Basics & Classification - Intro & Ouchies
- Soft Tissue Injury (STI): Damage to non-bony tissues (muscle, tendon, ligament, bursa, nerve, vessel).
- Classification:
- By Onset:
- Acute: Sudden (direct blow, overload, overstretch).
- Chronic: Overuse (e.g., tendinopathy).
- By Skin Integrity:
- Closed: Skin intact.
- Open: Skin breached.
- By Onset:
- Contusion (Bruise): Capillary rupture from blunt trauma; features pain, swelling, ecchymosis.
- Hematoma: Larger vessel damage; forms localized blood collection (mass); features pain, possible fluctuance.

- Healing Phases:
- Inflammation (0-7 days): Hemostasis, cellular influx.
- Proliferation (3-21 days): Fibroplasia, angiogenesis.
- Remodeling (Day 21 - 2 yrs): Collagen maturation, scar strengthening.
⭐ Hematomas often present as a palpable, fluctuant mass due to localized blood collection, distinguishing them from diffuse contusions.
Ligament & Tendon Injuries - Stretch & Snap
-
Sprains (Ligament Injury):
- Grading:
Gr Injury Symptoms Laxity Stability I Micro-tears Mild pain/swell Minimal Stable II Partial tear Mod pain/swell/bruise ↑ (endpt) Mild instab III Complete tear Sev pain/swell/bruise ↑↑ (no endpt) Unstable - Common:
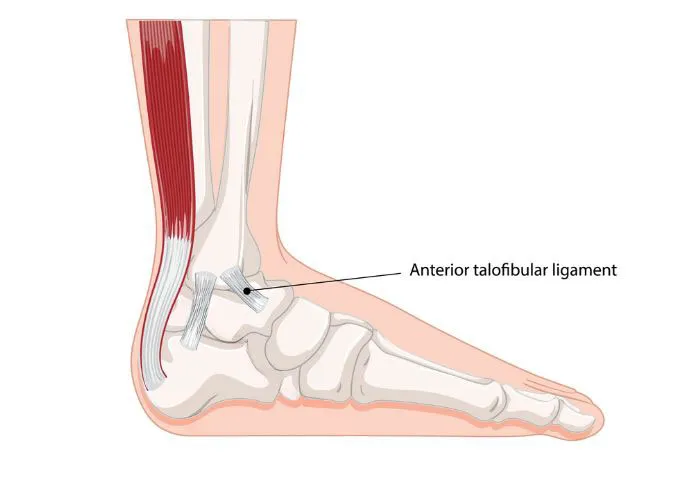
- Ankle: ATFL (most common); Inversion + Plantarflexion. 📌 ATFL: "Always Tears First".
- Knee: ACL (Lachman, Ant Drawer); PCL (Post Drawer); MCL (Valgus); LCL (Varus). Unhappy Triad: ACL, MCL, Medial Meniscus (AMM).
- Grading:
-
Strains (Musculotendinous Injury):
- Grading:
Gr Injury Symptoms Functional Loss I Stretch Mild pain Minimal II Partial tear Mod pain/weakness Moderate III Complete tear Sev pain/LOF Severe - Common: Hamstrings, Quads, Adductors, Rotator cuff.
- Grading:
-
Tendinopathies:
- Tendinitis (acute inflammation) vs. Tendinosis (chronic degen.).
- E.g., Achilles, Tennis elbow (Lat. epicondylitis), Golfer's (Med. epicondylitis).
⭐ ATFL: most common ligament in ankle sprains.
Muscle & Fascia Conditions - Aches & Alerts
- Muscle Injuries:
- Direct: Contusion, laceration.
- Indirect: Strain (see CG2), rupture.
- Delayed Onset Muscle Soreness (DOMS): Self-limiting post-exertional pain.
- Myositis Ossificans:
- Patho: Post-traumatic heterotopic ossification in muscle.
- Sites: Quadriceps, brachialis. Clinically: Pain, swelling, ↓ROM.
