Anaphylaxis: Definition & Pathophysiology - Shocking Speed Reaction
- Definition: Severe, life-threatening, generalized or systemic hypersensitivity reaction with rapid onset.
- Pathophysiology:
- Primarily Type I Hypersensitivity (IgE-mediated).
- Mechanism: Allergen cross-links IgE on mast cells & basophils → degranulation.
- Mediators Released:
- Preformed: Histamine (vasodilation, ↑vascular permeability), Tryptase.
- Newly Synthesized: Leukotrienes (bronchoconstriction), Prostaglandins, Platelet-Activating Factor (PAF).
- Non-IgE mediated (Anaphylactoid): Direct mast cell/basophil degranulation (e.g., radiocontrast media, opioids, NSAIDs).
⭐ Serum tryptase levels peak 1-2 hours after onset of symptoms and can be a useful diagnostic marker.
Anaphylaxis: Triggers & Risk Factors - Culprit Countdown
- Top Triggers (📌 FILM):
- Foods: Peanuts, tree nuts, milk, eggs, shellfish. (Common in children)
- Medications: NSAIDs, penicillins, contrast media. (Common in adults)
- Insect Stings: Bees, wasps, ants.
- Latex.
- Key Risk Factors:
- Atopy (asthma, eczema).
- History of previous anaphylaxis.
- Mastocytosis.
- ⚠️ Beta-blockers/ACE-inhibitors may worsen severity.

⭐ Food is the most common trigger of anaphylaxis in children, while medications are more common in adults.
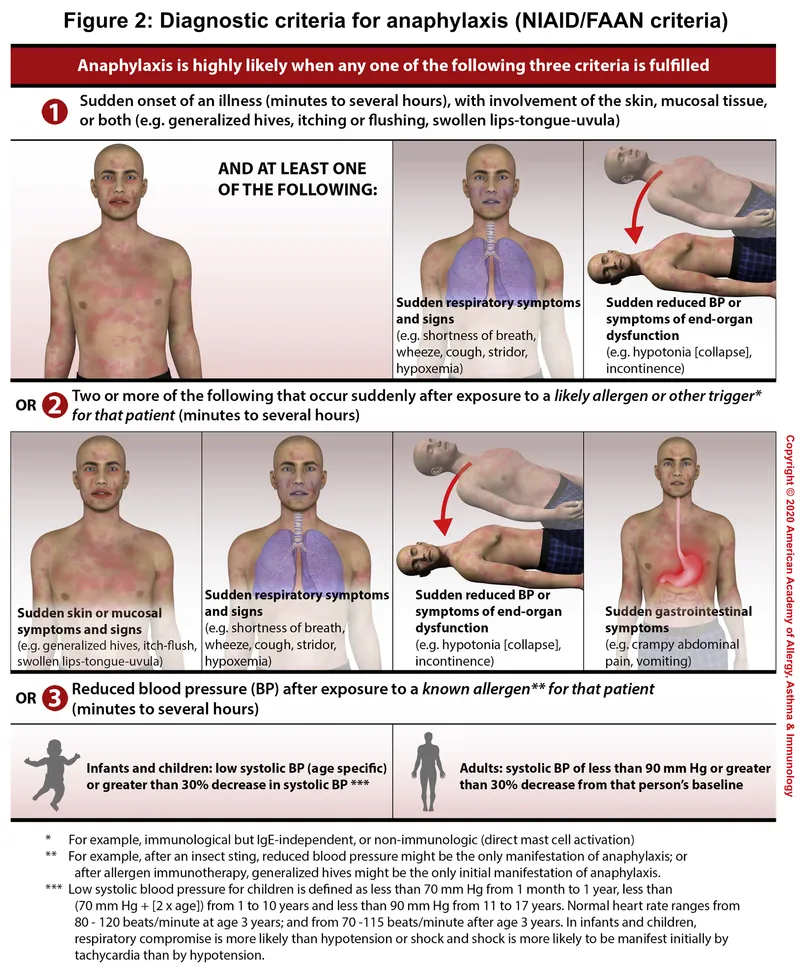
Anaphylaxis: Clinical Features & Diagnosis - Symptom Storm Signs
Rapid onset (mins-hrs) multi-system reaction.
- Skin/Mucosal (~90%): Urticaria, angioedema (lips, tongue, larynx), pruritus, flushing.
- Respiratory (~70%):
- Lower: Dyspnea, wheeze.
- Upper: Stridor, hoarseness (⚠️ laryngeal edema).
- Cardiovascular (~45%): Hypotension (SBP <90 mmHg or >30% drop), tachycardia, shock.
- GI (~45%): Nausea, vomiting, abdominal pain.
- Other: Sense of impending doom.
Diagnosis: Clinical. NIAID/FAAN criteria key. Lab (supportive): ↑ Serum tryptase (peaks 1-2 hrs).
⭐ Biphasic anaphylaxis (symptom recurrence 1-72 hrs later without re-exposure) occurs in up to 20% of cases.
