MoA & Classification - Steroid Superpowers
- Mechanism of Action (MoA): Potent anti-inflammatory.
- Genomic (slow): Bind cytosolic Glucocorticoid Receptors (GR) → complex to nucleus:
- ↑ Lipocortin-1 (Annexin A1) → inhibits $PLA_2$ → ↓ PGs, LTs.
- ↓ Pro-inflammatory genes ($NF-\kappa B$, AP-1 blocked).
- Non-Genomic (rapid): Via membrane GRs.
- Genomic (slow): Bind cytosolic Glucocorticoid Receptors (GR) → complex to nucleus:
- Types: Glucocorticoids (anti-inflammatory) vs. Mineralocorticoids (salt-retaining). Focus: Glucocorticoids.
- Classification (Glucocorticoids):
- Systemic (Oral/IV):
- Short (8-12h): Hydrocortisone.
- Intermediate (12-36h): Prednisolone, Methylprednisolone.
- Long (36-72h): Dexamethasone.
- Inhaled (ICS): Beclomethasone, Budesonide, Fluticasone (local action, ↓ systemic SEs). 📌 Potency: Hydrocortisone (1) < Prednisolone (4) < Methylprednisolone (5) < Dexamethasone (25).
- Systemic (Oral/IV):
⭐ Corticosteroids upregulate $\beta_2$-adrenergic receptors, enhancing bronchodilator responsiveness.
Inhaled Corticosteroids (ICS) - Puff Power
- Common ICS: Beclomethasone, Budesonide, Fluticasone, Ciclesonide, Mometasone.
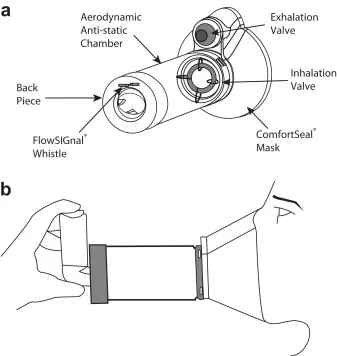
- Delivery Devices:
- MDI: Adv: Portable. Disadv: Needs coordination. Spacer improves delivery, ↓ local S/E.
- DPI: Adv: Breath-actuated. Disadv: Needs good inspiratory flow.
- Nebulizers: Adv: For severe attacks/uncooperative patients. Disadv: Less portable.
- Pharmacokinetics:
- High first-pass metabolism (e.g., Fluticasone, Budesonide) crucial for low systemic effects.
- Ciclesonide: Prodrug activated in lungs, minimizing local and systemic side effects.
- Local Side Effects & Prevention:
- Oropharyngeal candidiasis (thrush), dysphonia (hoarseness).
- Prevention: Use spacer with MDI; rinse mouth thoroughly with water and spit after inhalation.
⭐ Ciclesonide is a prodrug activated in the lungs, minimizing local side effects like candidiasis.
Systemic Steroids: Indications - System Savers
Systemic corticosteroids (Oral - OCS; Intravenous - IVCS) are vital for managing acute and severe respiratory conditions.
-
Core Indications (OCS/IVCS):
- Acute Severe Asthma: Rapidly reduces airway inflammation and obstruction.
- COPD Exacerbations: Shortens recovery time, improves FEV1 & PaO2, reduces relapse risk.
- Chronic Severe Asthma (Refractory): For patients not controlled on high-dose ICS/LABA.
- Sarcoidosis: Symptomatic pulmonary disease (e.g., Stage II/III with significant symptoms/lung function impairment).
- Interstitial Lung Diseases (ILDs):
- Cryptogenic Organizing Pneumonia (COP)
- Nonspecific Interstitial Pneumonia (NSIP) (especially cellular variant)
- ARDS (Acute Respiratory Distress Syndrome): Selected cases (e.g., early moderate-severe ARDS, COVID-19 related), benefits controversial, dose & timing critical.
-
Dosing Principles & Examples:
- "Burst" Therapy (Acute Exacerbations):
- Prednisolone (Oral): 40-50 mg/day for 5-7 days (Asthma/COPD). No tapering needed for short courses.
- Longer Courses (>2-3 weeks): Gradual tapering is essential to prevent adrenal insufficiency.
- Route Selection:
- Oral (PO): Prednisolone is preferred if patient can tolerate oral intake.
- Intravenous (IV): Methylprednisolone (e.g., 60-128 mg/day in divided doses for severe asthma), Hydrocortisone (e.g., 100-200 mg IV stat then q6h for status asthmaticus). Use for severe cases or if unable to take orally.
- "Burst" Therapy (Acute Exacerbations):
⭐ For acute asthma exacerbations, oral corticosteroids are as effective as intravenous corticosteroids if the patient can tolerate oral intake and there are no concerns about absorption.
Flowchart: Steroid Use in Acute Asthma Exacerbation
Adverse Effects & Management - Steroid Alerts
| Effect Type | Adverse Effects | Prevention / Management |
|---|---|---|
| Local (ICS) | Oropharyngeal candidiasis, dysphonia, cough. | Spacer, mouth rinsing. |
| Systemic (OCS / High-dose ICS) | HPA axis suppression, Cushingoid features (📌 CUSHINGOID), osteoporosis, hyperglycemia, immunosuppression, cataracts, glaucoma, skin thinning, mood changes, PUD. | Lowest effective dose, shortest duration, calcium/Vit D, bone density monitoring, PPI if needed, regular check-ups. |
Key Cautions:
- Active untreated infections (esp. TB, fungal), live vaccines (with high dose systemic), peptic ulcer disease, uncontrolled diabetes/hypertension.
Steroid Withdrawal Syndrome:
- Abrupt cessation: fatigue, myalgia, arthralgia, hypotension. Taper dose.
⭐ Alternate day therapy with short-acting oral corticosteroids like prednisolone can reduce HPA axis suppression in long-term use.
High‑Yield Points - ⚡ Biggest Takeaways
- Inhaled Corticosteroids (ICS) like Budesonide & Fluticasone are first-line for persistent asthma.
- Systemic corticosteroids (e.g., Prednisolone) manage acute asthma/COPD exacerbations.
- MOA: Broad anti-inflammatory effects, ↓ cytokines & eosinophils.
- ICS adverse effects: Oral thrush, dysphonia; mitigate with spacer & mouth rinsing.
- Systemic risks: Hyperglycemia, osteoporosis, HPA axis suppression, immunosuppression.
- Budesonide is the safest ICS during pregnancy.
- Also indicated for ABPA and pulmonary sarcoidosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

