Iron Deficiency Anemia - Rusty Pipes & Pale Faces
-
Etiology: Dietary (low bioavailability, Indian diets), ↑ demands (growth), blood loss, malabsorption.
-
Clinical Features: Pallor, fatigue, irritability. 📌 IRON: Reduced Hb, Oral (stomatitis, glossitis)/Odd cravings (pica), Nail (koilonychia).

-
Diagnosis:
- Hb < 11 g/dL (age-dependent).
- Indices: MCV ↓, MCH ↓, MCHC ↓, RDW ↑.
- Iron studies: S. Ferritin < 15 ng/mL (< 30 ng/mL with inflammation), S. Iron ↓, TIBC ↑, Transferrin Sat. < 16%.
⭐ Serum ferritin is the most sensitive and specific test for iron deficiency without inflammation.
-
Management:
- Oral: 3-6 mg/kg/day elemental iron; continue 2-3 months post-Hb normalization.
- Parenteral: Severe anemia + poor compliance/malabsorption/oral intolerance.
-
Prevention: Exclusive breastfeeding (6 months), iron-rich/fortified foods, prophylactic IFA supplementation (high-risk).
Iodine Deficiency Disorders - Thyroid's Tiny Terrors
- Spectrum:
- Fetal: Abortions, stillbirths, anomalies.
- Neonatal: Hypothyroidism, goiter.
- Child/Adolescent: Goiter, impaired mental & physical dev.
- Adult: Goiter, hypothyroidism, impaired mental function.
- Cretinism:
- Neurological: Severe MR, deaf-mutism, spasticity.
- Myxedematous: Dwarfism, myxedema, milder MR.
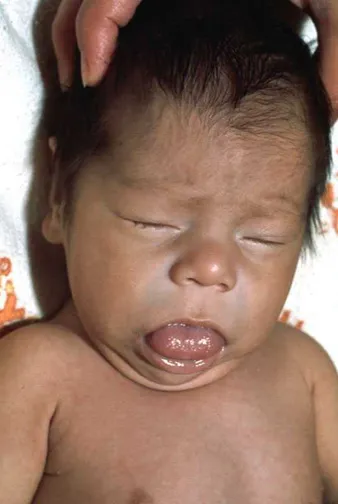
- 📌 Mnemonic '6 P's': Pot-belly, Pale, Puffy face, Protruding umbilicus, Protuberant tongue, Poor brain development.
- Diagnosis:
- Urinary Iodine Excretion (UIE): Population median < 100 µg/L (deficiency); Individual severe < 20 µg/L.
- Neonatal TSH screening (↑TSH).
- Serum: ↑TSH, ↓T3/T4.
- Thyroid palpation/USG for goiter.
- Management:
- Iodized salt (min. 15 ppm consumer).
- Iodine supplementation (age-specific).
- Prevention:
- Universal Salt Iodization (USI) - NIDDCP.
- Monitoring: Salt iodine, population UIE.
⭐ Iodine deficiency during pregnancy and early childhood is the world's leading preventable cause of brain damage.
Zinc Deficiency - Growth's Missing Link
Etiology: Inadequate intake (phytates, low animal food), malabsorption (celiac, IBD), ↑losses (diarrhea, burns), ↑req (prematurity, growth). Clinical Features:
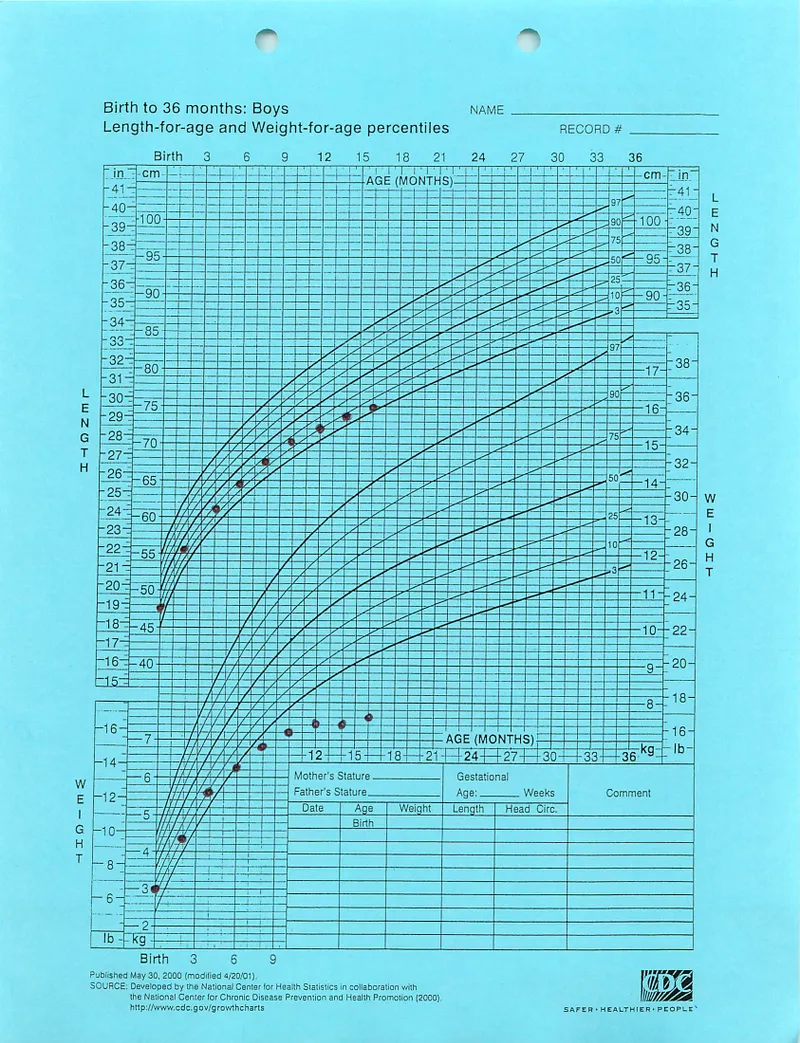
- Growth retardation/failure
- Diarrhea (acute/chronic)
- Dermatitis (acrodermatitis-like: periorificial, acral)

- Alopecia, Immune dysfunction (recurrent infections)
