Spinal Stenosis: Intro - Canal Calamity
- Spinal canal narrowing; causes nerve root/cord compression.
- Types:
- Central stenosis
- Lateral recess stenosis
- Foraminal stenosis
- Sites:
- Lumbar (commonest, esp. L4-L5, L3-L4)
- Cervical
- Thoracic (rare)
- Key Anatomy: Vertebral body, pedicles, laminae, intervertebral foramen, ligamentum flavum, facet joints, intervertebral disc.
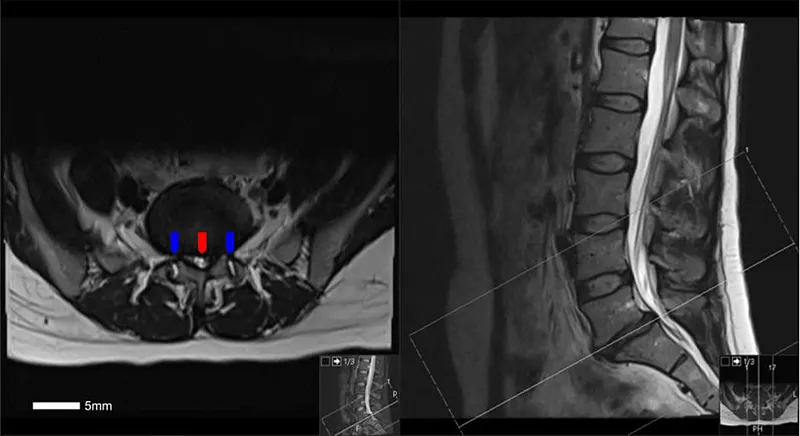
⭐ Degenerative lumbar spinal stenosis most commonly affects the L4-L5 level, followed by L3-L4 and L5-S1.
Spinal Stenosis: Origins - The Narrowing Path
- Congenital: Achondroplasia (results in short pedicles), idiopathic short pedicles.
- Acquired (Most Common):
- Degenerative (Spondylosis): Key factors include disc herniation/bulge, ligamentum flavum hypertrophy, and facet joint arthropathy/osteophytes.
- Spondylolisthesis (vertebral slip).
- Post-traumatic (e.g., fracture malunion).
- Post-surgical (iatrogenic).
- Paget’s disease.
- Pathophysiology: Involves mechanical compression of neural elements (nerve roots/cauda equina), associated vascular compromise (ischemia), and inflammatory mediators.
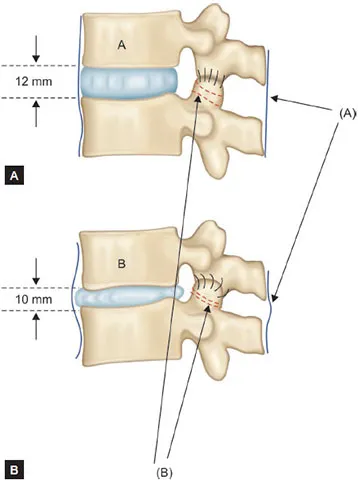
⭐ Hypertrophy of the ligamentum flavum is a key dynamic (buckling with extension) and static contributor to acquired lumbar spinal stenosis, significantly reducing canal diameter.
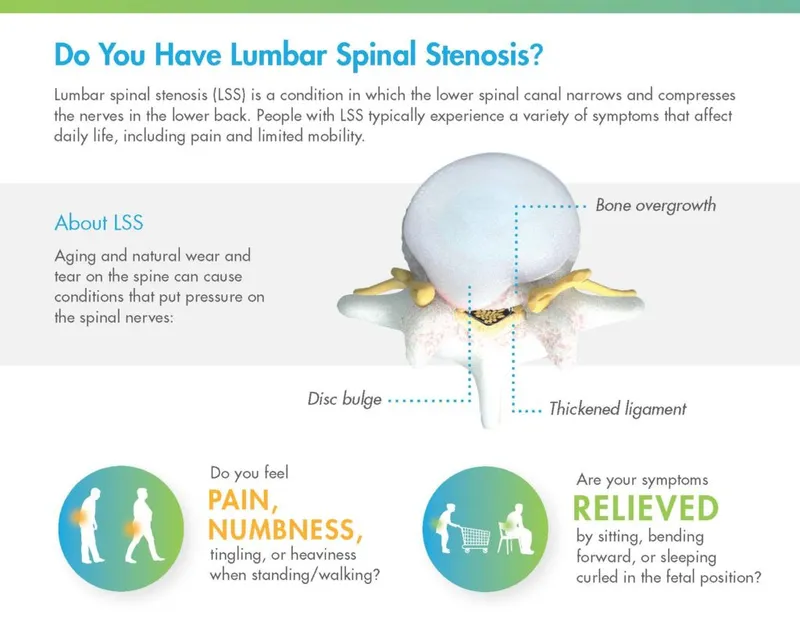
Spinal Stenosis: Symptoms - The Squeeze Sings
- Lumbar Stenosis:
- Neurogenic claudication: Bilateral buttock/thigh/leg pain, numbness, weakness.
