Diagnosis & Classification - Wheezy Kid Clues
Look for: recurrent wheeze, cough (esp. nocturnal, exercise-induced), dyspnea. Family history of atopy/asthma is crucial.
- Key Diagnostic Criteria:
- Spirometry: FEV1/FVC ratio < 0.9 (children 6-11 yrs). Significant reversibility: ↑FEV1 >12% AND >200ml after SABA.
- PEFR (children): Diurnal variability >13%.
- Classification (GINA): Intermittent, Mild Persistent, Moderate Persistent, Severe Persistent (based on symptoms, nighttime awakenings, SABA use, FEV1).
⭐ In children <5 years, diagnosis is often clinical; a therapeutic trial of SABA/ICS can be diagnostic if symptoms improve and recur off-treatment.
Pharmacotherapy - Meds & Moves
Relievers (Quick Relief):
- Short-Acting Beta2-Agonists (SABA): Salbutamol, Levosalbutamol.
- Dose: 100-200 mcg (1-2 puffs) PRN.
- Low-dose ICS-Formoterol: Preferred GINA reliever (MART strategy).
Controllers (Long-term Prevention):
- Inhaled Corticosteroids (ICS): Budesonide, Fluticasone. Mainstay.
- SE: Candidiasis (rinse mouth), dysphonia.
- Long-Acting Beta2-Agonists (LABA): Salmeterol, Formoterol.
- ⚠️ Always use with ICS.
- 📌 Formoterol: Fast (for MART).
- Leukotriene Receptor Antagonists (LTRA): Montelukast (10mg OD).
- Theophylline: Narrow therapeutic index.
- Biologics (Severe Asthma): Anti-IgE (Omalizumab), Anti-IL5 (Mepolizumab).
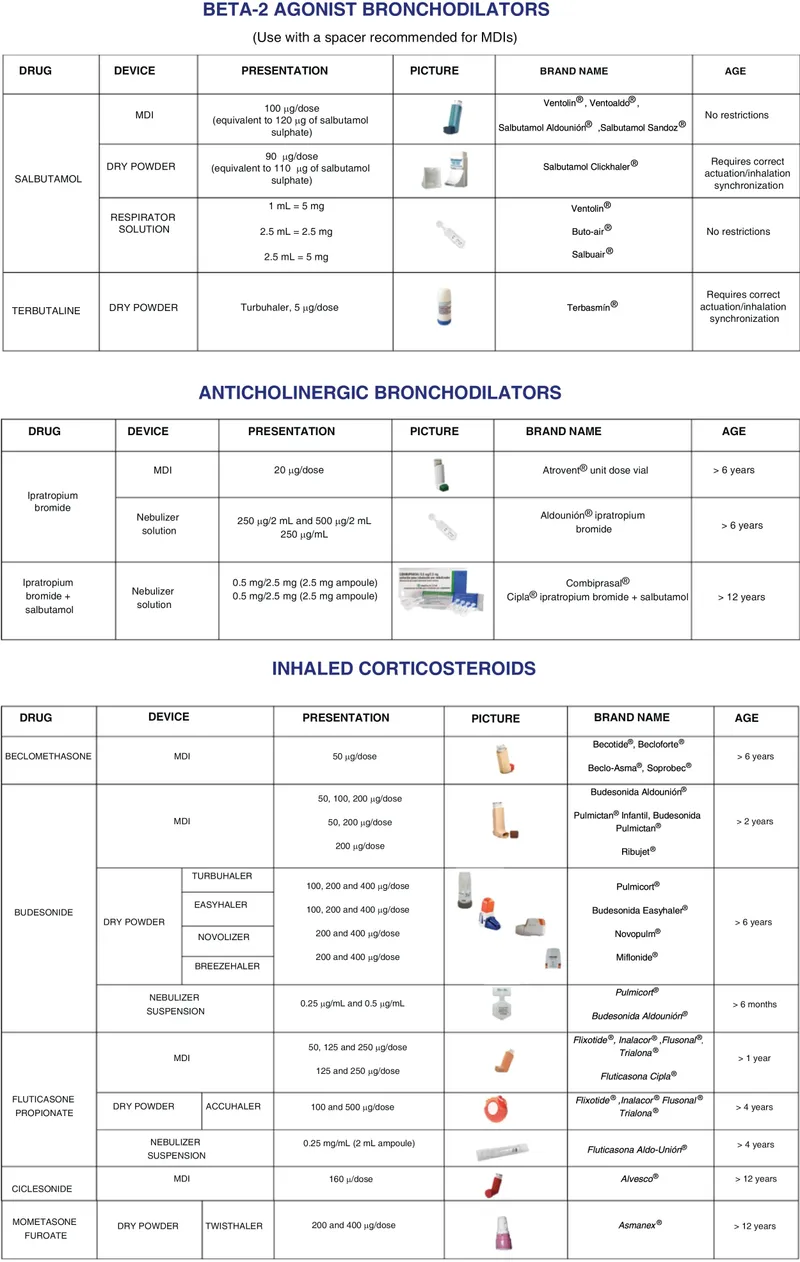
Delivery Devices:
- Metered Dose Inhaler (MDI) + Spacer (↑deposition, ↓SE).
- Dry Powder Inhaler (DPI).
- Nebulizer (acute severe exacerbations).
Stepwise Management (Simplified GINA Approach):
⭐ > Montelukast: rare neuropsychiatric events (agitation, sleep issues), esp. children.
Stepwise Management - The GINA Ladder
- Core Principle: Adjust treatment up or down for symptom control & risk reduction.
