NSAIDs: The Basics - Pain & Fire Fighters
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Combat pain, inflammation, fever.
- Core Therapeutic Actions: 📌 "The 3 A's"
- Analgesic: Relieve mild-moderate pain (somatic > visceral).
- Anti-inflammatory: Reduce inflammation (redness, swelling, pain, heat).
- Antipyretic: Reduce fever (antipyresis).
- General Pharmacokinetics:
- Most are weak organic acids.
- Good oral absorption.
- High plasma protein binding (e.g., to albumin).
- Hepatic metabolism, renal excretion.
- Key Features:
- Mechanism: All inhibit cyclooxygenase (COX) enzymes.
- Common ADRs: GI irritation, peptic ulcers, renal adverse effects.
⭐ Aspirin is the prototype NSAID, unique for its irreversible COX inhibition and significant antiplatelet effect at low doses (e.g., 75-150 mg daily).
Mechanism of Action - Prostaglandin Power Down
- Core Action: NSAIDs inhibit Cyclooxygenase (COX) enzymes (COX-1 & COX-2).
- This blocks conversion of Arachidonic Acid (AA) to Prostaglandin H2 (PGH2).
- PGH2 is a precursor to Prostaglandins (PGs), Prostacyclin (PGI2), & Thromboxane A2 (TXA2).
- AA Source: Released from cell membrane phospholipids by Phospholipase A2 (PLA2).
- 📌 Corticosteroids inhibit PLA2, a step before NSAID action.
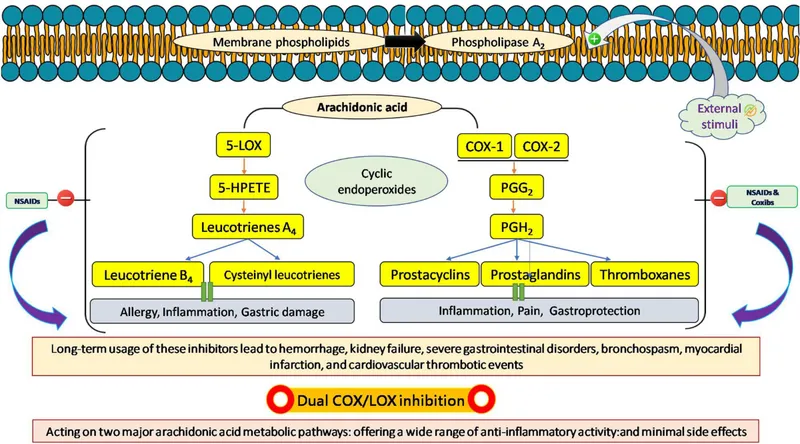
Simplified Arachidonic Acid Pathway & NSAID Action:
- Consequences of COX Inhibition:
- Therapeutic Effects:
- ↓ PGs → Analgesia (↓ pain), Antipyresis (↓ fever), Anti-inflammatory action.
- Adverse Effects (mainly via COX-1 inhibition):
- ↓ Gastric PGs (PGE2, PGI2) → Gastropathy, ulcers.
- ↓ Renal PGs → Na+/water retention, ↓ GFR, hypertension.
- ↓ Platelet TXA2 (COX-1) → Impaired hemostasis, ↑ bleeding time (esp. Aspirin - irreversible).
- Therapeutic Effects:
⭐ The primary mechanism of NSAIDs involves the inhibition of cyclooxygenase (COX) enzymes (COX-1 and COX-2), leading to decreased synthesis of prostaglandins and thromboxanes from arachidonic acid.
NSAID Classification - Selective Strategies
| Selectivity | Chemical Class | Examples | Key Points / Clinical Pearls |
|---|---|---|---|
| Non-selective (Inhibit COX-1 & COX-2) | Salicylates | Aspirin | Irreversible COX inhibitor. Low dose ($75-150$ mg) for antiplatelet effect. Main risk: GI toxicity, Reye's syndrome in children. |
| Propionic Acids | Ibuprofen, Naproxen | Reversible inhibitors. Good analgesic, antipyretic, anti-inflammatory. Moderate GI risk. Naproxen: longer half-life, considered CV safer by some. | |
| Acetic Acids | Diclofenac, Indomethacin, Ketorolac | Potent. Diclofenac: some COX-2 preference, ↑ liver enzyme risk. Indomethacin: potent, for gout, PDA closure; ↑ GI/CNS SE. Ketorolac: strong analgesic, short-term use (≤5 days). | |
| Preferential COX-2 (Higher affinity for COX-2) | Various (e.g., Sulfonanilides, Oxicams) | Nimesulide, Meloxicam, Etodolac | Better GI tolerance than non-selective. Nimesulide: hepatotoxicity risk ⚠️, banned in some countries. Meloxicam: for osteoarthritis, long t½. Etodolac: well-tolerated. |
| Selective COX-2 (Coxibs) (Specifically inhibit COX-2) | Coxibs | Celecoxib, Etoricoxib, Parecoxib (IV) | Significantly ↓ GI toxicity vs non-selective. Increased CV thrombotic risk (MI, stroke) due to unopposed TXA2. Sulfa allergy (Celecoxib). 📌 Mnemonic: "Celebrex Eats Pain" (for Celecoxib, Etoricoxib, Parecoxib). |
High‑Yield Points - ⚡ Biggest Takeaways
- NSAIDs inhibit COX enzymes, reducing prostaglandin synthesis to decrease pain and inflammation.
- COX-1 is constitutive (e.g., gastric cytoprotection); COX-2 is inducible by inflammatory stimuli.
- Aspirin is a unique irreversible COX inhibitor.
- Selective COX-2 inhibitors (e.g., Celecoxib) have ↓ GI toxicity but ↑ cardiovascular risk.
- Non-selective NSAIDs inhibit both COX-1 and COX-2 isoforms.
- Paracetamol: weak peripheral anti-inflammatory, primarily central analgesic/antipyretic effects.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

