Cerebral Palsy - Brain's Motion Muddle
CP: A group of permanent, non-progressive motor disorders affecting movement & posture, from disturbances in the developing fetal/infant brain.
-
Risk Factors: 📌 PREMATURE
- Prematurity, Perinatal asphyxia
- Rubella, Radiation
- Eclampsia, Erythroblastosis fetalis
- Multiple births
- Antepartum hemorrhage
- Toxins
- Unexplained
-
Classification:
Type Subtypes Key Features Spastic Diplegia, Hemiplegia, Quadriplegia ↑Muscle tone, hyperreflexia, UMN signs Dyskinetic Athetoid, Dystonic Involuntary movements, fluctuating tone Ataxic ↓Coordination, balance issues, wide-based gait Mixed Combination of types Varied presentation
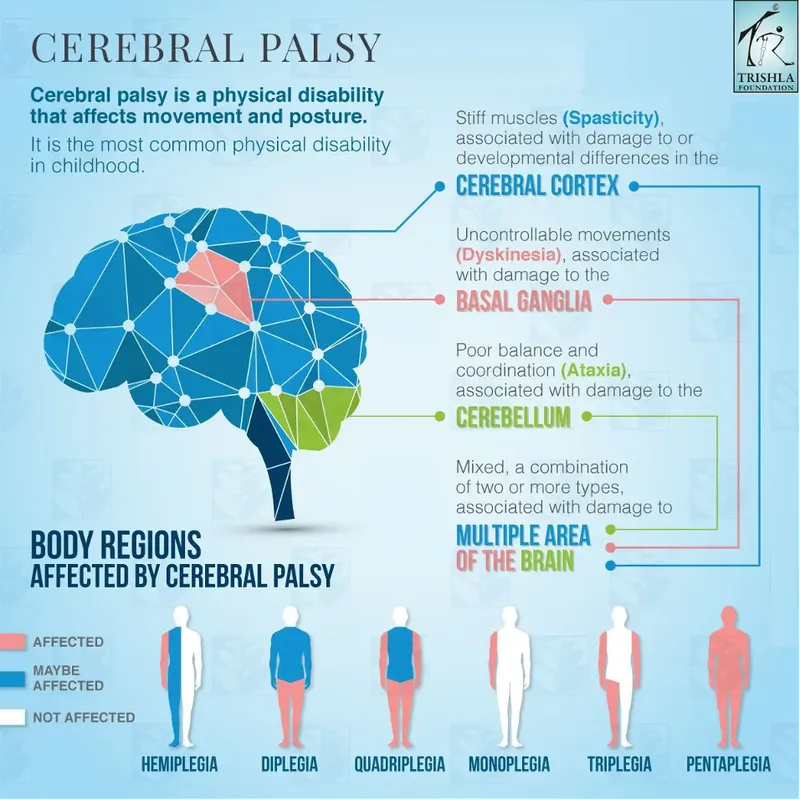
- Clinical Features: Delayed motor milestones, abnormal tone (spasticity/hypotonia), persistent primitive reflexes, feeding difficulties.
- Management: Multidisciplinary: physiotherapy, OT, speech therapy, antispasmodics (e.g., baclofen), orthopedic surgery.
⭐ The most common form of cerebral palsy is spastic cerebral palsy (~80%), and among preterm infants, spastic diplegia is particularly prevalent.
DCD & Stereotypies - Coordination Quirks & Rhythms
- Developmental Coordination Disorder (DCD)
- Motor skills (e.g., catching, writing) below age; appears clumsy.
- Significantly impacts Activities of Daily Living (ADLs), academics, or play.
- Not due to intellectual disability, visual impairment, or neurological conditions (e.g., Cerebral Palsy).
- 📌 Difficult Coordination Disorder.
- Stereotypic Movement Disorder (SMD)
- Repetitive, driven, purposeless motor acts (e.g., hand flapping, rocking, head banging).
- Interferes with activities or causes self-injury.
- Concern if: Persists >4 weeks, injurious, or functionally impairing. Not due to substance/other conditions.
⭐ DCD diagnosis: motor difficulties must significantly interfere with activities of daily living or academic achievement, and are not better explained by intellectual disability or visual impairment.
Tic Disorders & Tourette's - Unwanted Moves & Sounds
-
Tics: Sudden, rapid, recurrent, nonrhythmic motor movements or vocalizations.
- Motor Tics: Simple (e.g., eye blinking, head jerking) or Complex (e.g., facial gestures, jumping).
- Vocal Tics: Simple (e.g., throat clearing, sniffing) or Complex (e.g., words, echolalia, coprolalia - rare).
-
Tourette Syndrome (TS):
- Diagnostic Criteria (DSM-5):
- Multiple motor tics AND ≥1 vocal tics (need not be concurrent).
- Tics persist >1 year since first tic onset.
- Onset before age 18 years.
- Not attributable to substance or other medical condition.
- 📌 Mnemonic: TICS (Time >1yr, Involuntary, Combination of motor/vocal, Start <18yrs).
- Common Comorbidities: ADHD (most common, ~60%), OCD (~30-50%).
- Diagnostic Criteria (DSM-5):
⭐ Tourette Syndrome is characterized by both multiple motor tics and at least one vocal tic, present for more than a year, with onset before the age of 18.
Motor Delay Approach - Spotting Stumbles Early
Motor delay: Significant lag in achieving milestones (e.g., >2 SD below mean or <5th percentile).
- Key Milestones (Approx. Age):
- Head control: 2-3 months
- Rolls over: 4-6 months
- Sits unsupported: 6-8 months
- Walks alone: 12-15 months
- Red Flags: 📌 REGRESS (Regression, Early rolling/handedness <18m, Gross motor only delay, Reflexes persistent [Moro >4-6m, ATNR >6m], Eyes abnormal, Stiff/floppy).
- Other: Asymmetry, plateau/loss of skills.
- Brief DDx: Cerebral Palsy, Muscular Dystrophies, SMA, Genetic Syndromes.
⭐ Regression of previously achieved motor milestones is a significant red flag warranting prompt and thorough investigation.

High-Yield Points - ⚡ Biggest Takeaways
- Cerebral Palsy (CP) is a non-progressive motor disorder from perinatal brain injury; spastic type is most common.
- Developmental Coordination Disorder (DCD) involves impaired motor coordination affecting daily life, not due to other conditions.
- Tourette Syndrome: Multiple motor and ≥1 vocal tics for >1 year, onset <18 years.
- Gower's sign indicates proximal muscle weakness, classic in Duchenne Muscular Dystrophy (DMD).
- Spinal Muscular Atrophy (SMA) is a key cause of floppy infant due to LMN degeneration.
- Early intervention is critical for improving outcomes in motor disorders.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

