Foundations - Safe Space Chat
- Goal: Establish trust; ensure child feels safe, supported.
- Environment:
- Private, quiet, comfortable, age-appropriate.
- Minimal distractions. No authority figures/alleged perpetrator present initially.
- Interviewer:
- Empathetic, patient, non-judgmental, calm.
- Use child-friendly language.
- Initial Steps:
- Introduce self & role.
- Explain interview purpose (age-appropriately).
- Confidentiality & its limits (mandatory reporting of harm).
- Build rapport: non-leading, open-ended questions first.
- Ensure child's physical comfort (e.g., water, toilet break).
- Positioning:
- Sit at child's eye level; maintain open, non-threatening posture.
- Avoid physical barriers (e.g., large desk between interviewer and child).

⭐ High-Yield: Always inform the child about the limits of confidentiality, especially regarding mandatory reporting of abuse, before substantive questioning begins. This builds trust and manages expectations.
Child Interview - Kiddo Confabs
Error generating content for this concept group: No object generated: the tool was not called.
Caregiver Interview - Guardian Grills
- Objective: Elicit facts, assess caregiver's perspective, capacity, and willingness to protect child.
- Interview caregivers separately if possible to avoid collusion or intimidation.
- Approach: Non-judgmental, empathetic yet firm; build rapport.
- Key Areas to "Grill" (Explore):
- Child's daily routine, behavior, development.
- Caregiver's understanding of the injury/neglect; consistency of explanation.
- Family stressors, support systems, coping mechanisms.
- Discipline methods used; views on discipline.
- Explanation for any delays in seeking medical care.
- 📌 C.A.R.E.F.U.L. Interview: Calm & Attentive, Rapport building, Explore explanations, Focus on child, Understand stressors, Listen actively.
- Note inconsistencies, evasiveness, blaming the child, or hostility.
⭐ A caregiver's plausible explanation for an injury that is inconsistent with the child's developmental stage or the nature of the injury is a major red flag for abuse.
Documentation & Reporting - Record & Report
Documentation:
- Objective, factual, detailed, contemporaneous.
- 📌 F.A.C.T.S.: Factual, Accurate, Complete, Timely, Specific.
- Child's exact words (verbatim quotes).
- Body diagrams for injuries (location, size, shape, color).
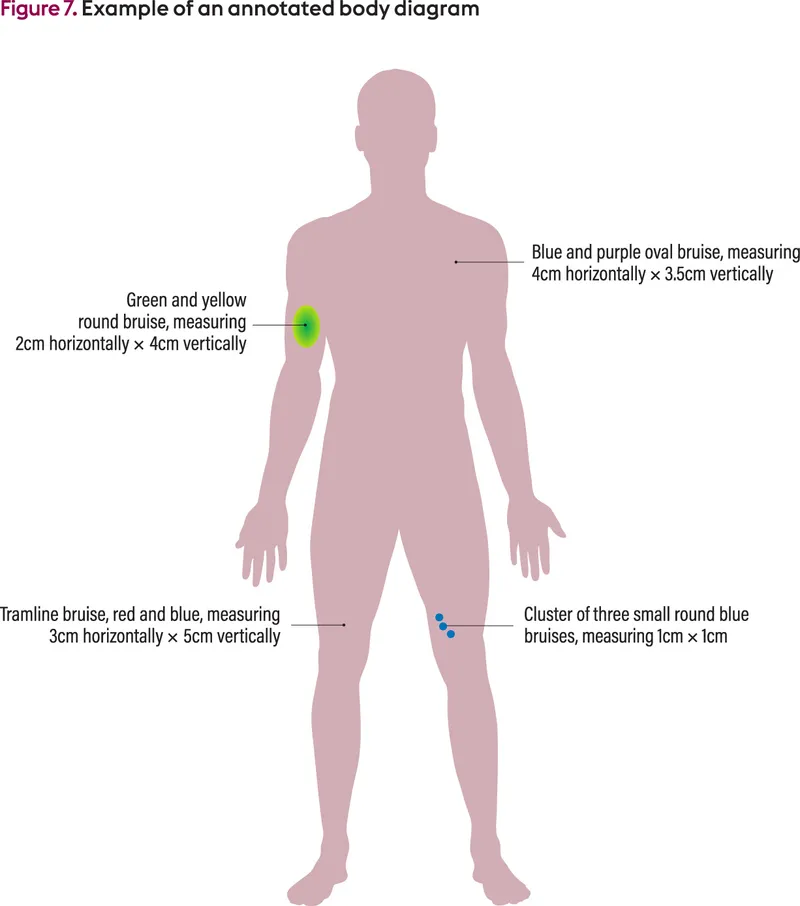
- Record date, time, persons present.
Reporting (POCSO Act, 2012):
- Mandatory for all suspected cases.
- To: Special Juvenile Police Unit (SJPU) or local police.
- Timeline: Within 24 hours of knowledge.
- Inform Child Welfare Committee (CWC).
- Maintain strict confidentiality.
⭐ Section 21, POCSO Act: Failure to report by persons in authority (e.g., doctors) is punishable by imprisonment up to 6 months and/or fine.
High‑Yield Points - ⚡ Biggest Takeaways
- Prioritize open-ended questions initially, allowing the child's spontaneous recall.
- Maintain a neutral, supportive, non-judgmental attitude throughout the interview.
- Strictly avoid leading questions or suggesting information to the child.
- Interview the child alone if abuse is suspected, ensuring a private setting.
- Use age-appropriate language and developmentally sensitive communication.
- Document verbatim the child's statements accurately and objectively.
- Carefully observe and note non-verbal cues and behavioral responses during the interview.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

