Intro & Etiology - Pancreas Under Siege
Chronic pancreatitis (CP): Progressive, irreversible pancreatic fibro-inflammation with permanent structural damage. Leads to exocrine (maldigestion) & endocrine (diabetes) insufficiency.
- Major Causes (TIGAR-O Classification 📌):
- Toxic-metabolic: Alcohol (most common), smoking, hyperlipidemia.
- Idiopathic.
- Genetic: PRSS1, SPINK1, CFTR mutations.
- Autoimmune pancreatitis.
- Recurrent and severe Acute Pancreatitis.
- Obstructive: Ductal obstruction (tumors, strictures, pancreas divisum).
- Tropical Pancreatitis: Significant in India; early onset, strong SPINK1 gene association.

⭐ Amylase and lipase levels may be normal or only mildly elevated in chronic pancreatitis due to acinar cell loss.
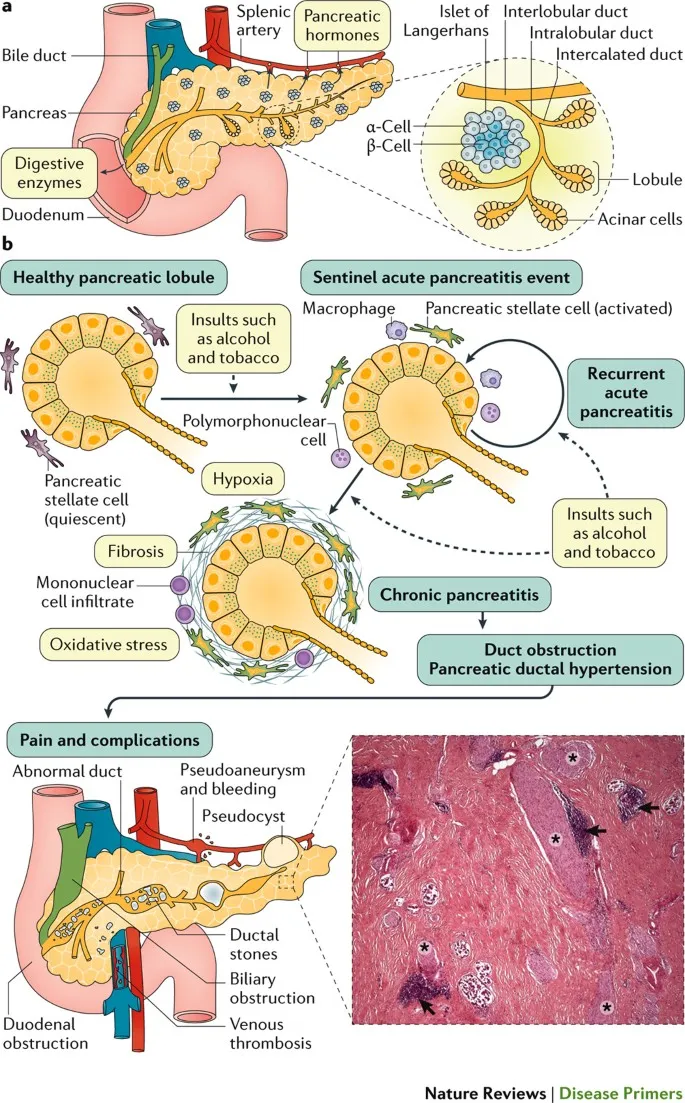
Pathophysiology & Morphology - Scarred & Stonewalled
- Pathophysiology: Recurrent/sustained pancreatic injury activates pancreatic stellate cells (PSCs).
- PSCs deposit collagen → progressive fibrosis, parenchymal destruction.
- Ductal obstruction (protein plugs, stones) → ↑ intraductal pressure.
- Key mechanisms: Necrosis-fibrosis sequence, toxic-metabolic effects, oxidative stress.
- Morphology:
- Gross: Firm, fibrotic, often shrunken gland. Dilated ducts with calcified concretions (stones); "chain of lakes" appearance. Pseudocysts common.
- Micro: Extensive fibrosis, acinar atrophy/loss, chronic inflammatory infiltrate. Islet cells relatively spared until late. Ductal changes: distortion, squamous metaplasia.
