Indoor Pollutants - Tiny Troublemakers
- Biological Agents:
- Molds: Damp areas; trigger asthma, allergies.
- Dust Mites: Bedding, carpets; asthma, eczema.
- Pet Dander: Animals; allergic reactions.
- Chemical Agents:
- Volatile Organic Compounds (VOCs): Paints, solvents; irritate eyes, respiratory tract.
- Formaldehyde ($CH_2O$): Furniture, glues; carcinogen, respiratory irritant.
- Carbon Monoxide ($CO$): Fuel burning; hypoxia. 📌 Silent Killer.
- Nitrogen Dioxide ($NO_2$): Gas stoves; ↑ respiratory infections.
- Lead (Pb): Old paint dust; neurotoxic, affects development.
- Environmental Tobacco Smoke (ETS): Major risk for SIDS, asthma, LRTI.
- Radon: Soil gas; lung cancer risk.

⭐ Environmental Tobacco Smoke (ETS) exposure is a significant risk factor for Sudden Infant Death Syndrome (SIDS) and recurrent lower respiratory tract infections (LRTIs) in children.
Pollutant Hotspots - Home Hazards
- Kitchen (Major Source):
- Biomass fuel (chulha - wood, dung, crop waste): ↑ Particulate Matter (PM2.5, PM10), CO, Polycyclic Aromatic Hydrocarbons (PAHs).
- Kerosene/LPG stoves (incomplete combustion, poor ventilation): ↑ $NO_2$, CO.

- Living Areas & Bedrooms:
- Mosquito coils/liquidators: Pyrethroids, VOCs, smoke.
- Incense sticks (agarbatti): PM, VOCs (benzene, formaldehyde), CO.
- Dust mites (mattresses, carpets, upholstery): Allergens (Der p1).
- Mould/Fungus (dampness, esp. monsoon): Spores, Mycotoxins, MVOCs.
- Paints, polishes, new furniture/plywood: Formaldehyde, VOCs.
- Environmental Tobacco Smoke (ETS).
- Other Sources:
- Cleaning products (phenols, ammonia): VOCs.
- Pesticides (sprays, chalks).
⭐ Biomass fuel use in poorly ventilated kitchens is a leading cause of indoor air pollution in rural India, significantly increasing risk of acute lower respiratory infections (ALRI) in children < 5 years.
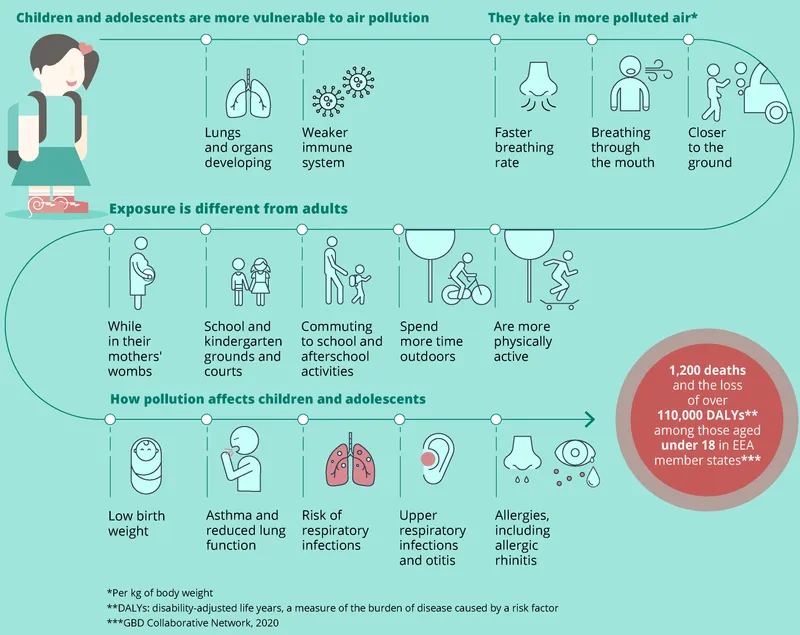
Child Health Hits - Vulnerable Lungs & Brains
- Unique Vulnerabilities:
- Higher respiratory rate & pollutant intake per kg body weight.
- Narrower airways, ↑ obstruction risk.
- Immature immune & detoxification systems.
- Developing organs (lungs, brain) - critical vulnerability periods.
