Malabsorption: Intro & Mechanisms - Gut Feeling Gone Wrong
- Definition: Impaired intestinal absorption of nutrients, leading to deficiencies & GI symptoms (diarrhea, steatorrhea, weight loss).
- Mechanisms:
- Intraluminal Phase: Defective hydrolysis or solubilization.
- E.g., Pancreatic insufficiency, Zollinger-Ellison syndrome, bacterial overgrowth, bile salt deficiency.
- Mucosal Phase: Impaired epithelial transport.
- E.g., Celiac disease, tropical sprue, Whipple's disease, lactase deficiency.
- Post-mucosal Phase (Transport): Lymphatic obstruction.
- E.g., Intestinal lymphangiectasia, lymphoma.

- E.g., Intestinal lymphangiectasia, lymphoma.
- Intraluminal Phase: Defective hydrolysis or solubilization.
⭐ Steatorrhea (bulky, foul-smelling, fatty stools) is a hallmark of generalized malabsorption, particularly of fats due to impaired digestion or absorption across the intestinal mucosa or lymphatic transport issues. It often presents when fat malabsorption exceeds 7g/day (normal <6g/day).
Malabsorption: Clinical Clues & Workup - Spotting the Signs
- Clinical Clues:
- GI: Steatorrhea (bulky, greasy stools), weight loss, distension, flatulence.
- Systemic: Anemia (Fe, B12, folate ↓), bone pain (Ca, Vit D ↓), edema (protein ↓), neuropathy (B12 ↓), bleeding (Vit K ↓).
- Initial Workup:
- Stool: Sudan III stain; 72-hr fecal fat (>7 g/day).
- Blood: CBC, iron studies, B12/folate, albumin, Ca, PT/INR.
- Diagnostic Approach:
⭐ Steatorrhea (>7 g/24h fecal fat) is a key indicator of malabsorption.
Celiac Disease - Gluten's Gut Grudge
- Immune-mediated enteropathy triggered by gluten (gliadin in wheat, barley, rye) in genetically predisposed (HLA-DQ2/DQ8) individuals.
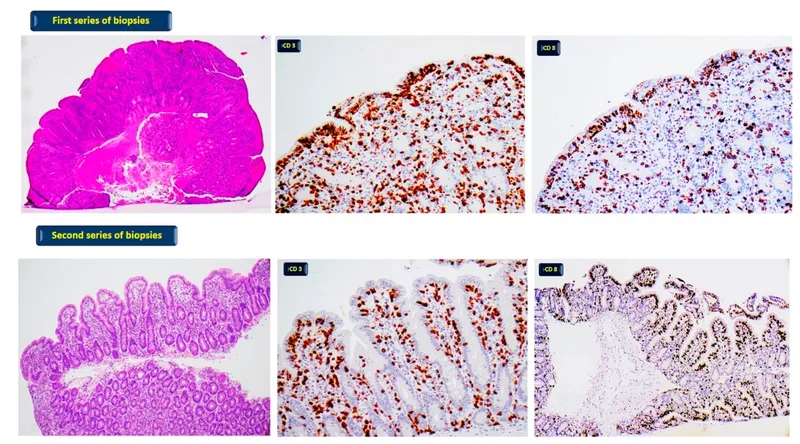
- Pathology: Small intestinal inflammation (esp. duodenum, proximal jejunum) → villous atrophy, crypt hyperplasia, ↑ intraepithelial lymphocytes (IELs).
- Clinical Features: Chronic diarrhea, steatorrhea, weight loss, abdominal pain, bloating. Children: failure to thrive. Iron deficiency anemia is common.
- Diagnosis:
- Serology: IgA anti-tissue transglutaminase (tTG) antibodies (screening); IgA anti-endomysial (EMA) antibodies (highly specific); Anti-deamidated gliadin peptide (DGP) antibodies.
- Duodenal biopsy: Confirmatory; shows villous atrophy (Marsh classification).
- Management: Lifelong strict gluten-free diet (GFD).
- Complications: Malabsorption, osteoporosis, infertility, dermatitis herpetiformis, increased risk of T-cell lymphoma (EATL) & small bowel adenocarcinoma.
⭐ > Dermatitis herpetiformis, an intensely pruritic papulovesicular rash typically on extensor surfaces (elbows, knees, buttocks), is a cutaneous manifestation highly specific for celiac disease.
Other Key Syndromes - The Malabsorption Medley
-
Whipple Disease:
- Infection by Tropheryma whipplei (Gram-positive actinomycete).
- Symptoms: Arthralgia, weight loss, diarrhea, abdominal pain, neurological & cardiac issues. 📌 Mnemonic: "Foamy Whipped cream in a CAN" (Foamy macrophages, Cardiac, Arthralgia, Neurologic).
- Dx: PAS-positive macrophages in intestinal biopsy; PCR. Rx: Prolonged antibiotics (e.g., Ceftriaxone then TMP-SMX).
⭐ PAS-positive, diastase-resistant granules in foamy macrophages within the small intestinal lamina propria are characteristic of Whipple disease.
-
Tropical Sprue:
- Etiology unclear (?post-infectious); affects residents/visitors of tropical areas.
- Features: Chronic diarrhea, steatorrhea, weight loss, megaloblastic anemia (folate & B12 deficiency).
- Biopsy: Villous atrophy (milder than celiac), ↑intraepithelial lymphocytes, chronic inflammation. Rx: Tetracycline & folic acid.
-
Short Bowel Syndrome:
- Reduced absorptive surface area post-surgical resection (e.g., Crohn's, volvulus).
- Complications: Malnutrition, diarrhea, electrolyte imbalance, ↑oxalate kidney stones, gallstones.
-
Lactase Deficiency (Lactose Intolerance):
- Deficiency of lactase enzyme (primary: adult-onset; secondary: mucosal injury).
- Symptoms: Osmotic diarrhea, bloating, flatulence after lactose ingestion.
- Dx: Lactose hydrogen breath test; empirical trial of lactose-free diet.
High‑Yield Points - ⚡ Biggest Takeaways
- Celiac disease: HLA-DQ2/DQ8 linked, anti-tTG IgA positive; villous atrophy, crypt hyperplasia.
- Tropical sprue: Affects jejunum & ileum; responds to antibiotics, folate.
- Whipple disease: Tropheryma whipplei infection; PAS-positive macrophages in lamina propria.
- Lactase deficiency: Osmotic diarrhea; normal villous morphology.
- Pancreatic insufficiency: Steatorrhea from impaired fat digestion; common in chronic pancreatitis.
- D-xylose test: Differentiates mucosal disease (abnormal) from pancreatic insufficiency (normal).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

