Eating Disorders Overview - Disorder Lineup
EDs: Persistent eating disturbances impairing health/function. Peak onset: adolescence.
- Anorexia Nervosa (AN): Intense fear of weight gain, distorted body image, severe restriction. BMI < 18.5 (adults) / <5th percentile (children).
- Bulimia Nervosa (BN): Recurrent binge eating + compensatory behaviors (e.g., vomiting, laxatives) ≥1x/week for 3 months.
- Binge Eating Disorder (BED): Recurrent binge eating episodes (distress, lack of control) ≥1x/week for 3 months, no regular compensatory behaviors.
- ARFID (Avoidant/Restrictive Food Intake Disorder): Food avoidance leading to nutritional deficiency/dependence; not due to body image concerns.
- Pica: Persistent eating of non-nutritive, non-food substances (≥1 month).
- Rumination Disorder: Repeated regurgitation of food (≥1 month).
- OSFED (Other Specified Feeding or Eating Disorder): Clinically significant EDs not meeting full criteria for AN, BN, BED, ARFID, Pica, or Rumination Disorder.
⭐ Anorexia Nervosa (AN) has the highest mortality rate of any psychiatric disorder.
Anorexia Nervosa - Starvation's Grip
-
Core: Energy restriction → significantly low body weight (contextual, e.g., <5th percentile for age); intense fear of weight gain; distorted body image.
-
Types: Restricting; Binge-eating/purging.
-
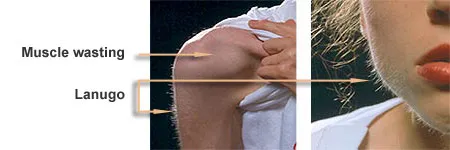
Features: Amenorrhea, lanugo, bradycardia, hypotension, hypothermia, osteoporosis. Psychological: Perfectionism, anxiety.
-
Severity (Adult BMI kg/m²): Mild ≥17, Mod 16-16.99, Sev 15-15.99, Ext <15.
-
⚠️ Refeeding Syndrome: Fluid/electrolyte shifts during re-feeding (↓$PO₄³⁻$, ↓$K⁺$, ↓$Mg²⁺$); can be fatal.
-
Management: Multidisciplinary. Medical stabilization; nutritional rehab (start 25-30 kcal/kg/day, ↑ gradually; monitor electrolytes esp. $PO₄³⁻$); psychotherapy (CBT, FBT). Olanzapine for weight gain.
⭐ Highest mortality of psychiatric disorders; due to medical complications (arrhythmias) or suicide.
Bulimia & BED - The Secret Cycle
-
Bulimia Nervosa (BN):
- Recurrent binge eating + compensatory behaviors (purging/non-purging).
- Frequency: ≥1x/week for 3 months.
- Self-evaluation unduly influenced by body shape/weight.
- Signs: Russell's sign (knuckles), dental erosion, parotid swelling.
- Complications: ↓K+, ↓Cl-, arrhythmias, Mallory-Weiss tears.
- Management: CBT, Fluoxetine (60mg/day).
-
Binge Eating Disorder (BED):
- Recurrent binge eating (no compensatory behaviors).
- Frequency: ≥1x/week for 3 months.
- Associated with ≥3 features (e.g., rapid eating, eating till full, eating alone, guilt).
- Marked distress regarding binging.
- Often linked to overweight/obesity & related comorbidities.
- Management: CBT, SSRIs, Lisdexamfetamine.

⭐ Hypokalemia is a common and dangerous complication of Bulimia Nervosa due to recurrent vomiting or laxative abuse, potentially leading to cardiac arrhythmias.
ARFID & Peds Focus - Beyond Weight Fears
- ARFID (Avoidant/Restrictive Food Intake Disorder):
- Persistent eating disturbance → failure to meet appropriate nutritional and/or energy needs.
- Key: No distress about body weight or shape (differentiates from Anorexia/Bulimia).
- Manifests as one or more:
- Significant weight loss / faltering growth (children).
- Significant nutritional deficiency.
- Dependence on enteral feeding or oral nutritional supplements.
- Marked interference with psychosocial functioning.
- Common underlying reasons: Sensory sensitivity to food qualities, fear of aversive consequences (e.g., choking, vomiting), apparent lack of interest in eating or food.
- Other Non-Weight Focused EDs (Briefly):
- Pica: Persistent eating of non-nutritive, non-food substances for ≥ 1 month; developmentally inappropriate.
- Rumination Disorder: Repeated regurgitation of food for ≥ 1 month; not due to a medical condition.
- Pediatric Management Focus:
- Multidisciplinary team: Pediatrician, dietitian, psychologist/psychiatrist.
- Nutritional rehabilitation: Restore weight, correct deficiencies.
- Behavioral therapies: e.g., exposure therapy, CBT for ARFID.
- Strong family involvement and support.
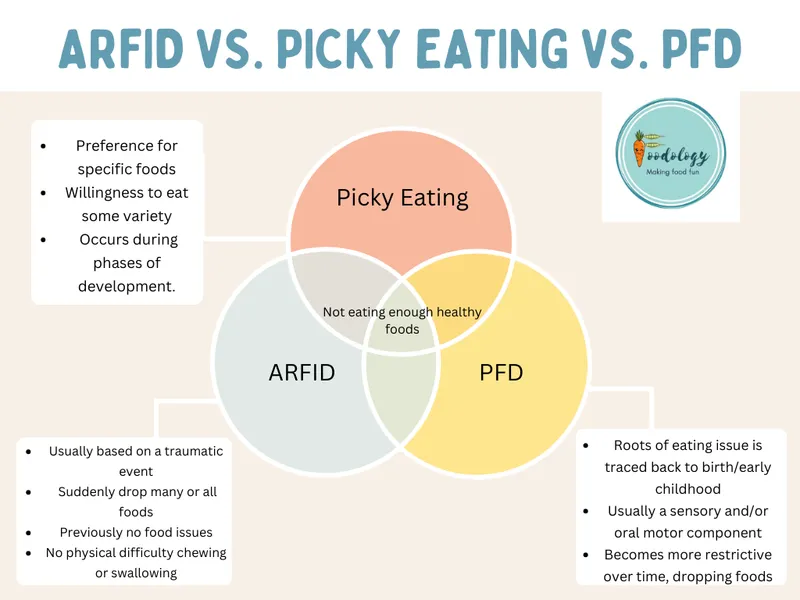
⭐ ARFID often has an onset in infancy or early childhood and may persist into adulthood; it can be associated with anxiety disorders, ASD, OCD, and ADHD.
High‑Yield Points - ⚡ Biggest Takeaways
- Anorexia Nervosa: Fear of weight gain, distorted body image, low BMI. Key: amenorrhea, bradycardia, osteoporosis.
- Bulimia Nervosa: Binge eating with compensatory actions. Often normal weight. Signs: dental erosion, parotid swelling.
- Binge Eating Disorder: Binge eating WITHOUT compensatory actions; causes distress, often obesity.
- ARFID: Food avoidance (not body image related); causes nutritional deficiency.
- Refeeding Syndrome: Risk in severe malnutrition; monitor phosphate.
- Treatment: Multidisciplinary (medical, nutrition, psychotherapy e.g., FBT).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