- Greater exposure: hand-to-mouth behavior, proximity to floor.
- Longer life expectancy for chronic effects.
- Respiratory Impacts:
- ↑ LRTI (pneumonia, bronchiolitis).
- Asthma: new onset, exacerbations, severity.
- Impaired lung development, ↓ lung function (e.g., FEV1).
- Chronic cough, wheezing, allergic rhinitis.
- Neurodevelopmental & Other Impacts:
- Cognitive impairment (↓ IQ), learning disabilities.
- ADHD, behavioral problems.
- Possible links to Autism Spectrum Disorder.
- SIDS (Sudden Infant Death Syndrome) risk (e.g., from SHS).
- Otitis Media.
⭐ Exposure to indoor air pollutants like secondhand smoke (SHS) during early childhood is a major risk factor for Sudden Infant Death Syndrome (SIDS), recurrent otitis media, and severe asthma.
Safe Sanctuaries - Clean Air Strategies
- Core Strategy: The 3 Pillars (📌 Mnemonic: SAVE - Source control, Air cleaning, Ventilation, Evaluation/Education)
- 1. Source Control: Most effective.
- Ban indoor smoking.
- Use low-VOC (Volatile Organic Compound) products.
- Control dampness (target humidity <50%) to prevent mold.
- Integrated Pest Management (IPM).
- Test for Radon; mitigate if levels >4 pCi/L.
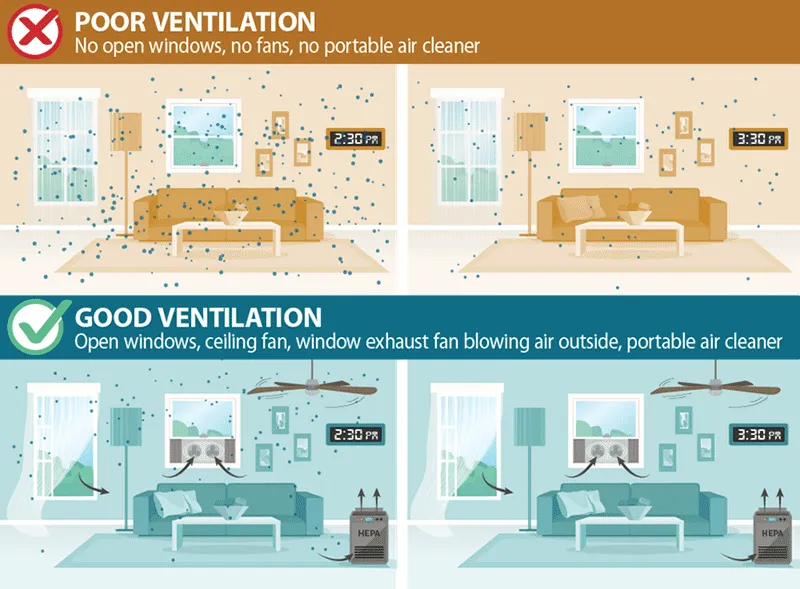
- 2. Ventilation: Dilutes & removes pollutants.
- Natural: Cross-ventilation via windows.
- Mechanical: Exhaust fans (kitchen/bath), HVAC systems (MERV ≥13 filters).
- 3. Air Cleaning: Supplements other methods.
- Portable air cleaners with HEPA filters.
⭐ HEPA filters are crucial, removing ≥99.97% of particles ≥0.3 µm (dust, pollen, mold spores, bacteria).
- Activated carbon for VOCs/odors.
- 1. Source Control: Most effective.
- Maintenance & Monitoring: Regular cleaning, filter changes. Install CO alarms.
High‑Yield Points - ⚡ Biggest Takeaways
- Secondhand smoke (SHS): Major indoor pollutant; linked to SIDS, respiratory infections, asthma.
- Biomass fuel (India): Key risk for ALRI due to indoor combustion (wood, dung) in poor ventilation.
- Carbon Monoxide (CO): Odorless gas from incomplete combustion; causes hypoxia, neurotoxicity. Suspect in unexplained drowsiness.
- Molds & dampness: Trigger allergies, asthma exacerbations, and respiratory issues.
- Volatile Organic Compounds (VOCs) (paints, furnishings): Irritate airways, worsen asthma.
- Lead dust (old paint): Inhalation/ingestion risk for childhood lead poisoning.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

