Resolution of Inflammation - Calm After Storm
- Ideal outcome: Return to normal tissue architecture & function post-acute inflammation.
- Core Processes:
- Removal of injurious stimuli.
- Cessation of pro-inflammatory signals.
- Switch to anti-inflammatory & pro-resolving mediators.
- Neutrophil apoptosis & macrophage-mediated clearance (efferocytosis).
- Drainage of edema fluid & debris.
- Key Pro-Resolving Mediators:
- Anti-inflammatory cytokines: IL-10, TGF-β.
- Specialized Pro-resolving Mediators (SPMs):
- Lipoxins (e.g., LXA₄).
- Resolvins (from EPA/DHA).
- Protectins (from DHA).
- Maresins (from DHA).
- Failure leads to: Chronic inflammation, scarring, or abscess.
⭐ SPMs like Lipoxins and Resolvins actively drive resolution, not just passive decay of inflammation.
Resolution of Inflammation - The Peacekeepers
- Goal: Complete restoration of tissue structure & function. Active, programmed process.
- Triggers: Removal of offending agent.
- Key Events:
- Cessation of pro-inflammatory signals (e.g., leukotrienes switch to lipoxins).
- Neutrophil apoptosis & subsequent efferocytosis by macrophages.
- Clearance of edema fluid & proteins via lymphatics.
- Macrophage phenotype switch: M1 (pro-inflammatory) → M2 (anti-inflammatory, pro-repair).
- Specialized Pro-resolving Mediators (SPMs): 📌 "LRPM" (Lipoxins, Resolvins, Protectins, Maresins)
- Lipoxins (LXA4, LXB4): Inhibit neutrophil chemotaxis, stimulate monocyte recruitment.
- Resolvins (E-series from EPA, D-series from DHA): Reduce PMN infiltration, enhance efferocytosis.
- Protectins (e.g., Neuroprotectin D1 from DHA): Potent anti-inflammatory.
- Maresins (MaR1 from DHA, by macrophages): Stimulate tissue regeneration.
- Anti-inflammatory Cytokines: IL-10, TGF-β.
⭐ Lipoxins are unique as they are generated through transcellular biosynthesis, often involving neutrophil-platelet or neutrophil-epithelial cell interactions, signifying a "stop signal" for inflammation.
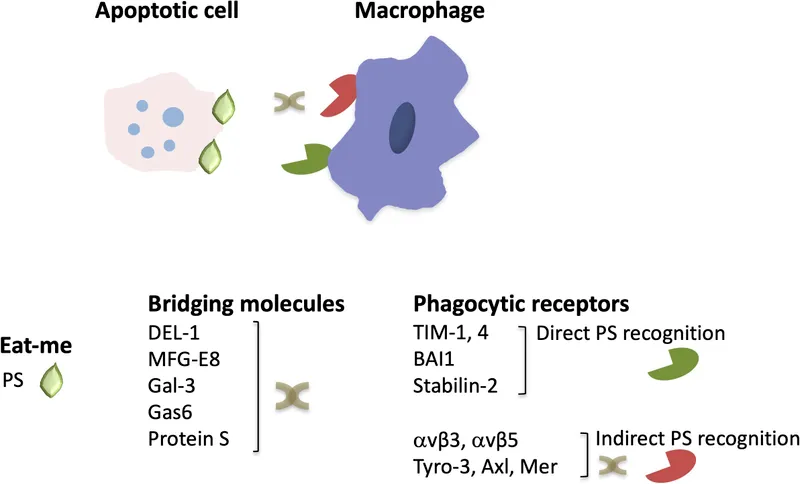
Resolution of Inflammation - Clean Sweep
Active, programmed return to homeostasis; not passive decay. Switches off pro-inflammatory signals, actively clears cells & debris.
- Hallmarks & Mechanisms:
- Cessation of stimulus: Removal of offending agent.
- Mediator Switch: From pro-inflammatory (e.g., Leukotrienes, Prostaglandins) to anti-inflammatory.
- Specialized Pro-resolving Mediators (SPMs): Lipoxins, Resolvins (e.g., RvE1, RvD1), Protectins, Maresins. 📌 (LRPM: "Let Resolution Promote Mend")
- Anti-inflammatory cytokines: IL-10, TGF-β.
- Stop signals: Inhibit leukocyte recruitment.
- Cellular Cleanup:
- Neutrophil apoptosis & subsequent efferocytosis (engulfment by macrophages).
- Macrophage phenotype switch: M1 (pro-inflammatory) → M2 (anti-inflammatory, pro-repair).
- Debris Clearance: Edema, proteins, necrotic cells via lymphatics & phagocytosis.
- Outcome: Tissue regeneration or repair (scarring).

⭐ Lipoxins (e.g., LXA4, LXB4) are key SPMs that inhibit neutrophil chemotaxis and adhesion, stimulate monocyte recruitment, and promote efferocytosis, acting as "braking signals" for acute inflammation.
Resolution of Inflammation - Healing Hiccups
- Ideal Outcome: Complete restoration of normal tissue structure & function.
- "Hiccups" - Factors Impeding Resolution:
- Persistent injurious agent (e.g., M. tuberculosis)
- Extensive necrosis or non-regenerating tissue
- Inadequate drainage (e.g., empyema)
- Foreign bodies
- Impaired host immunity
- Alternative Outcomes if Resolution Fails:
- Chronic Inflammation: Ongoing inflammation, angiogenesis, fibrosis.
⭐ Persistent macrophage activation (e.g., epithelioid, giant cells) is key in chronic inflammation, often driving fibrosis.
- Fibrosis/Scarring: Replacement by connective tissue; loss of function.
- Abscess Formation: Localized pus (neutrophils, necrotic cells, edema fluid) walled off by fibrous tissue.
- Chronic Inflammation: Ongoing inflammation, angiogenesis, fibrosis.

High‑Yield Points - ⚡ Biggest Takeaways
- Resolution is the ideal outcome, restoring normal tissue structure and function post-inflammation.
- Driven by Specialized Pro-resolving Mediators (SPMs) like lipoxins, resolvins, and protectins.
- Involves neutrophil apoptosis, efferocytosis by M2 macrophages, and cessation of leukocyte influx.
- M2 macrophages clear debris and release anti-inflammatory cytokines (e.g., IL-10, TGF-β).
- Failure leads to chronic inflammation, fibrosis, or abscess formation.
- Favored by minimal tissue damage and rapid removal of the injurious stimulus.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

