Insomnia & Sleep Basics - Nighty Night Knots
- Sleep Architecture: NREM (N1, N2, N3/SWS-deep) & REM (dreams, atonia) cycle ~90 min.
- Neurotransmitters: Sleep ↑: GABA, Melatonin. Wake ↑: Histamine, Orexin.
- Insomnia: Difficulty initiating/maintaining sleep or early awakening.
- Chronic: ≥3 nights/week, ≥3 months, causing distress/impairment (DSM-5).
- Types: Sleep-onset, maintenance, early awakening.
- Non-Pharm (1st Line): CBT-I, sleep hygiene (e.g., regular schedule, avoid stimulants).

⭐ REM Sleep: "Paradoxical sleep" - active EEG, muscle atonia, vivid dreams.
Benzodiazepines (BZDs) - Calming the Chaos
- Mechanism of Action: Positive allosteric modulators of GABA-A receptors. They ↑ frequency of $Cl^-$ channel opening $\rightarrow$ ↑ $Cl^-$ influx $\rightarrow$ neuronal hyperpolarization $\rightarrow$ CNS depression.
- Classification (Primarily for Insomnia):
- Short-acting (1-6 hrs): Triazolam, Midazolam
- Intermediate-acting (6-24 hrs): Temazepam, Lorazepam, Alprazolam, Estazolam
- Long-acting (>24 hrs): Flurazepam, Diazepam, Clonazepam, Quazepam
- Pharmacokinetics:
- Generally lipid-soluble, well-absorbed orally.
- Metabolism: Hepatic (oxidation/conjugation). 📌 LOT (Lorazepam, Oxazepam, Temazepam) undergo direct conjugation (safer in elderly/liver disease as they bypass Phase I oxidative metabolism).
- Therapeutic Uses: Short-term relief of insomnia; also anxiolytic, anticonvulsant, muscle relaxant, alcohol withdrawal.
- Adverse Effects: Sedation, dizziness, ataxia, anterograde amnesia, psychomotor impairment. Tolerance, dependence, withdrawal syndrome (rebound insomnia, anxiety, seizures). ⚠️ Respiratory depression (esp. with alcohol/opioids). Paradoxical excitement.
- Contraindications: Myasthenia gravis, sleep apnea, severe respiratory insufficiency, pregnancy (Floppy Infant Syndrome), history of substance abuse, acute narrow-angle glaucoma.
- Antidote: Flumazenil.
⭐ Flumazenil: A competitive antagonist at BZD binding sites on the GABA-A receptor. It reverses BZD-induced sedation and overdose effects. Short half-life may require repeated doses.
Z-Drugs (Non-BZD Hypnotics) - Zzz's Select Agents
- Examples: Zolpidem, Zaleplon, Zopiclone, Eszopiclone. 📌 ZZZ-Es.
- MoA: Selective BZ1 (α1-GABA-A) agonists $\rightarrow$ ↑Cl⁻ influx.
- Kinetics: Rapid onset; short $t_{1/2}$ (Zaleplon ~1h); CYP3A4 metabolism.
- Pros (vs BZDs): ↓ sleep architecture change, ↓ tolerance/dependence, ↓ rebound insomnia.
- AEs: Headache, dizziness, GI upset; next-day drowsiness (↓ Zaleplon); ⚠️ complex sleep behaviors (Zolpidem); bitter taste (Zopiclone/Eszopiclone).
| Drug | $t_{1/2}$ | Use | Note |
|---|---|---|---|
| Zolpidem | 2-3h | Onset/Maint. | ⚠️ Complex sleep behaviors; max 10mg |
| Zaleplon | ~1h | Onset | Least next-day sedation |
| Zopiclone | 5-6h | Onset/Maint. | Bitter taste |
| Eszopiclone | 6h | Onset/Maint. | Bitter taste (S-isomer) |
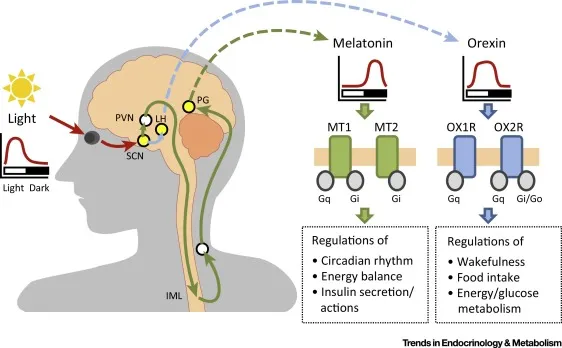
Melatonin & Orexin Modulators - Rhythm & Rest Agents
- Melatonin Agonists: Ramelteon, Tasimelteon
- Mechanism: Selective agonists at MT1 & MT2 melatonin receptors.
- Uses: Ramelteon for sleep-onset insomnia; Tasimelteon for non-24-hour sleep-wake disorder (often in blind individuals).
- Advantages: No abuse potential, no rebound insomnia or withdrawal symptoms.
⭐ Ramelteon is notably not a DEA scheduled controlled substance.
- Orexin Receptor Antagonists (DORAs): Suvorexant, Lemborexant, Daridorexant
- Mechanism: Block orexin A & B binding to OX1R & OX2R, suppressing wakefulness.
- Uses: Effective for both sleep-onset and sleep-maintenance insomnia.
- Adverse Effects: Somnolence, headache, abnormal dreams; ⚠️ High doses may cause sleep paralysis or cataplexy-like symptoms.
 oka
oka
Adjunctive Sedatives - Borrowed Bedtime Boosters
- Sedating Antidepressants:
- Doxepin (low-dose TCA; H1 block for sleep maintenance).
⭐ Low-dose Doxepin (3-6 mg) is FDA-approved for sleep maintenance.
- Trazodone (SARI; H1 & 5-HT2A block).
- Mirtazapine (NaSSA; H1 block).
- Doxepin (low-dose TCA; H1 block for sleep maintenance).
- Antihistamines (1st-gen): Diphenhydramine, Doxylamine (H1 block). Issues: anticholinergic effects, tolerance, next-day sedation.
- Others (Off-label/Caution): Gabapentinoids; low-dose Quetiapine (⚠️ side effects).
High‑Yield Points - ⚡ Biggest Takeaways
- Benzodiazepines (BZDs): Short-term insomnia; high dependence & withdrawal risk.
- Z-drugs (Zolpidem, Zopiclone): Act on BZ1 receptors; lesser dependence than BZDs; risk of complex sleep behaviors.
- Ramelteon: Melatonin agonist for sleep-onset insomnia; non-addictive.
- Suvorexant: Orexin receptor antagonist for sleep onset & maintenance.
- Antihistamines (e.g., Diphenhydramine): OTC sedation; significant anticholinergic side effects.
- Low-dose Doxepin (TCA): Approved for insomnia; watch for anticholinergic/cardiac effects.
- Barbiturates: Rarely used due to high abuse potential, narrow therapeutic index, and enzyme induction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

