Osteoporosis Overview - Brittle Bones Battle
- Definition: Low bone mass & microarchitectural deterioration, leading to ↑ bone fragility. WHO diagnostic criterion: T-score ≤ -2.5.
- Major Risk Factors:
- Advanced age
- Postmenopausal status (↓ estrogen)
- Long-term corticosteroid use
- Smoking, excessive alcohol
- Goals of Therapy:
- Prevent fractures
- ↑ Bone Mineral Density (BMD)
- Reduce pain, maintain function
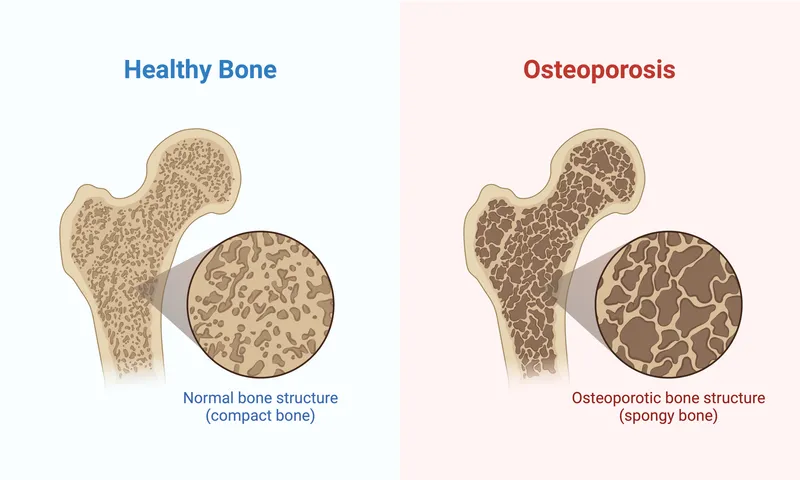
⭐ Most common osteoporotic fractures: vertebral, hip, and wrist.
Bisphosphonates - Mighty Mineral Binders
- MOA: Pyrophosphate analogs; bind hydroxyapatite in bone, inhibiting osteoclast activity and bone resorption.
- 📌 BPP: Bisphosphonates Prevent Pores.
- Key Agents:
- Oral: Alendronate, Risedronate, Ibandronate
- IV: Zoledronic acid, Pamidronate
- Oral Administration:
- Empty stomach (poor absorption).
- Full glass of plain water.
- Remain upright for 30-60 min (Alendronate/Risedronate 30 min; Ibandronate 60 min) to prevent esophagitis.
- Major ADRs:
- Esophagitis ⚠️ (oral)
- Osteonecrosis of the Jaw (ONJ)
- Atypical femoral fractures (long-term use)
- Hypocalcemia; Flu-like symptoms (IV)
- ⭐
Zoledronic acid is given once yearly IV for osteoporosis treatment.
 oka
oka
SERMs & Denosumab - Targeted Bone Defenders
| Feature | Raloxifene (SERM) | Denosumab |
|---|---|---|
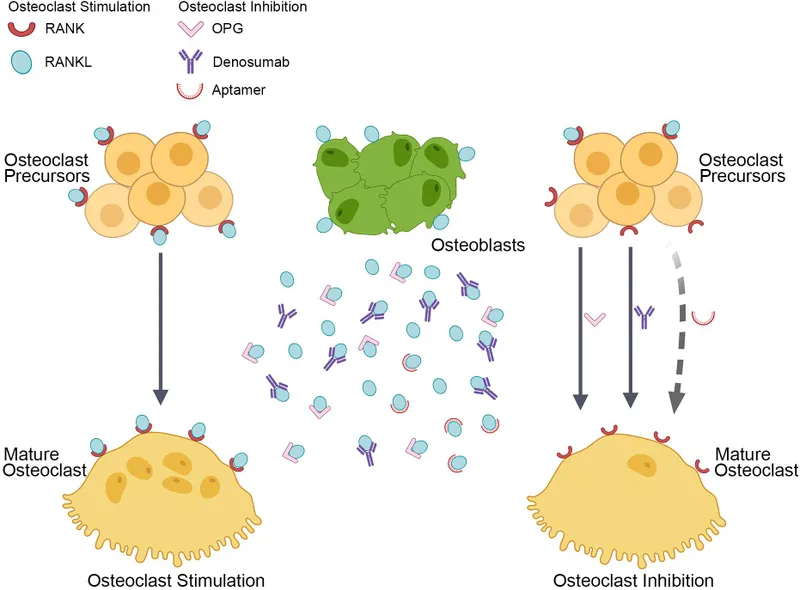
| MOA | Estrogen agonist on bone; antagonist on breast & uterus | MAb vs RANKL; inhibits osteoclast formation & survival |
| Benefits | ↓ Vertebral fractures; ↓ invasive breast cancer risk | Broad ↓ fracture risk (vertebral, hip, non-vertebral) |
| Admin | Oral | SC q6 months |
| Key ADRs | Hot flashes, ↑ VTE risk (DVT/PE) | Hypocalcemia, skin issues, ONJ, atypical femoral fractures |
| 📌 Mnemonic | Raloxifene: Risk (VTE) vs Reward (bone/breast) | Denosumab: Deactivates osteoclasts via RANKL Directly |
Anabolic Agents & Calcitonin - Bone Growth Boosters
-
Anabolic Agents: Stimulate new bone formation.
- Teriparatide, Abaloparatide: Recombinant PTH analogues.
- MOA: Intermittent exposure stimulates osteoblasts > osteoclasts, ↑ bone mass.
- Use: Severe osteoporosis, patients at high fracture risk. Max 2 years therapy.
- ADRs: Hypercalcemia, orthostatic hypotension, leg cramps.
- ⚠️ BBW: Osteosarcoma risk (rats); avoid in Paget's disease, prior skeletal radiation.
⭐ Teriparatide treatment should be followed by an anti-resorptive agent to maintain BMD gains.
- Teriparatide, Abaloparatide: Recombinant PTH analogues.
-
Calcitonin (Salmon):
- MOA: Directly inhibits osteoclasts, ↓ bone resorption; provides analgesic effect.
- Forms: Nasal spray, injection.
- Use: Limited efficacy for osteoporosis; mainly for pain relief from acute vertebral compression fractures.

High‑Yield Points - ⚡ Biggest Takeaways
- Bisphosphonates (e.g., Alendronate) are first-line agents, inhibiting osteoclast activity; key risks include ONJ and atypical femoral fractures. Specific administration is crucial.
- Denosumab, an anti-RANKL monoclonal antibody, potently inhibits osteoclast function; administered as an SC injection every 6 months.
- Teriparatide (recombinant PTH) is an anabolic agent that stimulates osteoblast activity and bone formation; reserved for severe osteoporosis.
- Raloxifene, a SERM, inhibits bone resorption; it increases the risk of DVT/PE but decreases the risk of invasive breast cancer.
- Romosozumab, an anti-sclerostin antibody, has a dual effect: it increases bone formation and decreases bone resorption.
- Adequate Calcium and Vitamin D supplementation is essential alongside all pharmacological therapies for osteoporosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

