Spine Disorders

On this page
🏗️ Spine Disorders: The Vertebral Architecture Mastery
Your spine bears the mechanical burden of upright life, translating forces through an elegant column of bone, disc, and ligament-yet this same architecture becomes a common source of pain and disability when loading patterns exceed tissue capacity. You'll master how vertebral anatomy dictates injury patterns, recognize clinical syndromes through systematic examination, and deploy evidence-based algorithms that distinguish benign mechanical pain from serious pathology requiring urgent intervention. By integrating biomechanics, diagnostic reasoning, and rehabilitation principles, you'll build the clinical expertise to confidently evaluate and manage the full spectrum of spine disorders.

The Spinal Engineering Blueprint
The spine functions as a sophisticated load-bearing column with 24 mobile segments creating a triple-curve architecture that distributes mechanical stress across multiple planes. Each functional spinal unit (FSU) consists of 2 adjacent vertebrae with their interconnecting disc, facet joints, and ligamentous structures.
- Cervical Lordosis: 20-40° curvature accommodating 12-15 pounds of head weight
- C1-C2 complex: 50% of cervical rotation (90° total)
- C5-C6 level: Most common disc herniation site (60% of cases)
- Vertebral arteries: 3mm diameter foramina vulnerability
- Thoracic Kyphosis: 20-50° curvature with rib cage stabilization
- T12-L1 junction: 70% of thoracolumbar fractures
- Costovertebral joints: 24 articulations limiting flexion to 4° per level
- Lumbar Lordosis: 40-60° curvature bearing 60% of body weight
- L4-L5 disc: 45% of lumbar herniations
- L5-S1 junction: 75% of spondylolisthesis cases
📌 Remember: CLTS - Cervical Lordosis, Thoracic kyphosis, Lumbar lordosis, Sacral kyphosis. Normal sagittal alignment maintains 7cm plumb line from C7 to posterior S1 corner.
| Spinal Region | Vertebrae Count | Primary Motion | Load Capacity | Common Pathology | Age of Onset |
|---|---|---|---|---|---|
| Cervical | 7 | Rotation (90°) | 12-15 lbs | Spondylosis | 40-50 years |
| Thoracic | 12 | Lateral flexion (25°) | 40-60 lbs | Compression fractures | 60-70 years |
| Lumbar | 5 | Flexion/extension (60°) | 100-150 lbs | Disc herniation | 30-40 years |
| Sacral | 5 (fused) | Minimal | 200+ lbs | Sacroiliitis | 20-30 years |
| Coccygeal | 3-5 (fused) | None | Variable | Coccydynia | Any age |
💡 Master This: The instantaneous axis of rotation (IAR) shifts with spinal pathology. Normal cervical IAR lies within the lower third of vertebral bodies; disc degeneration shifts IAR posteriorly, creating abnormal stress patterns and accelerated facet arthritis.
The intervertebral disc architecture reveals the spine's shock-absorption mastery. Each disc contains 80% water in healthy young adults, decreasing to 70% by age 40 and 60% by age 60. The nucleus pulposus maintains 1.5-2.0 MPa of intradiscal pressure at rest, increasing to 2.3 MPa during sitting and 2.5 MPa during forward flexion.
Connect this foundational architecture through biomechanical stress patterns to understand how normal loading transforms into pathological breakdown.
🏗️ Spine Disorders: The Vertebral Architecture Mastery
⚙️ Biomechanical Stress Patterns: The Loading Dynamics Engine
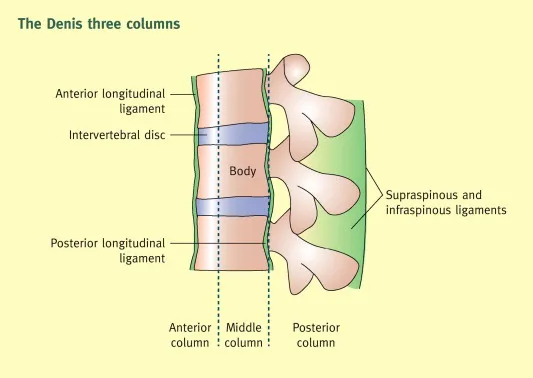
The Three-Column Stability Model
Denis's three-column concept provides the foundation for understanding spinal stability and injury patterns. Stability requires 2 of 3 columns to remain intact; failure of all 3 columns creates unstable injuries requiring surgical intervention.
- Anterior Column: Anterior longitudinal ligament, anterior 2/3 of vertebral body and disc
- Compression failure: Burst fractures with >50% height loss
- Flexion failure: Compression wedge fractures with >20° kyphosis
- Middle Column: Posterior 1/3 of vertebral body, posterior disc, posterior longitudinal ligament
- Critical for stability: 80% of unstable injuries involve middle column
- Retropulsion: >50% canal compromise requires decompression
- Posterior Column: Facet joints, ligamentum flavum, interspinous/supraspinous ligaments
- Distraction failure: >11mm interspinous widening indicates instability
- Rotation failure: >2mm lateral translation on flexion-extension films
📌 Remember: FAM - Flexion (anterior column compression), Axial loading (middle column burst), hyperextension (posterior column distraction). Each mechanism creates predictable column failure patterns.
Disc Pressure Dynamics and Failure Mechanisms
Intradiscal pressure varies dramatically with posture and activity, creating predictable patterns of disc degeneration and herniation. Understanding these pressure gradients explains why 95% of lumbar disc herniations occur at L4-L5 and L5-S1 levels.
| Activity | L3-L4 Pressure (MPa) | Relative Increase | Herniation Risk | Clinical Correlation |
|---|---|---|---|---|
| Supine | 0.1 | Baseline | Minimal | Night pain relief |
| Standing | 0.5 | 5x | Low | Tolerated well |
| Sitting | 0.7 | 7x | Moderate | Office worker syndrome |
| Forward flexion | 1.2 | 12x | High | Lifting injuries |
| Coughing/Valsalva | 1.5 | 15x | Highest | Acute herniation trigger |
💡 Master This: Creep phenomenon explains morning stiffness and increased injury risk. Overnight disc hydration increases height by 1-2cm and stiffness by 300%. First 2 hours after awakening show 5x higher disc injury rates during flexion activities.
The posterior annular fibers contain only outer 1/3 innervation, explaining why central disc herniations remain asymptomatic until neural compression occurs. Lateral herniations affect nerve root at the same level (L4-L5 disc affects L5 root), while far lateral herniations affect the exiting root (L4-L5 disc affects L4 root).
Connect these biomechanical principles through clinical pattern recognition to master diagnostic accuracy in spine disorders.
⚙️ Biomechanical Stress Patterns: The Loading Dynamics Engine
🎯 Clinical Pattern Recognition: The Diagnostic Radar System
The Red Flag Recognition Matrix
Immediate identification of red flag symptoms separates benign mechanical pain from serious pathology requiring urgent intervention. Cauda equina syndrome presents in <2% of back pain cases but requires <6-hour surgical decompression to prevent permanent neurological deficit.
- Neurological Red Flags (Immediate surgical consultation)
- Cauda equina syndrome: Saddle anesthesia + bladder dysfunction + bilateral leg weakness
- Progressive neurological deficit: >3/5 motor weakness or rapid deterioration
- Bowel/bladder dysfunction: Post-void residual >100ml or fecal incontinence
- Infectious Red Flags (Blood cultures + MRI within 24 hours)
- Fever >38.5°C + back pain + elevated ESR >50mm/hr
- IV drug use history + new onset back pain
- Recent spinal procedure + wound drainage or systemic symptoms
- Malignancy Red Flags (MRI + oncology referral within 2 weeks)
- Age >50 with new onset back pain + weight loss >10lbs
- History of cancer + night pain + no relief with rest
- Constant pain unrelieved by position changes
📌 Remember: SCUBA - Saddle anesthesia, Cauda equina, Urinary retention, Bilateral weakness, Anal sphincter dysfunction. Any 2+ features require immediate MRI and surgical consultation.

