Headache Basics & Types - Kiddo Head Pains
- Headache (cephalgia): Pain in head/upper neck. Common in children.
- Types:
- Primary: No underlying cause. E.g., Migraine, Tension-Type Headache (TTH).
- Secondary: Due to pathology. E.g., Infection, tumor, ↑ICP.
- ⚠️ Red Flags (SNOOPP):
- Systemic: Fever, weight loss, immunosuppression.
- Neurologic: Focal deficits, papilledema, altered mental status, seizures.
- Onset: Sudden (thunderclap), new in child <5 yrs, or recent significant change.
- Occipital: Especially if isolated and in young children.
- Pattern: Progressive, wakes from sleep, worse with Valsalva/cough, postural aggravation.
- 📌 SNOOPP helps screen for serious underlying causes.
⭐ Migraine is the most common cause of recurrent headaches in children.
Pediatric Migraine - Little Brain Storms
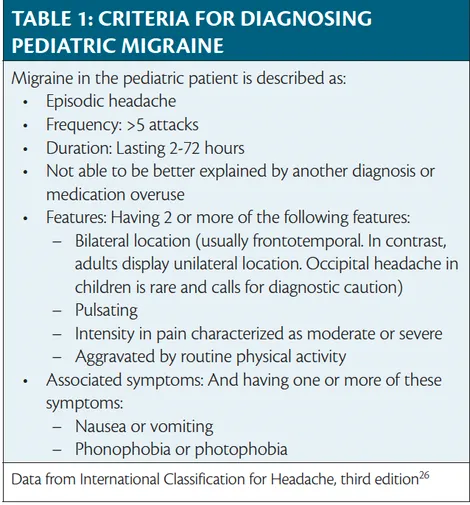
- Common primary headache; ~7-10% child prevalence.
- Clinical (vs. Adults):
- Shorter: 1-72 hrs.
- Often bilateral (frontal/temporal).
- Prominent GI: Nausea, vomiting, abdominal pain.
- Aura: Visual (common), sensory.
- Diagnosis: ICHD-3 (≥5 attacks).
- Variants: Abdominal Migraine, Cyclical Vomiting (CVS), Benign Paroxysmal Vertigo (BPV).
- Management:
- Acute: Ibuprofen (10 mg/kg); Sumatriptan (age-specific).
- Prophylaxis: Topiramate, Propranolol (frequent/disabling).
- Non-pharm: Trigger avoidance, lifestyle.
⭐ Pediatric migraine attacks are often shorter (1-72h), bilateral, with prominent GI symptoms; aura may be atypical (e.g., confusion).
Other Headaches & Red Flags - Danger Signals
-
Tension-Type Headache (TTH):
- Most common primary headache.
- Bilateral, non-pulsating, "band-like" pressure.
- Mild-moderate intensity. Not worsened by routine activity.
- No nausea/vomiting; photophobia OR phonophobia (not both).
- Rx: NSAIDs, Paracetamol. Prophylaxis: Amitriptyline.
-
Headache Red Flags (Danger Signals) 📌 SNOOP + 3 P's:
- Systemic symptoms (fever, weight loss) or risk factors (cancer, HIV).
- Neurologic signs/symptoms (focal deficits, altered mental status, seizures).
- Onset: Sudden ("thunderclap"), or new/progressive in child < 5 yrs.
- Occipital location (posterior fossa tumor risk).
- Papilledema (check fundus!).
- Pattern change (↑frequency/severity, awakens from sleep).
- Precipitated by Valsalva/cough/exertion, or Postural trigger.
⭐ > Occipital headache in a child is a red flag for a posterior fossa tumor until proven otherwise.

Headache Management - Kid-Friendly Relief
- Non-Pharmacological First! (Pillar of management)
- Lifestyle: Regular sleep, hydration, balanced diet, identify & avoid triggers.
- Stress reduction: Relaxation techniques, CBT, biofeedback.
- Acute (Abortive) Therapy: (Step-up approach)
- Mild: Rest, paracetamol (15 mg/kg), ibuprofen (10 mg/kg).
- Migraine (Mod-Severe): If simple analgesics fail or severe onset.
- Triptans: Sumatriptan Nasal Spray (>12y), Rizatriptan ODT (>6y), Almotriptan tabs (>12y).
- Antiemetics: Ondansetron, Domperidone (⚠️ QT risk).
- Prophylactic (Preventive) Therapy:
- Indications: ≥4 headache days/month, prolonged attacks, significant disability, or abortive therapy failure/overuse.
- Meds: Propranolol, Topiramate (⚠️ cognitive effects), Amitriptyline, Flunarizine. Cyproheptadine (esp. <7y, appetite stimulant).
⭐ In children >12 years with acute moderate-to-severe migraine, sumatriptan nasal spray (10-20 mg) is a preferred first-line specific therapy if NSAIDs are insufficient.

High‑Yield Points - ⚡ Biggest Takeaways
- Migraine in children: often bilateral, shorter duration; positive family history common. Aura may occur.
- Tension-type headache (TTH): typically bilateral, "band-like" pressure, not worsened by routine activity.
- Key Red Flags: sudden severe onset, neurological deficits, papilledema, persistent morning vomiting, age <5.
- Acute treatment: ibuprofen or paracetamol. Sumatriptan (nasal/oral) for adolescent migraines.
- Consider prophylaxis (e.g., propranolol, topiramate) for frequent or disabling migraines.
- Medication Overuse Headache (MOH): identify early; caused by frequent analgesic/triptan use.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

