Altitude & Initial Responses - Thin Air Tango
High altitude: >2500m.
- Primary insult: ↓ Barometric pressure ($P_B$) $\implies$ ↓ Partial pressure of inspired $O_2$ ($P_I O_2$).
- $P_I O_2 = F_I O_2 \times (P_B - P_{H_2O})$
- Immediate Responses (Unacclimatized):
- Hypoxia: Peripheral chemoreceptors detect hypoxia.
- Hyperventilation (Hypoxic Ventilatory Response - HVR): ↑ Respiratory Rate (RR) & Tidal Volume (TV).
- → Respiratory alkalosis (↓ $P_a CO_2$, ↑ pH).
- Cardiovascular:
- ↑ Heart rate (HR), ↑ Cardiac Output (CO).
- Pulmonary vasoconstriction (Hypoxic Pulmonary Vasoconstriction - HPV) $\implies$ ↑ Pulmonary artery pressure.
- Cerebral vasodilation (maintains cerebral $O_2$ delivery).
- Fluid shifts: Potential for edema.
- 📌 Mnemonic: "THIN AIR" - Tachycardia, Hyperventilation, Increased CO, Nausea, Alkalosis (resp), Insomnia, Reduced $P_I O_2$.
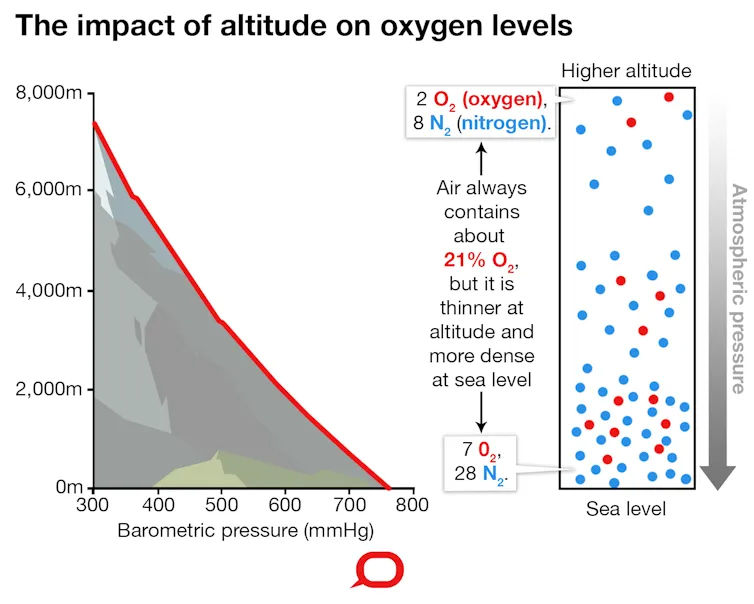
⭐ Hyperventilation, via peripheral chemoreceptors sensing hypoxemia, is the key initial response to high altitude exposure.
Ventilatory & Hematological Acclimatization - Breathing & Building
Ventilatory (Breathing):
- Trigger: Hypoxia (↓$P_aO_2$) sensed by peripheral chemoreceptors (carotid bodies).
- Response: Immediate ↑Ventilation (hyperventilation).
- Leads to: Respiratory alkalosis (↓$P_aCO_2$, ↑pH).
- Correction: Renal compensation (↑$HCO_3^-$ excretion over days) normalizes pH; hyperventilation persists.
- Key mediator: $HIF-1\alpha$ stabilization contributes to chemoreceptor sensitivity.
- Outcome: Sustained ↑Alveolar $P_{A}O_2$, improved $O_2$ uptake.
Hematological (Building):
- Trigger: Chronic hypoxia stimulates $HIF-1\alpha$.
- EPO Production: Kidneys release ↑Erythropoietin (EPO).
⭐ EPO levels peak within 24-48 hours of ascent to high altitude, but red cell mass increases take weeks.
- Erythropoiesis: ↑RBC production → ↑Hematocrit, ↑Hemoglobin (weeks).
- Outcome: ↑$O_2$ carrying capacity.
- $O_2$ Delivery: ↑2,3-DPG (2,3-Diphosphoglycerate) within hours-days.
- Effect: Right shift of Oxygen Dissociation Curve (ODC) → enhanced $O_2$ unloading to tissues.

Cardiovascular, Tissue & Cellular Adaptations - System & Cell Shift
- Cardiovascular:
- Cardiac Output (CO): Normalizes (post-initial ↑); Heart Rate (HR) slightly ↑, Stroke Volume (SV) ↓.
- Pulmonary Artery Pressure: Persists ↑ → Right Ventricular (RV) Hypertrophy.
- Blood Volume & Red Blood Cell (RBC) Mass: ↑ (due to Erythropoietin - EPO) → ↑Hematocrit (Hct), ↑Hemoglobin (Hb) (Polycythemia).
- Blood Viscosity: ↑.
- Tissue & Cellular:
- Capillarization: ↑ in muscles, brain (VEGF-driven).
- Myoglobin: ↑ in muscle cells (↑O2 storage).
- Mitochondria: ↑ number & density.
- Oxidative Enzymes: ↑ activity.
- 2,3-Diphosphoglycerate (2,3-DPG): Stays ↑ → Oxygen Dissociation Curve (ODC) right shift (↑O2 unloading to tissues).
⭐ Polycythemia is a key long-term adaptation to chronic hypoxia, increasing O2 carrying capacity but also blood viscosity.
High‑Yield Points - ⚡ Biggest Takeaways
- Hypobaric hypoxia is the key trigger for all acclimatization processes.
- Hyperventilation (↑RR): immediate reflex, causes respiratory alkalosis, ↑PaO2.
- ↑ Erythropoietin (EPO) from kidneys: stimulates ↑ RBC mass (polycythemia) over weeks.
- ↑ RBC 2,3-DPG: shifts ODC to the right, promoting O2 unloading to tissues.
- Renal compensation: ↑ HCO3- excretion by kidneys, correcting respiratory alkalosis.
- Persistent hypoxic pulmonary vasoconstriction: can lead to pulmonary hypertension.
- Cellular adaptations: ↑ tissue capillary density, ↑ mitochondria, ↑ myoglobin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