Anaphylaxis: Acute Management - Epi Pen Power Play
- Immediate: Assess ABCs. Call help. Position supine, legs elevated (respiratory distress: semi-recumbent).
- IM Epinephrine (1:1000): First-line! STAT to anterolateral thigh.
- Dose: 0.01 mg/kg.
- Adult: 0.3-0.5 mg.
- Child: 0.01 mg/kg (max 0.3 mg).
- Repeat 5-15 min if symptoms persist/recur.
- Dose: 0.01 mg/kg.
- EpiPen®:
- Adult (>30kg): 0.3mg.
- Child (15-30kg): 0.15mg. 📌 Jr. for 0.15mg.
- Adjuncts (after Epinephrine):
- Oxygen: High flow 6-8 L/min.
- IV Fluids: NS/RL 10-20 ml/kg rapid bolus.
- Antihistamines: H1 (Diphenhydramine) + H2 blockers (Ranitidine).
- Corticosteroids: Hydrocortisone to prevent biphasic reaction (onset 4-6 hrs).
- Bronchodilators: Salbutamol for persistent wheezing.
⭐ β-blocker refractory anaphylaxis: Glucagon 1-5 mg IV over 5 min, then infusion.
Anaphylaxis: Long-term & Prevention - Allergy Armor Up

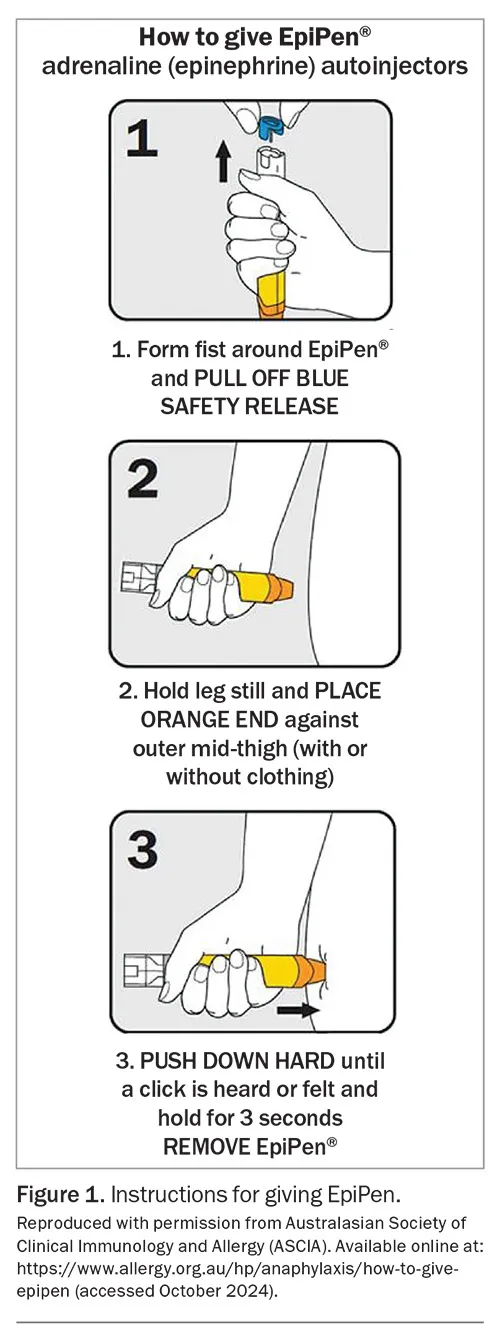
- Epinephrine Auto-Injector (EAI): Prescribe TWO devices. Train patient & family on correct use (e.g., technique, expiry).
- Allergen Avoidance: Strict, educated avoidance of identified triggers. Emphasize food label reading.
- Written Anaphylaxis Action Plan: Clear emergency steps for patient/caregivers.
- Specialist Referral: To Allergist/Immunologist for evaluation & potential immunotherapy.
- Medical Alert Jewelry: Strongly recommended.
⭐ Biphasic anaphylaxis occurs in up to 20% of cases, typically 1-72 hours (commonly 8-12 hrs) after initial resolution; mandates adequate observation post-treatment.
High‑Yield Points - ⚡ Biggest Takeaways
- Anaphylaxis: Severe, rapid-onset systemic hypersensitivity reaction, potentially life-threatening.
- Key triggers: Foods (milk, peanut), drugs (penicillin), insect stings.
- Pathophysiology: IgE-mediated mast cell degranulation releasing histamine.
- Clinical: Multi-system (skin, respiratory, CV, GI); biphasic reaction possible (1-72 hrs).
- Treatment cornerstone: IM Adrenaline (0.01 mg/kg, 1:1000) in anterolateral thigh.
- Adjuncts: Corticosteroids (prevent biphasic), antihistamines, oxygen, IV fluids.
- Diagnosis: Primarily clinical; serum tryptase may be elevated post-reaction (peaks 1-2 hrs).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