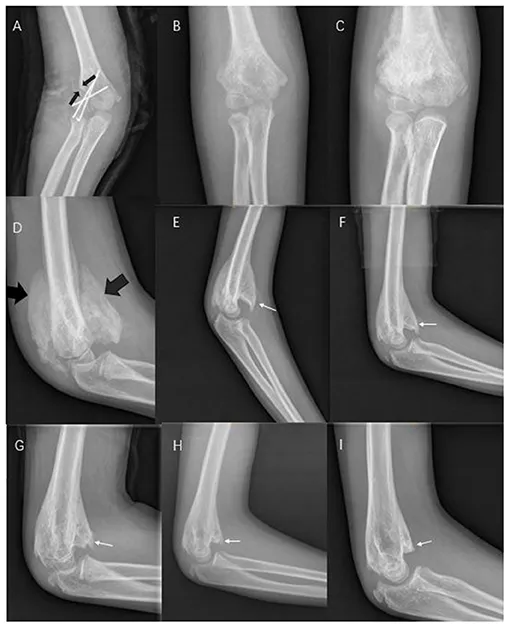
- X-ray: Fluffy calcification → mature peripheral ossification.
- Mgmt: Rest, NSAIDs. ⚠️ AVOID early aggressive massage/surgery.
- Compartment Syndrome:
- Patho: ↑ Intracompartmental pressure (ICP) → ↓ tissue perfusion → ischemia, necrosis.
- Causes: Tibial fractures, crush injuries, burns, tight casts/dressings.
- 📌 6 P's: Pain (out of proportion, earliest sign), Paresthesia, Pallor, Pulselessness, Paralysis, Poikilothermia (late signs).
- Dx: Clinical suspicion crucial. ICP: Normal 0-8 mmHg. Fasciotomy if absolute ICP >30-40 mmHg or $ΔP$ (Diastolic BP - ICP) < 20-30 mmHg.
⭐ Pain out of proportion to injury is the earliest and most reliable clinical sign of compartment syndrome.
- Mgmt: Emergency Fasciotomy.
Nerve Trauma & General Repair - Zaps & Patches
-
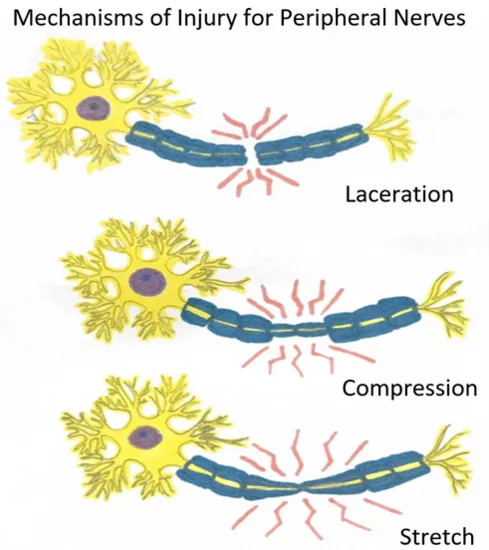
Peripheral Nerve Injury Classification:
Seddon Sunderland Pathology Recovery (Prognosis) Neuropraxia I Myelin damage, axon intact, no Wallerian Full (days-weeks) Axonotmesis II-IV Axon damage, Wallerian degen., sheath variable Variable (1mm/day), may need surgery Neurotmesis V Complete division, Wallerian degen. Surgery essential - EMG: Denervation (fibrillations, +ve sharp waves) in Axonotmesis/Neurotmesis.
-
Common Nerve Palsies: 📌 DR CUMA (Drop wrist - Radial; Claw - Ulnar; Median - Ape/Benediction)
- Axillary n.: Anterior shoulder dislocation → Deltoid paralysis, regimental badge anaesthesia.
- Radial n.: Humerus shaft # → Wrist drop.
- Median n.: Supracondylar #, Carpal Tunnel Syndrome → Ape hand, thenar wasting.
- Ulnar n.: Medial epicondyle # → Claw hand (4th/5th digits), Froment's sign.
- Common Peroneal n.: Fibular neck # → Foot drop, steppage gait.
-
Soft Tissue Management:
- Protection, Optimal Loading, Ice, Compression, Elevation (POLICE). Analgesia.
- Balance immobilization & early mobilization. Physiotherapy crucial.
- Surgical Indications: Complete tears (active individuals), nerve transection, compartment syndrome, failed conservative management.
⭐ Order of sensory recovery: Pain → Temperature → Touch → Proprioception.
High‑Yield Points - ⚡ Biggest Takeaways
- Sprains are ligament injuries; strains involve muscle/tendon units.
- Ottawa Ankle/Knee Rules are crucial for guiding X-ray decisions.
- Compartment syndrome: surgical emergency; pain out of proportion is the earliest reliable sign.
- Achilles tendon rupture: positive Thompson test (absent plantarflexion on calf squeeze).
- Meniscal injuries: joint line tenderness, locking, or clicking; McMurray test is indicative.
- ACL tears: often non-contact pivoting injuries; Lachman test is most sensitive_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