- Delayed wound healing, Hypogeusia/anorexia, Delayed sexual maturation. 📌 'ZINC DEF': Dermatitis/Diarrhea, Eye lesions/Emotional lability, Failure to thrive/Folliculitis, Infections (recurrent), Neuropsychiatric issues, Cutaneous lesions/Cell-mediated immunity ↓. Diagnosis:
- Serum zinc < 70 µg/dL (diurnal, inflammation)
- ↓ Alkaline phosphatase (zinc-dependent)
- Clinical response to supplementation. Management:
- Deficiency: Oral elemental Zn 1-2 mg/kg/day.
- Acute Diarrhea: 10 mg/day (<6mo), 20 mg/day (≥6mo) for 10-14 days.
⭐ WHO/UNICEF: Zinc for acute diarrhea reduces duration, severity, and future episodes. Prevention: Dietary diversification, fortification, supplementation.
Calcium & Other Key Minerals - Bone Builders & Body Balancers
-
Calcium:
- Role: Bone mineralization, nerve conduction, muscle contraction, clotting.
- Deficiency (Vit D linked): Rickets, osteomalacia, tetany (Chvostek's, Trousseau's), poor growth.
- 📌 'CATS Go Numb': Convulsions, Arrhythmias, Tetany, Spasms/Stridor, Numbness.
- Sources: Dairy, ragi, green leafy veg.
-
Copper:
- Role: Enzyme cofactor (ceruloplasmin, lysyl oxidase).
- Deficiency: Microcytic anemia (Fe-unresponsive), neutropenia, osteoporosis, depigmentation (Menkes: ATP7A gene).
⭐ Menkes disease: pili torti ('kinky hair'), growth failure, neurodegeneration (ATP7A mutation).
-
Fluoride:
- Role: Prevents dental caries, bone structure.
- Deficiency: ↑ Dental caries. Excess: Dental/Skeletal fluorosis.
- Optimal water: 0.7-1.2 ppm.
-
Selenium:
- Role: Antioxidant (glutathione peroxidase).
- Deficiency: Keshan disease (cardiomyopathy), Kashin-Beck (osteoarthropathy).
High‑Yield Points - ⚡ Biggest Takeaways
- Iron deficiency: Most common; pallor, pica, koilonychia, ↓ ferritin. Screen 9-12 months.
- Zinc deficiency: Acrodermatitis enteropathica (rash, alopecia, diarrhea), growth failure, impaired immunity.
- Iodine deficiency: Hypothyroidism, cretinism (intellectual disability, goiter). Salt iodization is key.
- Copper deficiency: Menkes disease (X-linked, kinky hair); osteoporosis, neutropenia, anemia, neurodegeneration.
- Selenium deficiency: Keshan disease (cardiomyopathy), Kashin-Beck disease (osteoarthropathy).
- Fluoride: Deficiency ↑ dental caries; excess → dental & skeletal fluorosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

