Overuse Pathophysiology - Strain Game Begins
Overuse injury: Tissue damage from repetitive submaximal loading, where microtrauma accumulation outpaces repair.
- Risk Factors:
- Intrinsic (Host): 📌 "MALES" - Muscle imbalance, Alignment (e.g., genu varum/valgum), Limb length discrepancy, Endurance poor, Strength deficits.
- Extrinsic (Environment): 📌 "TOES" - Training errors (sudden ↑ intensity/duration), Old/improper equipment, Environment (hard surface), Sport technique poor.
- Pathophysiological Stages:
- Microtrauma accumulation.
- Inflammation (acute response).
⭐ Tendinopathy is primarily a degenerative condition ('tendinosis'), not inflammatory, despite common suffix '-itis'.
- Failed healing (repair capacity overwhelmed).
- Degeneration (structural tissue changes).
- Commonly Affected Tissues: Tendons (tendinopathy), bone (stress fractures), bursa (bursitis), fascia (fasciitis).

Upper Limb Overuse - Arm Agonies
- Rotator Cuff Tendinopathy/Impingement:
- Anatomy: 📌 SITS (Supraspinatus, Infraspinatus, Teres minor, Subscapularis) muscles; subacromial space.
- Mechanism: Repetitive overhead activity, compression.
- Tests: Jobe's (supraspinatus), Neer's, Hawkins-Kennedy, Painful arc (60-120° abduction).
⭐ Painful arc syndrome (pain between 60-120° of shoulder abduction) is characteristic of subacromial impingement.
- Lateral Epicondylitis (Tennis Elbow):
- Anatomy: Common extensor origin (esp. ECRB - Extensor Carpi Radialis Brevis).
- Mechanism: Repetitive wrist extension/supination.
- Tests: Cozen's test (resisted wrist extension), Mill's test.
- Medial Epicondylitis (Golfer's Elbow):
- Anatomy: Common flexor origin.
- Mechanism: Repetitive wrist flexion/pronation.
- Tests: Golfer's elbow test (resisted wrist flexion & pronation).

Comparison: Upper Limb Tendinopathies
| Condition | Site | Key Test(s) | Nerve (if relevant) | Sport Example |
|---|---|---|---|---|
| Rotator Cuff Tendinopathy | Subacromial space, SITS tendons | Jobe's, Neer's, Painful Arc | Suprascapular | Swimming, Throwing |
| Lateral Epicondylitis | Lateral epicondyle (Extensor origin) | Cozen's, Mill's | Radial (PIN) | Tennis (backhand) |
| Medial Epicondylitis | Medial epicondyle (Flexor origin) | Golfer's elbow test | Ulnar (sometimes) | Golf, Pitching |
Lower Limb Overuse - Leg Loads
- Patellofemoral Pain Syndrome (PFPS)
- Mechanism: Malalignment, overuse (running, jumping).
- Symptoms: Anterior knee pain, worse with stairs, squatting; "movie-goer's sign".
- $Q-angle$: ↑ angle linked to PFPS. Normal: Male $14°$, Female $17°$.
- Achilles Tendinopathy
- Mechanism: Repetitive microtrauma, overuse.
- Symptoms: Pain/stiffness at posterior heel/calf, worse with activity.
- Test: Pain on palpation, Thompson test (for rupture, not tendinopathy typically).
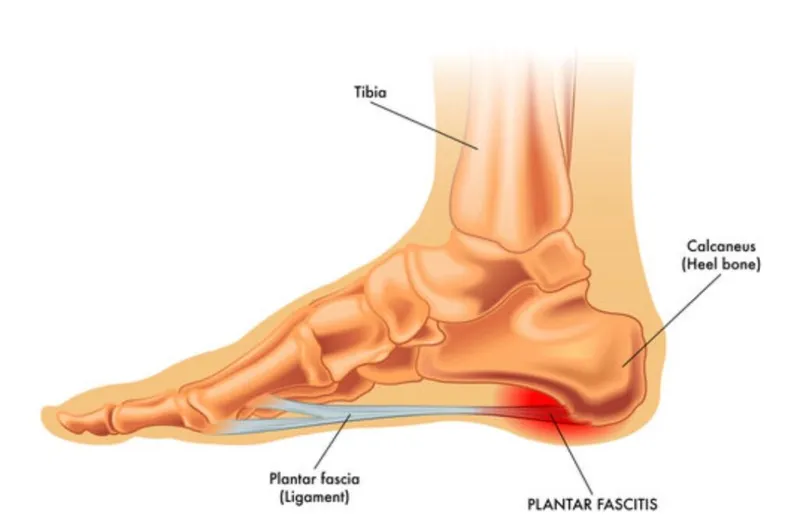
- Plantar Fasciitis
- Mechanism: Inflammation of plantar aponeurosis due to overuse, poor footwear.
- Symptoms: Inferior heel pain, esp. first steps in morning or after rest.
- Test: Windlass test, tenderness at medial calcaneal tuberosity.
- Stress Fractures
- Mechanism: Repetitive submaximal loading (e.g., tibia, metatarsals).
- Symptoms: Insidious onset, localized bone tenderness, pain with activity.
- 📌 Mnemonic (Common sites): "Tired Muscles Take Frequent Falls" (Tarsals, Metatarsals, Tibia, Fibula, Femur).
| Condition | Site of Pain | Aggravating Factors | Key Sign/Test |
|---|---|---|---|
| PFPS | Anterior knee | Stairs, squatting, sitting | Movie-goer's sign |
| Achilles Tendinopathy | Posterior heel/calf | Activity, push-off | Palpable tenderness |
| Plantar Fasciitis | Inferior heel | Morning steps, post-rest | Windlass test |
| Stress Fracture | Localized bone | Weight-bearing activity | Point tenderness |
Overuse Dx & Rx - Fix & Prevent
- Dx Approach:
- History: Training errors (sudden ↑ load, ↓ rest), insidious onset pain.
- Exam: LOOK (swelling), FEEL (point tenderness), MOVE (painful arc), Special Tests.
- Imaging: X-ray (late stress #); USG (tendons, dynamic); MRI (gold standard soft tissue/early stress #).
- Rx - Fix:
- 📌 POLICE principle. Activity modification (relative rest).
- NSAIDs: Short-term; ⚠️ cautious in tendinopathy.
- Rehab: Pain control → ROM → Strength (esp. eccentric) → Proprioception → Gradual RTS.
- Prevention:
- Training: 10% rule (gradual ↑ load).
- Proper technique, equipment, biomechanics.
- Adequate warm-up, cool-down, rest.
⭐ Eccentric exercises are the cornerstone of tendinopathy rehabilitation.
High‑Yield Points - ⚡ Biggest Takeaways
- Overuse injuries: Repetitive microtrauma exceeding tissue repair.
- Hallmark: Pain with activity, relieved by rest; night pain indicates severity.
- Tennis elbow (lateral epicondylitis): ECRB origin; Golfer's elbow (medial): flexor-pronator mass.
- Jumper’s knee: Patellar tendinopathy at inferior patellar pole.
- Stress fractures: Insidious onset point tenderness; initial X-rays often normal.
- Key management: Activity modification, physiotherapy, gradual return to sport.
- Chronic cases are tendinopathy (degenerative) more than tendinitis_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