⭐ Perineural inflammation is a major contributor to intractable pain.
Clinical Features - The Pain Game
- Dominant Symptom: Persistent or recurrent abdominal pain.
- Location: Epigastric, classically radiating to the back.
- Character: Deep, boring, severe; often post-prandial (15-30 min after meals).
- Exacerbating factors: Alcohol, fatty foods.
- Relieving factors: Leaning forward, fetal position.
- Pain Pattern Evolution:
- Early: Intermittent attacks.
- Late: Can become continuous or, paradoxically, decrease ("burnout phenomenon").
- Associated: Nausea, vomiting, significant weight loss (due to anorexia, food fear).
⭐ Pain "burnout" (decrease in intensity) can occur in late-stage chronic pancreatitis due to progressive destruction of pancreatic parenchyma and nerves, affecting roughly 50% of patients after 5-10 years disease duration an important clinical point for NEET PG aspirants to remember for prognosis related questions
Diagnosis & Investigations - Cracking the Code
- Key Lab Tests:
- Fecal elastase-1: ↓ (sensitive for exocrine insufficiency).
- Serum amylase/lipase: Often normal; may ↑ in flares.
- HbA1c: Monitors for diabetes.
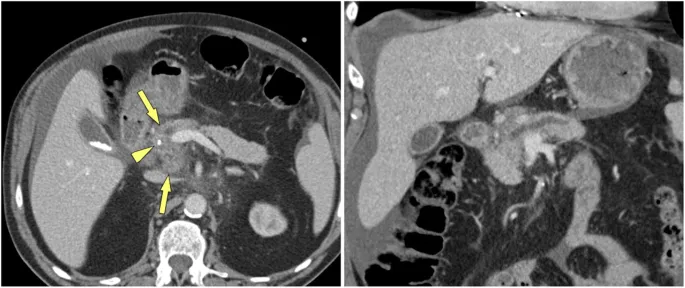
- Imaging Hierarchy:
- CT Scan (CECT): Initial choice; detects calcifications, ductal changes, atrophy.
- MRCP: Superior for ductal anatomy; non-invasive.
- EUS: Highly sensitive for early subtle changes; guides FNA.
- X-ray: Pancreatic calcifications (late).
- ERCP: Diagnostic & therapeutic; invasive.
⭐ Fecal elastase-1 is a highly sensitive and specific non-invasive test for pancreatic exocrine insufficiency, crucial for early detection.
Complications & Management Outline - Damage Control
- Key Complications:
- Pseudocysts (most common), abscess, pancreatic ascites/pleural effusion
- Biliary (CBD) & duodenal stenosis/obstruction
- Vascular: Splenic vein thrombosis (gastric varices), pseudoaneurysms
- Exocrine insufficiency: Malabsorption (steatorrhea, weight loss)
- Endocrine insufficiency: Pancreatogenic diabetes (Type 3c)
- Chronic pain, malnutrition
- ↑ Risk of pancreatic adenocarcinoma
- Management Principles (Damage Control):
- Strict alcohol/smoking cessation
- Pancreatic enzyme replacement therapy (PERT)
- Analgesia (multimodal approach)
- Nutritional support (low fat diet, vitamins)
- Endoscopic therapy (sphincterotomy, stenting, stone extraction)
- Surgical intervention (drainage, resection) for refractory pain/complications

⭐ Patients with hereditary pancreatitis have a lifetime pancreatic cancer risk as high as 40-50%.
High‑Yield Points - ⚡ Biggest Takeaways
- Alcohol abuse (adults) and Cystic Fibrosis (children) are primary causes.
- Characterized by irreversible pancreatic fibrosis, leading to exocrine and endocrine insufficiency.
- Clinical hallmarks: Recurrent/persistent abdominal pain, steatorrhea (malabsorption), and diabetes mellitus.
- Key complications: Pseudocysts, pancreatic ascites, splenic vein thrombosis, and significantly increased pancreatic cancer risk.
- Pancreatic calcifications on imaging (CT/X-ray) are highly diagnostic.
- ERCP/MRCP often shows "chain of lakes" appearance due to ductal strictures and dilations.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

