FTT Fundamentals - Defining the Dip
- Failure to Thrive (FTT): Inadequate growth in infants & children; a sign, not a diagnosis.
- Key Anthropometric Criteria:
- Weight for age < 3rd or 5th percentile.
- Weight for length/height < 3rd or 5th percentile.
- Weight gain velocity < expected for age.
- Deceleration: Weight crossing ≥2 major centile lines downwards.
- Classification:
- Organic: Due to underlying medical illness (e.g., malabsorption, CHD).
- Non-organic (Psychosocial): Environmental/caregiver factors (e.g., neglect, poor feeding technique).
- Mixed: Combination of both.
⭐ Weight falling >2 major centile lines on a standard growth chart is a key indicator of FTT.
Root Causes - Why So Small?
Failure to Thrive (FTT) signifies chronically insufficient usable calories. Key mechanisms:
| Category | Key Causes & Examples |
|---|---|
| Organic FTT | Medical conditions: Impaired intake (CNS, cleft, GERD), malabsorption (celiac, CF), ↑demand (CHD, chronic infection/TB), metabolic disorders. |
| Non-Organic FTT | Psychosocial factors: Faulty feeding, insufficient food (poverty), neglect, maternal depression, poor parent-child interaction. |
- Feeding problems (technique, supply)
- Absorption (celiac, CF)
- Increased losses (GERD, diarrhea)
- Low intake (neglect, poverty)
- Utilization (metabolic, renal)
- Requirements ↑ (CHD, infection)
- Environmental/Endocrine
⭐ In India, infections (like TB, recurrent diarrhea) and inadequate calorie intake due to poverty or improper feeding practices are major contributors to organic and non-organic FTT respectively.
Detective Work - Spotting FTT
- Core Principle: Identify ↓ growth velocity or crossing 2 major percentile lines on growth charts.
- History Taking - The Foundation:
- Dietary: Detailed 3-day diet recall (type, quantity, frequency, feeding difficulties, mealtime environment).
- Medical: Prenatal, birth, postnatal illnesses, developmental milestones, medications.
- Social & Family: Psychosocial stressors, caregiver-child interaction, family support, economic factors.
- Clinical Examination - The Clues:
- Anthropometry: Accurate weight, height/length, head circumference (HC). Plot on WHO/IAP charts.
- Weight-for-age < 3rd or < 5th percentile.
- Weight-for-length/height < 3rd or < 5th percentile.
- ↓ growth velocity: Crossing ≥2 major percentile lines.
- Systemic exam: Signs of malnutrition (e.g., muscle wasting, ↓ subcutaneous fat, hair/skin changes), dysmorphism, or underlying organic disease.
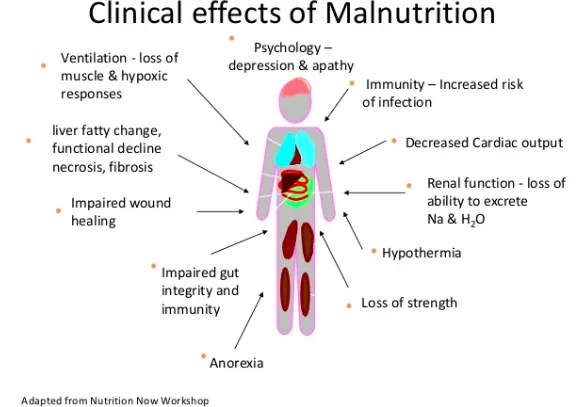
- Anthropometry: Accurate weight, height/length, head circumference (HC). Plot on WHO/IAP charts.
- Initial Investigations (Guided by History & Physical - H&P):
- CBC, ESR
- Urine analysis & culture
- Stool for ova, parasites, occult blood, reducing substances
- Serum electrolytes, renal function tests (RFT), liver function tests (LFT) (if indicated)
⭐ A 3-day diet recall is a crucial first step in evaluating caloric intake for a child with suspected FTT.
Fixing FTT - Growth Boosters
- Goal: Achieve catch-up growth; target weight gain 20-30 g/day (infants), 10-15 g/day (older children).
- Nutritional Rehabilitation:
- Calorie intake: $120-150 \text{ kcal/kg/day}$ (can go up to $200 \text{ kcal/kg/day}$ in severe cases).
- Protein: $2-3 \text{ g/kg/day}$.
- High-calorie diet: Fortified foods, energy-dense formulas.
- Micronutrients: Iron, Zinc, Vitamin A, Vitamin D supplementation as needed.
- Feeding Strategies:
- Structured, frequent meals & snacks.
- Positive feeding environment; avoid force-feeding.
- Parental education & counseling.
- Address Underlying Cause: Treat infections, malabsorption, psychosocial issues.
- Monitoring: Regular weight, height, head circumference checks.
⭐ Initial nutritional rehabilitation for severe FTT often requires 120-150 kcal/kg/day and 2-3 g protein/kg/day for catch-up growth.
- Hospitalization if: Severe malnutrition, dehydration, suspected abuse/neglect, failed outpatient management, or complex medical needs requiring multidisciplinary care (e.g., feeding tube).
High-Yield Points - ⚡ Biggest Takeaways
- Definition: Weight < 3rd-5th percentile or crossing 2 major centiles downwards on growth charts.
- Most common cause: Inadequate caloric intake, often psychosocial (non-organic FTT).
- Organic FTT: Caused by underlying medical conditions like malabsorption or chronic illness.
- Sequence of growth failure: Weight affected first, then length/height, lastly head circumference.
- Key investigation: Detailed dietary history and observation of feeding.
- Management: Focus on nutritional rehabilitation and treating any underlying organic cause.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

