Atherosclerosis: Definition & Risks - Hardening Arteries 101
Atherosclerosis: Chronic inflammation forming intimal fibro-fatty plaques (atheromas), causing arterial wall thickening, hardening, and stenosis.
- Key Non-Modifiable Risk Factors:
- Increasing Age
- Male Gender
- Family History
- Genetic Predisposition
- Key Modifiable Risk Factors:
- Hyperlipidemia (↑LDL, ↓HDL, ↑Triglycerides)
- Hypertension (e.g., BP > 130/80 mmHg)
- Cigarette Smoking
- Diabetes Mellitus
- Obesity (BMI ≥ 30 kg/m²)
- Physical Inactivity
- Chronic Inflammation (e.g., ↑hs-CRP)

⭐ Hyperlipidemia (especially ↑LDL cholesterol) and cigarette smoking are the two most significant and modifiable risk factors accelerating atherogenesis.
Atherosclerosis: Pathogenesis - Plaque's Evil Plan
- Trigger: Endothelial injury (↑ permeability, leukocyte adhesion).
- Key Events:
- LDL insudation & oxidation (oxLDL).
- Monocytes → Macrophages → Foam cells (engulf oxLDL).
- Smooth Muscle Cell (SMC) migration, proliferation, ECM deposition → Fibrous cap.
- Necrotic core (lipids, debris) development.
- Outcome: Complex plaque → Calcification, rupture, thrombosis.
⭐ Oxidized LDL (oxLDL) is pivotal, driving inflammation and macrophage transformation into foam cells.

Atherosclerosis: Morphology - Anatomy of Atheroma
- Atheromatous Plaque (Atheroma): Focal intimal thickening; hallmark of atherosclerosis.
- Key Structural Components:
- Fibrous Cap: Superficial layer.
- Composition: Smooth muscle cells (SMCs), dense collagen, elastin, proteoglycans.
- Cells: Macrophages, T-lymphocytes.
- Necrotic Core (Lipid Core): Central part, deep to cap.
- Composition: Cholesterol crystals/esters, necrotic debris, foam cells (lipid-laden macrophages), fibrin, calcium.
- Shoulder Region: Junction of cap and normal arterial wall; most cellular area.
- Composition: Macrophages, T-cells, SMCs.
- Fibrous Cap: Superficial layer.
- Neovascularization: Proliferation of small blood vessels at plaque periphery.
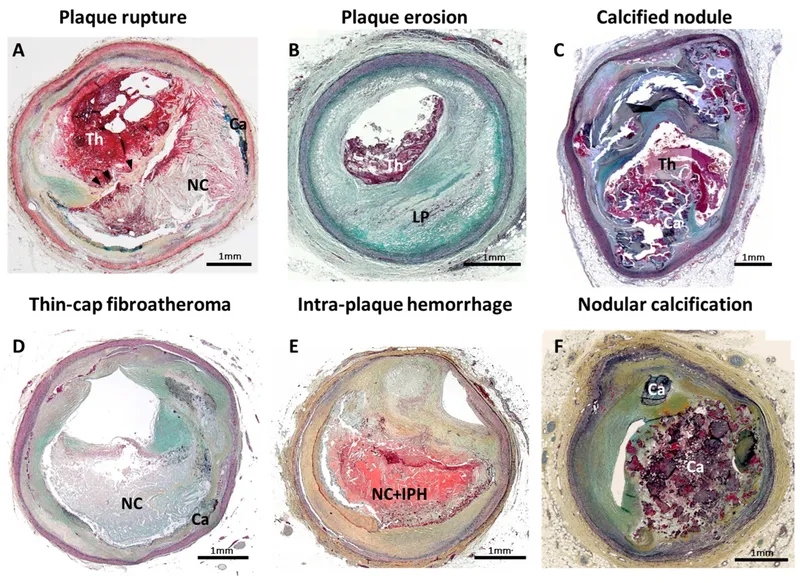
- Key Structural Components:
⭐ The shoulder region, rich in inflammatory cells (macrophages, T-cells), is the most common site for plaque rupture, leading to thrombosis and acute coronary syndromes.
Atherosclerosis: Clinical Sequelae - Arterial Blockage Woes
- Coronary Artery Disease (CAD): Angina, Myocardial Infarction (MI).
- Cerebrovascular Disease (CVD): Transient Ischemic Attack (TIA), Stroke.
- Peripheral Arterial Disease (PAD): Intermittent claudication, gangrene.
- Aneurysms: Aortic (abdominal most common), iliac.
- Renal Artery Stenosis: Secondary hypertension, renal failure.

⭐ Most common site for atherosclerosis is the abdominal aorta, followed by coronary arteries, popliteal arteries, internal carotid arteries, and circle of Willis.
- Mesenteric Ischemia: Bowel infarction.
- Sudden cardiac death often due to plaque rupture/thrombosis in CAD.
Atherosclerosis: Prevention Basics - Plaque Defense Tips
- Lifestyle Modification:
- Diet: ↓Saturated/trans fats, ↑fruits, vegetables, fiber.
- Exercise: Aerobic, ≥150 min/week.
- Smoking cessation.
- Weight management: BMI <25 kg/m².
- Pharmacological:
- Statins (LDL-C goal <70-100 mg/dL based on risk).
- Antiplatelet agents (e.g., Aspirin).
- Blood pressure control (target <130/80 mmHg).
⭐ Statins are first-line for primary and secondary prevention of atherosclerotic cardiovascular disease (ASCVD).
High‑Yield Points - ⚡ Biggest Takeaways
- Most common sites: Abdominal aorta > coronary > popliteal > carotid arteries.
- Initiating event: Chronic endothelial injury/dysfunction.
- Hallmark lesion: Atheromatous plaque (fibrous cap, necrotic lipid core).
- Major modifiable risks: Smoking, hypertension, diabetes, hyperlipidemia (↑LDL, ↓HDL).
- Earliest lesion: Fatty streaks (lipid-laden macrophages/foam cells).
- Key complications: Myocardial infarction, stroke, aortic aneurysms, peripheral vascular disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