- Worse: walking/standing (esp. downhill).
- Relief: lumbar flexion/sitting (📌 'Shopping Cart Sign' / 'Stoop to Conquer').
- Chronic low back pain; radicular pain if foraminal.
- Neurogenic claudication: Bilateral buttock/thigh/leg pain, numbness, weakness.
- Cervical Stenosis:
- Neck pain.
- Radiculopathy: Arm pain, paresthesia, weakness (dermatomal/myotomal).
- Myelopathy: Gait disturbance (spastic, broad-based), clumsiness, UMN signs (Hoffmann's, Babinski), late bowel/bladder dysfunction.
- ⚠️ Cauda Equina Syndrome (RED FLAG):
- Saddle anesthesia.
- Bowel/bladder incontinence/retention.
- Bilateral leg weakness.
⭐ Neurogenic claudication, characterized by pain relief upon lumbar flexion (e.g., leaning forward, sitting), is a hallmark symptom of lumbar spinal stenosis, distinguishing it from vascular claudication.
Spinal Stenosis: Unmasking - The Imaging Insight
- History: Symptom analysis (claudication distance, aggravating/relieving factors, red flags).
- Physical Exam:
- Neurological: Motor, sensory, reflexes (normal/subtle deficits).
- Gait assessment.
- Special tests: SLR (often negative in central stenosis), Kemp’s, Romberg; Hoffman's/Babinski (cervical).
- Imaging:
- X-rays (AP, lat, flex-ext): Alignment, instability, degeneration.
- MRI (GOLD STANDARD): Canal dimensions, disc, lig. flavum, nerve/cord compression.
- CT Myelogram: If MRI C/I; superior bony detail.
⭐ MRI is the imaging modality of choice for diagnosing spinal stenosis, providing excellent visualization of neural structures and soft tissue contributors to the narrowing.
Spinal Stenosis: Action Plan - Relieving the Rule
- Conservative Management (Initial):
- Activity modification, analgesics (NSAIDs, acetaminophen).
- Neuropathic agents (gabapentin, pregabalin), muscle relaxants.
- Physiotherapy: flexion-based exercises, core strengthening.
- Epidural steroid injections (short-term relief).
- Surgical Indications:
- Failure of conservative treatment (typically 3-6 months).
- Progressive/severe neurological deficits (e.g., significant weakness, myelopathy).
- Cauda equina syndrome (EMERGENCY).
- Intractable pain significantly affecting quality of life.
- Surgical Procedures:
- Decompression: Laminectomy, laminotomy, foraminotomy, facetectomy.
- +/- Instrumented Fusion (if instability, significant deformity, or extensive decompression).
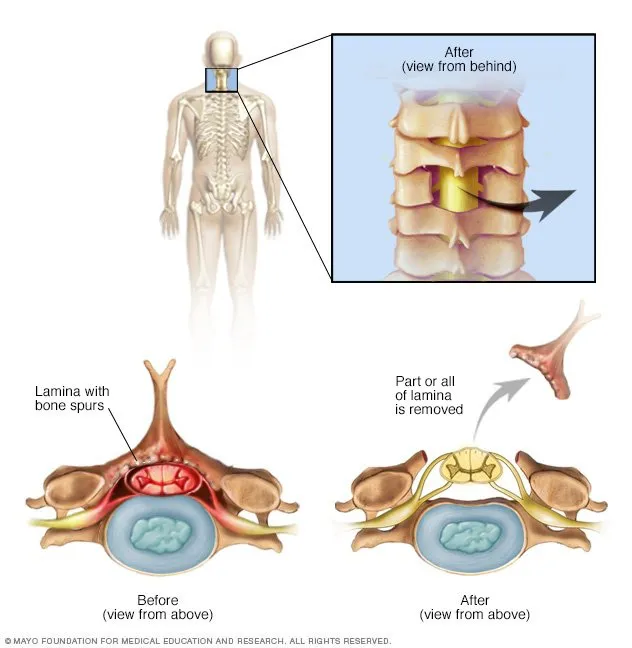
⭐ The primary goal of surgery for spinal stenosis is decompression of the neural elements; fusion is added if there is associated instability or deformity.
High‑Yield Points - ⚡ Biggest Takeaways
- Neurogenic claudication (pseudoclaudication) is pathognomonic: buttock/leg pain with walking.
- Symptoms worsen with lumbar extension (standing, walking downhill), relieved by flexion (sitting, "shopping cart sign").
- Most common in lumbar spine, particularly L4-L5.
- MRI is the investigation of choice for diagnosis.
- Key acquired causes: ligamentum flavum hypertrophy, facet joint arthropathy, disc herniation.
- Definitive treatment for severe symptoms: surgical decompression (e.g., laminectomy).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