- GINA Preferred Pathway (Adults & Adolescents ≥12 years):
- Step 1: As-needed low-dose ICS-formoterol.
- Step 2: As-needed low-dose ICS-formoterol.
- Step 3: Low-dose ICS-formoterol (Maintenance And Reliever Therapy - MART).
- Step 4: Medium-dose ICS-formoterol (MART).
- Step 5: High-dose ICS-formoterol (MART). Add LAMA. Refer; consider biologics (e.g., anti-IgE).
- Review & Adjust: Assess 2-6 weeks post-change, then 3-12 monthly. Step down if stable 3 months.
⭐ > The use of ICS-formoterol as both maintenance and reliever (MART) in Steps 3-5 simplifies treatment and improves outcomes by providing rapid relief and anti-inflammatory action with each dose.
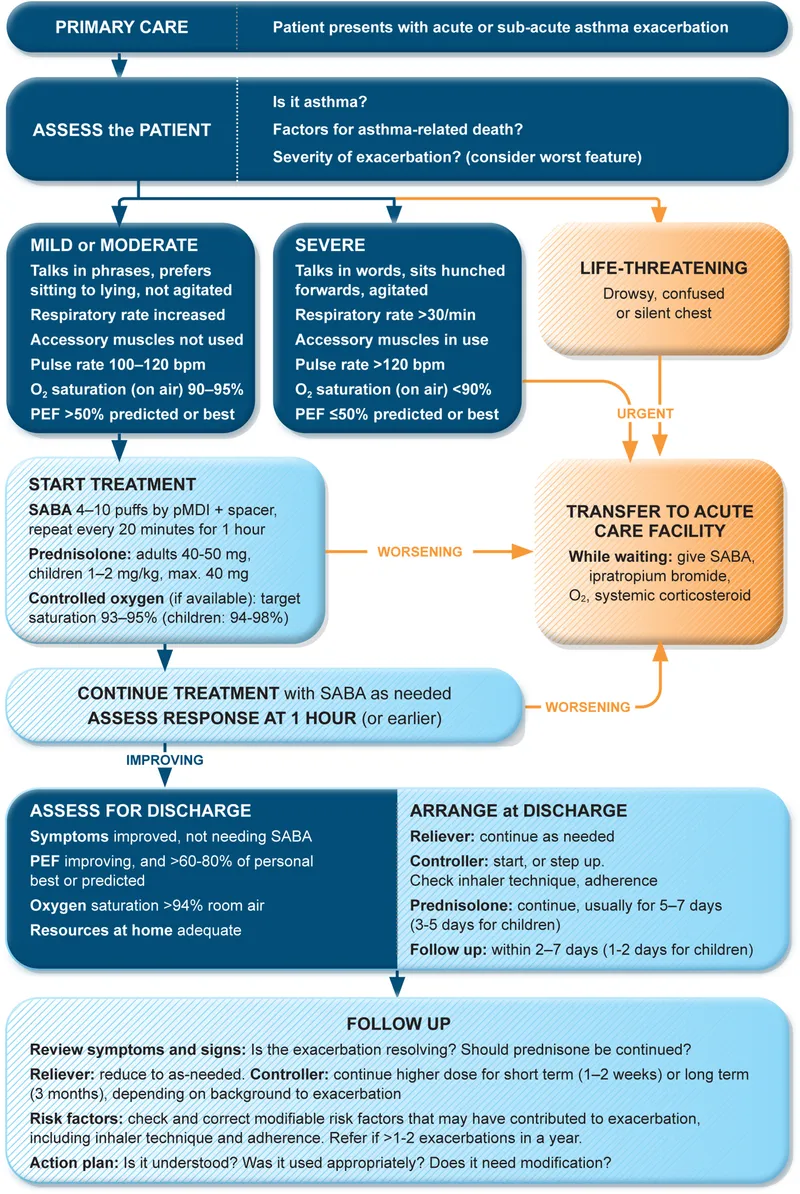
Acute Exacerbation - SOS Protocol
- Initial Actions (First Hour):
- Oxygen: Titrate to SpO2 > 92% (Children: 94-98%).
- SABA (Salbutamol): Nebulized 2.5-5mg (child: 0.15mg/kg) or MDI 4-10 puffs via spacer. Repeat q20min for 1st hour.
- Ipratropium Bromide: Add 0.5mg (child: 0.25mg) nebulized with SABA for moderate-severe cases.
- Systemic Corticosteroids: Oral Prednisolone 1-2mg/kg (max 40-60mg) or IV Hydrocortisone. Administer within 1 hour.
- Severe/Life-Threatening (or poor response):
- IV Magnesium Sulfate: 2g IV over 20 min (child: 25-75mg/kg, max 2g).
- Consider continuous SABA, ICU for monitoring/ventilation.
⭐ A "silent chest" in acute asthma is an ominous sign indicating severe airflow limitation and impending respiratory failure.
High‑Yield Points - ⚡ Biggest Takeaways
- Asthma management follows a stepwise approach (GINA guidelines).
- Short-Acting Beta Agonists (SABA) like Salbutamol are for acute symptom relief.
- Inhaled Corticosteroids (ICS) are the preferred long-term controller medication.
- Leukotriene Receptor Antagonists (LTRAs) like Montelukast are add-on/alternative therapy.
- Severe exacerbations require systemic corticosteroids, oxygen, and frequent nebulized SABA/Ipratropium.
- Peak Expiratory Flow Rate (PEFR) helps monitor asthma control and severity.
- Spacer devices are crucial for effective MDI drug delivery in children.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

