Vulnerability & Overview - Tiny Humans, Big Risks
- Children face amplified risks from climate change due to unique physiological and developmental factors.
- Key Physiological Vulnerabilities:
- ↑ Respiratory rate: greater inhalation of air pollutants.
- ↑ Surface area to body mass ratio: enhanced dermal absorption of toxins.
- Immature organ systems (e.g., lungs, immune, nervous systems).
- Higher metabolic rate: increased toxin intake per body weight.
- Longer life expectancy: more time for latent effects to manifest.
- Dependency & Behavioral Factors:
- Reliance on caregivers for safety and resources.
- Limited ability to recognize or escape environmental hazards.
- Increased outdoor play and hand-to-mouth behaviors.

⭐ Children bear a disproportionately high burden of climate-sensitive diseases, including diarrheal diseases, malnutrition, and vector-borne illnesses like malaria.
Direct Climate Impacts - Nature's Fury Hits Hard
⭐ Extreme weather events (floods, cyclones) are major causes of child mortality and morbidity in India via direct injuries, drowning, and displacement.
- Heat Extremes (Heatwaves):
- Children vulnerable: ↑SA:Vol ratio, immature thermoregulation, dependence.
- Heatstroke: Emergency; core temp > 40°C, altered sensorium, hot/dry skin.

- Intense Storms & Flooding:
- Trauma (fractures, wounds), electrocution.
- Drowning: Key cause of flood-related child deaths.
- Wildfires: Burns, smoke inhalation, respiratory distress.
Indirect Climate Impacts - The Ripple Effect Perils

- Vector-Borne Diseases (VBDs): ↑Temperature & altered rainfall → ↑vector (mosquito, tick) breeding & survival.
- India: ↑Dengue, Malaria, Chikungunya, Japanese Encephalitis (JE), Kyasanur Forest Disease (KFD).
- Expanded geographic range & longer transmission seasons.
- Water Insecurity & Contamination: Altered precipitation, ↑floods & droughts → ↓water quality & availability.
- ↑Risk: Cholera, typhoid, diarrheal diseases, hepatitis A & E.
- Food Insecurity & Malnutrition: Extreme weather (floods, droughts, heatwaves) → ↓crop yields & livestock productivity.
- Impacts: ↑Childhood malnutrition (stunting, wasting), micronutrient deficiencies.
- Disrupted food supply chains.
⭐ Climate change is projected to increase the incidence and geographic spread of vector-borne diseases like dengue, chikungunya, and Japanese Encephalitis in India.
Indian Scenario & Action - Our Kids, Our Climate Fight
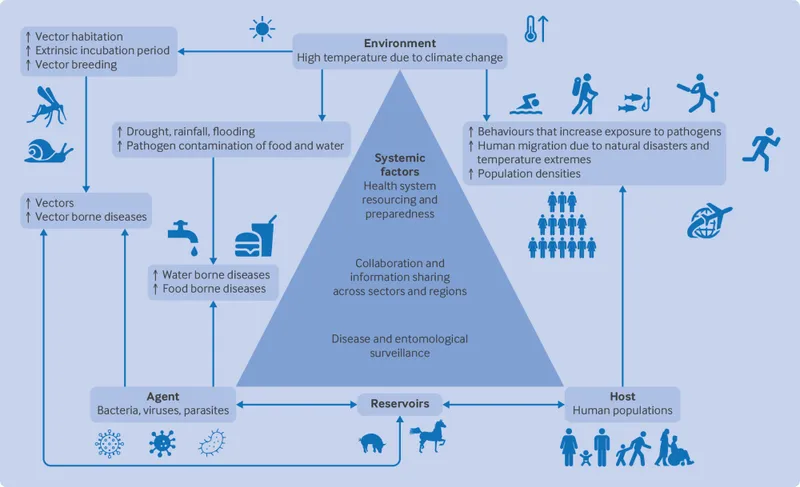
- Vulnerability Hotspots: Children in coastal regions, arid zones, urban slums, and tribal belts face heightened risks.
- Key Indian Concerns:
- ↑ Heatwaves: Risk of heatstroke, dehydration, esp. neonates & infants.
- Water Scarcity & Contamination: Leads to ↑ diarrheal diseases (cholera, typhoid), malnutrition.
- Vector-Borne Diseases: Changing patterns for malaria, dengue, chikungunya due to altered temperature & rainfall.
- Air Pollution: Exacerbated by climate change, ↑ respiratory illnesses (asthma, bronchitis).
- Food Insecurity: Crop failures impact child nutrition.
- National Response:
- National Action Plan on Climate Change (NAPCC) & State Action Plans (SAPCCs).
⭐ The National Action Plan on Climate Change and Human Health (NAPCCHH) in India emphasizes strengthening surveillance, health workforce capacity, and inter-sectoral coordination.
- Pediatrician's Role: Advocacy for child-centric policies, community education on adaptation, early detection of climate-sensitive diseases, promoting sustainable healthcare practices within clinics/hospitals. Support for Mission LiFE (Lifestyle for Environment).
High‑Yield Points - ⚡ Biggest Takeaways
- Children are disproportionately vulnerable to climate change impacts due to unique physiological and developmental factors.
- Increased risk of vector-borne diseases (dengue, malaria) and water-borne illnesses (cholera, typhoid).
- Greater susceptibility to heat stress, dehydration, and heat-related illnesses.
- Worsening air quality from pollution and wildfires exacerbates respiratory conditions like asthma.
- Food and water insecurity leads to malnutrition, stunting, and increased diarrheal disease burden.
- Climate change can also impact child mental health and neurodevelopment adversely.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

