Celiac Disease - Gluten Gone!
- Immune reaction to gluten (proteins in wheat, rye, barley) causing small intestinal villous atrophy & malabsorption.
- Clinical Features:
- GI: Chronic diarrhea, failure to thrive (FTT), abdominal pain/distension.
- Non-GI: Iron deficiency anemia, short stature, dental enamel defects, dermatitis herpetiformis.
- Diagnosis:
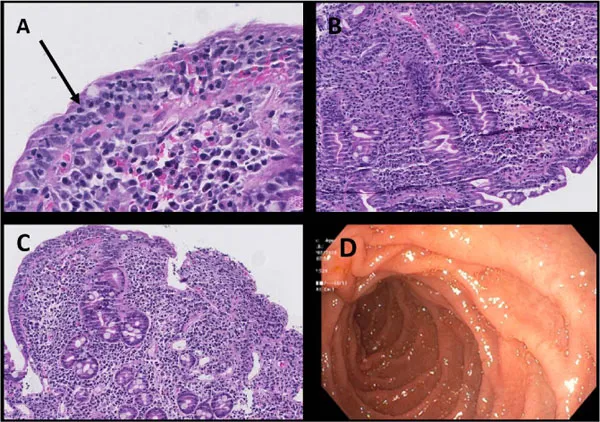
- Serology: IgA anti-tissue transglutaminase (Anti-tTG IgA) is the primary screening test. iv - Endoscopy with duodenal biopsy: Confirmatory; shows villous atrophy, crypt hyperplasia, increased intraepithelial lymphocytes.
- Management:
- Lifelong strict Gluten-Free Diet (GFD).
- Avoid: Wheat, Rye, Barley, and oats not certified gluten-free. (📌 BROW: Barley, Rye, Oats, Wheat).
- Allowed: Rice, corn, millets, quinoa, potatoes, fruits, vegetables.
- Monitor & supplement: Iron, folate, Vitamin D, calcium, B12.
⭐ Dermatitis herpetiformis, an intensely pruritic papulovesicular rash typically on extensor surfaces, is the specific cutaneous manifestation of celiac disease and responds to a GFD.
Cystic Fibrosis - CF Calorie Crusade
- Goal: Optimize nutrition, promote growth, prevent deficiencies.
- Energy: High needs: 110-200% of RDA.
- Diet: High-calorie, high-fat, high-protein. Unrestricted fat.
- PERT: Pancreatic Enzyme Replacement Therapy with all meals/snacks.
- Lipase: 500-2,500 U/kg/meal; max 10,000 U/kg/day or <4,000 U/g fat/day.
- Vitamins: Fat-soluble (A, D, E, K) supplementation. 📌 ADEK for CF's sake.
- Minerals: Salt supplementation, especially with ↑sweat loss (e.g., fever, hot weather).
- Monitoring: Growth (weight, height, BMI), stool (steatorrhea), annual vitamin levels.
⭐ Pancreatic insufficiency, seen in 85-90% of CF patients, mandates lifelong enzyme therapy.
IBD Nutrition - Gut Guardian Grub
- Goal: Induce/maintain remission, correct deficiencies, promote growth. Growth failure common; requires aggressive support.
- Crohn's Disease (CD) - Active:
- Exclusive Enteral Nutrition (EEN): First-line therapy.
- Duration: 6-8 weeks.
- Mechanism: ↓ inflammation, alters microbiome, mucosal healing.
- Polymeric formulas often used.
- 📌 EEN for Effective Eradication of Nasty CD flares.
- Exclusive Enteral Nutrition (EEN): First-line therapy.
- CD - Maintenance:
- Partial Enteral Nutrition (PEN).
- Specific diets (CDED, SCD) - emerging evidence.
- Ulcerative Colitis (UC):
- EEN less established; supportive nutrition crucial.
- Key Deficiencies: Monitor & replete Fe, Vit D, B12, Zn, Folate.
⭐ EEN is as effective as corticosteroids for inducing remission in pediatric Crohn's disease, with superior mucosal healing and fewer side effects.
setup for a child with Crohn's Disease)
CKD Nutrition - Kidney Care Kitchen
- Key Goals: Support growth, manage complications (uremia, acidosis, bone disease).
- Energy: Meet RDA for height-age; ↑ for catch-up growth.
- Protein (HBV):
- Pre-dialysis: RDA, may need moderate restriction (~0.8-1.0 g/kg/day).
- Dialysis: ↑ needs (1.0-1.5 g/kg/day).
- Sodium: Restrict (e.g., 1-3 mEq/kg/day or <2 g/day); individualize fluid.
- Potassium: Restrict if K$^+$ > 5.5 mEq/L. Avoid high-K foods.
- Phosphorus: Restrict; use phosphate binders. Target age-specific levels.
- Vitamins/Minerals:
- Active Vitamin D (e.g., Calcitriol).
- Iron, water-soluble vitamins (B, C, Folic acid).

⭐ Protein needs ↑ significantly on dialysis due to losses & increased catabolism.
High‑Yield Points - ⚡ Biggest Takeaways
- Cystic Fibrosis: High-calorie, high-protein, high-fat diet; pancreatic enzyme replacement (PERT).
- Celiac Disease: Lifelong strict gluten-free diet (no wheat, barley, rye).
- IBD (Crohn's): Exclusive Enteral Nutrition (EEN) for induction; monitor micronutrients.
- CKD: Protein restriction (stage-dependent), phosphorus control, ensure adequate calories.
- IEMs (e.g., PKU): Disease-specific dietary modifications and special formulas.
- T1DM: Carbohydrate counting, balanced meals, match insulin regimen.
- Chronic Liver Disease: Medium-chain triglycerides (MCTs), fat-soluble vitamin support_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

