Lumbar Anatomy & Biomechanics - Backbone Basics
- Vertebrae: 5 (L1-L5); largest, kidney-shaped bodies. Normal lordosis.
- Intervertebral Discs (IVD):
- Nucleus Pulposus: Gelatinous core (Type II collagen, GAGs); shock absorption.
- Annulus Fibrosus: Lamellar rings (Type I collagen); tensile strength.
- Facet Joints (Zygapophyseal): Sagittally oriented; guide flexion/extension, limit rotation.
- Ligaments: ALL (limits extension), PLL (limits flexion, weaker), Ligamentum Flavum (elastic, connects laminae).
- Neural Elements: Conus medullaris typically ends at L1-L2. Cauda equina below.
- Biomechanics: Major weight-bearing. Flexion opens intervertebral foramina; extension narrows them.

⭐ The sinuvertebral nerve (recurrent nerve of Luschka) innervates the posterior annulus fibrosus, PLL, and dura mater, mediating discogenic pain.
Lumbar Disc Herniation - Disc Drama
*Nucleus pulposus (NP) herniation through annulus fibrosus (AF), usually posterolateral. *Common levels: L4-L5, L5-S1. *Clinical: Sciatica (radicular pain), paresthesia, weakness. Positive Straight Leg Raise (SLR). *Nerve root compressed by disc at level:
- L3-L4 disc (L4 root): Weak quads (📌 kick door), ↓ knee jerk, medial leg sensory loss.
- L4-L5 disc (L5 root): Weak dorsiflexion (foot drop; 📌 heel walk), lat leg/dorsum foot sensory loss.
- L5-S1 disc (S1 root): Weak plantarflexion (📌 toe walk), ↓ ankle jerk, post calf/lat foot sensory loss. *Diagnosis: MRI (gold standard). X-ray to exclude other issues. *Management:
- Conservative: Rest, NSAIDs, physiotherapy.
- Surgical (Discectomy): For cauda equina syndrome (CES), progressive neuro deficit, or failed conservative Rx (>6 weeks).
⭐ Posterolateral L5-S1 herniation most commonly compresses S1 nerve root.
Lumbar Canal Stenosis & Spondylolisthesis - Narrow Escapes & Slips
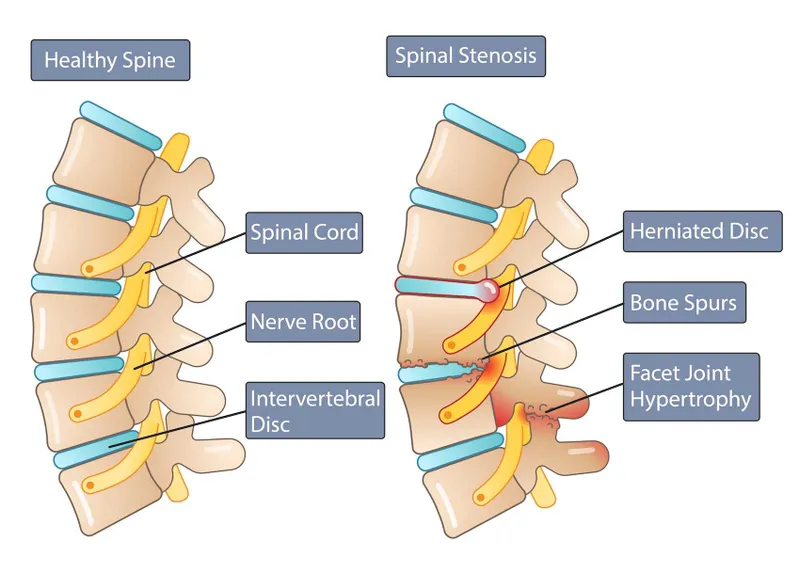
Lumbar Canal Stenosis (LCS)
- Narrowing: Spinal, lateral recess, or foraminal.
- Cause: Degenerative (commonest), congenital.
- hallmark: Neurogenic claudication (leg pain/weakness on walking, relieved by flexion/sitting 📌 "Shopping cart sign").
- Dx: MRI.
- Rx: Conservative; Surgery (decompression) if severe.
Spondylolisthesis
- Slippage: Anterior vertebral displacement.
- Types:
- Isthmic (pars defect; "Scottie dog" X-ray).
- Degenerative (facet arthropathy; often with LCS).
- Symptoms: LBP, radiculopathy, +/- claudication.
- Meyerding Grade: I (<25%), II (25-50%), III (50-75%), IV (75-100%), V (>100%).
- Rx: Conservative; Surgery (fusion) for high grade/instability.
⭐ Isthmic spondylolisthesis (Type II) is most common at L5-S1, often from pars interarticularis fracture (spondylolysis).
Red Flags & Cauda Equina Syndrome - Spine Emergencies!
-
Red Flags (Back Pain):
- Age <20 or >55 years (new onset)
- Trauma (significant)
- Unexplained weight loss, fever, night sweats (constitutional symptoms)
- History of cancer, immunosuppression, IV drug use
- Neurological deficit: motor weakness, sensory loss, bladder/bowel dysfunction
- Nocturnal pain, pain at rest
- Thoracic pain
- Saddle anesthesia
-
Cauda Equina Syndrome (CES): Spinal cord compression below L1-L2 (conus medullaris)
- Severe low back pain
- Bilateral sciatica
- Saddle anesthesia (perineal numbness S2-S5 dermatomes)
- Bowel/bladder dysfunction (urinary retention/incontinence, fecal incontinence)
- Lower extremity weakness, ↓ reflexes
- Sexual dysfunction
- 📌 Mnemonic SADDLE: Saddle anesthesia, Ankle/foot weakness, Diminished reflexes, Dribbling (urinary retention), Leg pain (bilateral), Erectile dysfunction.

⭐ Urinary retention (post-void residual volume >200 mL) is a strong predictor of Cauda Equina Syndrome and warrants immediate investigation.
High‑Yield Points - ⚡ Biggest Takeaways
- Lumbar disc prolapse: Most common at L4-L5 & L5-S1 levels; typically posterolateral herniation.
- Cauda Equina Syndrome: Surgical emergency! Key signs: saddle anesthesia, bowel/bladder dysfunction, and bilateral leg weakness.
- Positive Straight Leg Raise (SLR) test: Indicates lumbosacral radiculopathy (e.g., L4-S1 nerve root irritation from disc herniation).
- Lumbar spinal stenosis: Presents with neurogenic claudication (pain/numbness worse with standing/walking, relieved by flexion).
- Spondylolisthesis: Anterior vertebral slip; isthmic type (pars interarticularis defect) common in young athletes, may show "Scottie dog" sign.
- Red flags for low back pain: Include night pain, unexplained weight loss, progressive neurological deficits, fever, history of cancer or IV drug use.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

