Ventilatory:
- Sustained ↑ alveolar ventilation (HVR); peripheral chemoreceptors reset.
- Renal $HCO_3^-$ excretion compensates respiratory alkalosis.
- Cardiovascular & Tissue:
- Heart rate normalizes (vs. acute).
- ↑ Tissue capillarity, myoglobin, mitochondrial density, oxidative enzymes.
- Summit Strategy:
- "Climb high, sleep low"; gradual ascent.
- Staging: 2-3 weeks > 3000m before higher ascent.
- Supplemental $O_2$: Common > 7000m.
- Pharmacological aids:
- Acetazolamide: Aids acclimatization, prevents AMS.
- Dexamethasone: HACE/HAPE treatment.
- Sleep: Periodic breathing (Cheyne-Stokes) common.
⭐ The most important long-term acclimatization mechanism is increased hemoglobin concentration due to EPO stimulation.
High‑Yield Points - ⚡ Biggest Takeaways
- Hypoxic hypoxia (e.g., high altitude): ↓PaO2, ↓SaO2. Anemic hypoxia: ↓Hb, normal PaO2.
- OHDC Right Shift (↑P50, ↑O2 release): due to ↑H+, ↑CO2, ↑Temp, ↑2,3-DPG.
- Acclimatization: Hyperventilation, polycythemia, ↑2,3-DPG, ↑capillaries.
- CO Poisoning: Cherry-red skin, normal PaO2, ↓SaO2, strong left shift of OHDC.
- P50: PaO2 at 50% Hb saturation (normal 26.6 mmHg); reflects Hb-O2 affinity.
- Oxygen content (CaO2) primarily depends on Hb concentration and SaO2.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

