Dementia Overview & Targets - Brain Fog Busters
- Dementia: Progressive neurocognitive decline; impairs memory, thinking, daily activities.
- Major Types:
- Alzheimer's Disease (AD): Most common.
- Vascular Dementia.
- Dementia with Lewy Bodies (DLB).
- Key Drug Targets (Primarily AD):
- Cholinergic deficit: ↓ Acetylcholine (ACh).
- Glutamatergic excitotoxicity: ↑ NMDA receptor activity.
- Pathological proteins: Amyloid-β (Aβ) plaques & Tau neurofibrillary tangles (NFTs).

⭐ Alzheimer's Disease accounts for approximately 60-80% of all dementia cases.
Cholinesterase Inhibitors - Memory Menders
- Mechanism: Reversibly inhibit acetylcholinesterase (AChE) → ↑ acetylcholine (ACh) levels in brain → improve cholinergic transmission.
- Primarily symptomatic relief; do not alter disease progression.
- Indications:
- Mild to moderate Alzheimer's Disease (AD).
- Donepezil also for severe AD.
- Rivastigmine also for Parkinson's Disease Dementia (PDD).
- Key Drugs: 📌 "Don Riva dances Gaily" (Donepezil, Rivastigmine, Galantamine)
- Donepezil (Aricept):
- Once daily dosing (long t½).
- Metabolized by CYP2D6 & CYP3A4.
- Rivastigmine (Exelon):
- Inhibits both AChE & Butyrylcholinesterase (BuChE).
- Available as oral & transdermal patch (↓ GI side effects).
- Galantamine (Reminyl):
- Dual mechanism: AChE inhibition & nicotinic receptor modulation.
- Metabolized by CYP2D6 & CYP3A4.
- Donepezil (Aricept):
- Common Side Effects (Cholinergic):
- GI: Nausea, vomiting, diarrhea (most common).
- CNS: Insomnia, dizziness, headache.
- CV: Bradycardia, syncope. ⚠️ Caution in patients with cardiac conduction defects or sick sinus syndrome.
- Drug Interactions:
- Anticholinergics (↓ efficacy).
- Beta-blockers (↑ risk of bradycardia).
- CYP inhibitors/inducers for donepezil & galantamine.
⭐ Rivastigmine is unique as it inhibits both acetylcholinesterase (AChE) and butyrylcholinesterase (BuChE), and its transdermal patch formulation improves tolerability by reducing gastrointestinal side effects.

NMDA Antagonists - Excitotoxicity Erasers
- Memantine: Key drug. 📌 MEMAntine aids MEMOry by blocking NMDA overactivity.
- Mechanism: Non-competitive NMDA receptor antagonist.
- Blocks pathological glutamate overstimulation.
- Reduces excessive $Ca^{2+}$ influx, ↓ excitotoxicity & neuronal damage.
- Low affinity, voltage-dependent: spares physiological receptor function.
- Indication: Moderate to severe Alzheimer's Disease.
- Monotherapy or adjunct to AChE inhibitors.
- Dosing: Start 5 mg/day; titrate weekly to 10 mg BID (max 20 mg/day).
- Side Effects: Generally mild; dizziness, headache, confusion.

⭐ Memantine uniquely targets the glutamatergic pathway in Alzheimer's, complementing cholinergic therapies.
Novel Dementia Therapies - Amyloid Annihilators
- Focus: Reduce Aβ plaque burden in early Alzheimer's Disease (AD).
- Mechanism: Monoclonal antibodies (mAbs) targeting various Aβ species.
- Key Drugs & Targets:
- Aducanumab (Aduhelm): Targets aggregated Aβ forms (plaques).
- FDA accelerated approval; use is limited.
- Lecanemab (Leqembi): Targets soluble Aβ protofibrils.
- Slows cognitive decline by 27% (CDR-SB over 18 months).
- Full FDA approval for early AD.
- Donanemab: Targets N-terminal pyroglutamate Aβ (N3pG Aβ) in plaques.
- Phase 3 trials show significant plaque clearance and clinical benefit.
- Aducanumab (Aduhelm): Targets aggregated Aβ forms (plaques).
- Major Side Effect Profile:
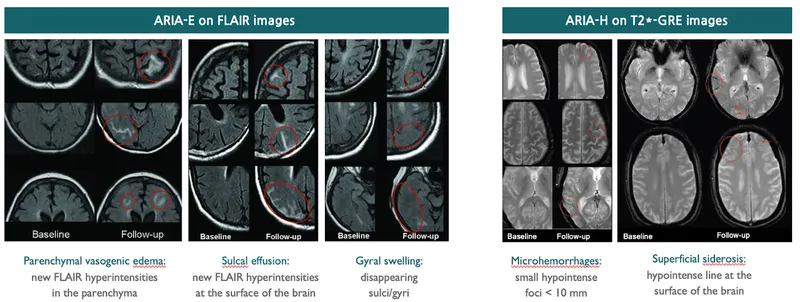
- Amyloid-Related Imaging Abnormalities (ARIA):
- ARIA-E: Vasogenic edema or sulcal effusions.
- ARIA-H: Microhemorrhages or superficial siderosis.
- Requires regular MRI monitoring, especially during initiation.
- Amyloid-Related Imaging Abnormalities (ARIA):
⭐ Lecanemab is the first anti-amyloid antibody to receive full FDA approval demonstrating both amyloid plaque reduction and a statistically significant slowing of clinical decline in early AD.
- Indicated for mild cognitive impairment (MCI) or mild dementia stage of AD with confirmed amyloid pathology.
High‑Yield Points - ⚡ Biggest Takeaways
- Acetylcholinesterase inhibitors (AChEIs) like Donepezil, Rivastigmine, Galantamine are first-line for mild-moderate Alzheimer's.
- Memantine, an NMDA antagonist, treats moderate-severe Alzheimer's, often combined with AChEIs.
- AChEIs commonly cause GI side effects; Rivastigmine patch may reduce these.
- Memantine works by blocking glutamate excitotoxicity.
- Current drugs offer symptomatic relief, not a cure for dementia.
- Avoid anticholinergics with AChEIs due to opposing mechanisms.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more