Iron Physiology - Rusty Regulation
- Absorption: Duodenum (Fe²⁺ via DMT1); basolateral export via Ferroportin.
- Transport: Transferrin carries Fe³⁺ in blood.
- Storage: Ferritin (main, soluble), Hemosiderin (insoluble, excess).
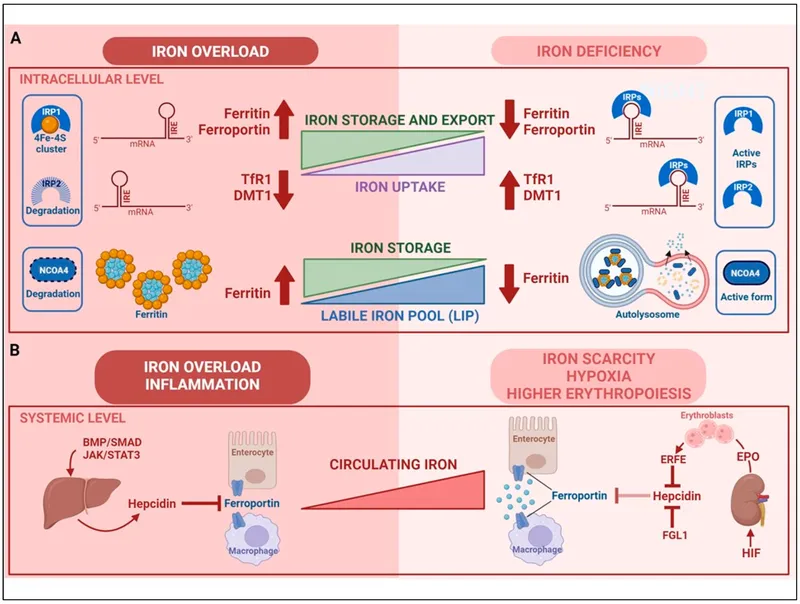
- Regulation: Hepcidin (liver hormone) is the master regulator.
- ↑ Hepcidin: Blocks ferroportin → ↓ iron absorption & macrophage release.
- ↓ Hepcidin: Facilitates iron absorption & release (stimulated by iron deficiency, ↑ erythropoiesis).
- Daily Loss: ~1 mg (GI, skin); menstruation adds. 📌 "Rusty pipes lose a bit daily."
⭐ Hepcidin levels are ↑ in inflammation (e.g., anemia of chronic disease), leading to functional iron deficiency.
Iron Deficiency Anemia - Empty Tanks
- Depleted iron stores → impaired Hb synthesis. Commonest nutritional anemia.
- Causes: Chronic blood loss (GIT/Gynae), ↓intake/absorption, ↑demand (pregnancy, growth).
- Features: Fatigue, pallor, glossitis, koilonychia (spoon nails), pica.
- Labs:
- CBC: ↓Hb, ↓MCV (<80fL), ↓MCH, ↓MCHC.
- Iron Profile: ↓Serum Fe, ↓Ferritin (<30ng/mL), ↑TIBC, ↓Transferrin Saturation (<16%).
- Smear: Microcytic hypochromic RBCs, pencil cells.

⭐ Serum ferritin: best indicator of iron stores; ↓ in IDA before Hb changes.
Oral Iron Therapy - Pill Power Up
- Goal: Correct IDA, replenish iron stores.
- Preparations (Ferrous salts preferred): 📌 "Us" (Ferrous) > "Ic" (Ferric).
- Ferrous Fumarate (33% elemental Fe), Ferrous Sulfate (most common, 20% elemental Fe), Ferrous Gluconate (12% elemental Fe).
- Dose (Elemental Fe):
- Therapeutic: 100-200 mg/day (adults); 3-6 mg/kg/day (children).
- Prophylactic: 60 mg/day.
- Absorption: ↑ Vit C; ↓ food, antacids, phytates, tetracyclines. Best on empty stomach.
- Duration: 3-6 months post-Hb normalization to replenish stores.
- Monitoring & Response:
- ADRs: GI upset (nausea, constipation - common), dark stools (harmless).
⭐ Reticulocyte count is the earliest lab indicator of response to oral iron therapy, peaking in 7-10 days post-initiation.
Parenteral Iron Therapy - IV Iron Impact
- Indications: Oral iron failure/intolerance, severe malabsorption (IBD), CKD on ESAs, significant blood loss, need for rapid Hb ↑.
- Dosing: Total iron deficit calculated (e.g., Ganzoni: $Dose (mg) = BW (kg) \times (Target Hb - Actual Hb) \times 2.4 + Stores (mg)$).
- Common IV Preparations:
- Iron Sucrose: Safer, multiple doses. Max 200 mg/infusion.
- Ferric Carboxymaltose (FCM): Higher single doses (up to 1000 mg).
- Iron Dextran: ⚠️ Higher anaphylaxis risk; test dose.
- Impact: Rapid Hb ↑, improved symptoms, repletion of iron stores.
- Monitoring: Hb, Ferritin (4-8 weeks post-infusion).
⭐ FCM allows for Total Dose Infusion (TDI), replenishing iron stores in a single session for eligible patients.
Treatment & Monitoring - Refilling & Watching
- Oral Iron:
- Dose: 100-200 mg elemental Fe/day (e.g., ferrous sulfate), preferably on empty stomach.
- Duration: Normalize Hb, then 3-6 months for stores (Target: Ferritin >50 ng/mL).
- Monitor: Reticulocytes (peak 7-10d), Hb (↑ 1 g/dL/wk or 2g/dL/3wks).
- Parenteral Iron:
- Indications: Oral intolerance/failure, malabsorption, severe/ongoing loss, CKD.
- E.g., Iron sucrose, Ferric Carboxymaltose (FCM). Calculate total dose.
- ⚠️ Anaphylaxis risk (esp. high MW dextran; less with FCM, iron sucrose).
- Response Monitoring:
⭐ Parenteral iron: Ferric Carboxymaltose (FCM) allows for rapid, high-dose administration (up to 1000 mg Fe per session) via Total Dose Infusion (TDI), ideal for severe cases.
High‑Yield Points - ⚡ Biggest Takeaways
- Oral iron (ferrous salts: sulfate, fumarate) preferred; Vitamin C ↑ absorption, antacids/food ↓.
- Parenteral iron (iron sucrose, FCM) for malabsorption, severe intolerance, or rapid need.
- Iron dextran: highest anaphylaxis risk; test dose mandatory.
- Acute iron toxicity: GI distress, shock; antidote is deferoxamine.
- Chronic iron overload (hemochromatosis): liver/heart damage; manage with phlebotomy or deferasirox.
- Target Hb rise: ~1 g/dL/week with effective therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

