Basics of Immunotherapy - Immune Tune-Up
- Definition: Therapeutic administration of allergens to induce immune tolerance in allergic individuals, modifying the natural course of allergic disease.
- Goal: Achieve long-term symptom remission, prevent new sensitizations, and improve quality of life.
- Mechanism of Action:
- Shifts immune response from Th2 (pro-allergic) to Th1 (protective).
- Induces regulatory T cells (Tregs) & regulatory B cells (Bregs).
- ↑ Production of blocking antibodies (IgG4).
- ↓ Allergen-specific IgE levels over time.
- ↓ Mast cell, basophil, and eosinophil reactivity.
- Core Principle: Gradual, controlled exposure to increasing doses of specific allergens.
⭐ Immunotherapy is the only disease-modifying treatment for allergic diseases.
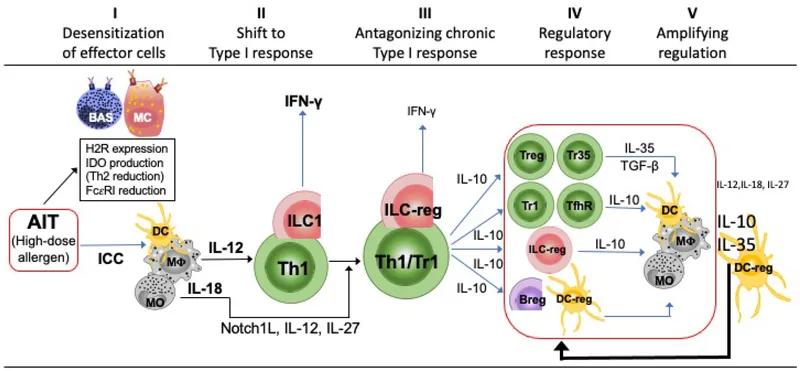
Allergen Immunotherapy (AIT) - Allergy Avengers Assemble
-
Goal: Induce allergen-specific tolerance, modify disease course.
-
Mechanism: ↑Treg, IL-10, IgG4 (blocking Ab); ↓IgE, mast cell reactivity; Th2→Th1 shift.
-
Indications:
- Allergic rhinitis/conjunctivitis (mod-severe, persistent).
- Allergic asthma (mild-mod, controlled, allergen confirmed).
- Venom hypersensitivity (VIT highly effective).
- Atopic dermatitis (select cases with aeroallergens).
- Criteria: IgE-mediated allergy, allergen unavoidable, meds/avoidance insufficient.
-
Contraindications:
- Absolute: Uncontrolled asthma (FEV1 < 70%), active systemic autoimmune disease, malignancy.
- Relative: Significant CVD, β-blockers/ACE-i (esp. SCIT), poor adherence, pregnancy (initiation).
-
SCIT vs. SLIT:
⭐ Sublingual Immunotherapy (SLIT) generally has a better safety profile than Subcutaneous Immunotherapy (SCIT), especially regarding systemic reactions.
- Duration: Typically 3-5 years for sustained benefit post-discontinuation.
- 📌 AIT: Alleviates Immune Troubles!
AIT Practicalities - Dose, Duration, Dangers
- Dosing & Standardization:
- Allergen extracts standardized: Bioequivalent Allergy Units (BAU), Allergy Units (AU).
- Phases: Build-up (weekly/bi-weekly, gradually ↑dose) & Maintenance (monthly, constant highest tolerated dose).
- Dose adjustments for missed doses, local/systemic reactions, or new allergen vials.
- Duration for Tolerance:
⭐ The standard duration for allergen immunotherapy (SCIT/SLIT) to achieve long-term tolerance is typically 3-5 years.
- Decision to stop based on sustained clinical benefit and patient/physician assessment.
- Dangers & Management:
- Local Reactions: Common (erythema, pruritus, swelling at injection site). Manage with cold compresses, topical corticosteroids, oral antihistamines.
- Systemic Reactions (SRs): Range from mild (urticaria, rhinitis) to severe anaphylaxis.
- Risk factors: Uncontrolled asthma, high allergen dose, dosing errors, concurrent illness.
- 📌 Anaphylaxis: Epinephrine (0.01 mg/kg of 1:1000 solution IM, max 0.3-0.5 mg per dose), O2, IV fluids, antihistamines, corticosteroids. Observe for 4-6 hours.
- Contraindications (Absolute): Severe uncontrolled asthma, active autoimmune disease. (Relative): Beta-blocker/ACE inhibitor use, significant cardiovascular disease.

Special ITx - Venom Victors & Food Frontiers
- Venom Immunotherapy (VIT):
- Highly effective for Hymenoptera venom allergy (bees, wasps, ants).
- Significantly ↓ anaphylaxis risk from future stings.
- Protocol: Initial build-up, then maintenance every 4-8 weeks for 3-5 years.
- Indications: Systemic reaction to sting + positive venom IgE or skin test.
⭐ Venom immunotherapy (VIT) is nearly 95-98% effective in preventing anaphylaxis from future stings in sensitized individuals.
- Food Immunotherapy (FIT):
- Oral (OIT): Aims to desensitize to specific foods (e.g., peanut, milk, egg). Involves ingesting gradually increasing allergen doses. Requires strict medical supervision.
- Sublingual (SLIT): Alternative to OIT for food allergy; potentially fewer systemic reactions but less established for food allergens compared to aeroallergens or VIT for venom.
High‑Yield Points - ⚡ Biggest Takeaways
- Allergen Immunotherapy (AIT) aims to induce allergen-specific immune tolerance.
- Key indications: severe allergic rhinitis, allergic asthma, and insect venom hypersensitivity.
- Mechanism: Shifts from Th2 to Th1 response, increases Treg cells and IgG4 blocking antibodies.
- Routes: Subcutaneous (SCIT) and Sublingual (SLIT) are primary methods.
- Duration: Typically 3-5 years for sustained, disease-modifying effects.
- SCIT carries a risk of anaphylaxis; requires post-injection observation.
- AIT can lead to long-term remission of allergic symptoms after completion of therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