Radiculopathy vs Myelopathy Discrimination Framework
Distinguishing nerve root compression (radiculopathy) from spinal cord compression (myelopathy) determines treatment urgency and surgical approach. Cervical myelopathy shows >90% progression without surgical intervention.
| Feature | Radiculopathy | Myelopathy | Clinical Significance |
|---|---|---|---|
| Pain pattern | Sharp, shooting, dermatomal | Dull, aching, non-dermatomal | 85% diagnostic accuracy |
| Motor weakness | Single myotome | Multiple levels/bilateral | Localizes compression level |
| Reflexes | Diminished at level | Hyperreflexia below level | Upper vs lower motor neuron |
| Sensory loss | Dermatomal distribution | Glove/stocking or level | Anatomical correlation |
| Gait disturbance | Foot drop (specific nerve) | Broad-based, spastic | Functional impairment |
| Babinski sign | Negative | Positive (90% sensitivity) | Pathognomonic for myelopathy |
| Hoffman sign | Negative | Positive (cervical myelopathy) | Cervical cord compression |
💡 Master This: The inverted radial reflex - tapping the brachioradialis tendon produces finger flexion instead of forearm flexion. This pathognomonic sign indicates C5-C6 myelopathy with >90% specificity and requires urgent surgical evaluation.
Mechanical vs Inflammatory Pain Patterns
Distinguishing mechanical from inflammatory spine pain guides treatment selection and predicts response to conservative management. Mechanical pain responds to NSAIDs + physical therapy in 85% of cases within 6 weeks.
- Mechanical Pain Characteristics
- Morning stiffness <30 minutes, improves with movement
- Worse with activity, better with rest
- Position-dependent: sitting intolerance suggests disc pathology
- Age >40 years with gradual onset
- Inflammatory Pain Characteristics
- Morning stiffness >60 minutes, improves with exercise
- Night pain disrupting sleep, no relief with rest
- Age <40 years with insidious onset >3 months
- Family history of inflammatory arthritis
Connect these recognition patterns through systematic diagnostic approaches to achieve rapid, accurate spine disorder classification.
🎯 Clinical Pattern Recognition: The Diagnostic Radar System
🔬 Systematic Diagnostic Approaches: The Investigation Architecture
The Clinical-Imaging Correlation Matrix
Clinical correlation remains paramount in spine imaging interpretation, as 30-40% of asymptomatic adults show disc abnormalities on MRI, and 20% show significant stenosis without symptoms. Understanding when imaging changes management prevents both over-investigation and missed pathology.
- Immediate Imaging Indications (Within 24 hours)
- Red flag symptoms: Cauda equina, progressive neurological deficit
- Trauma with neurological symptoms or high-energy mechanism
- Suspected infection: Fever + back pain + elevated inflammatory markers
- Known malignancy with new back pain
- Early Imaging Indications (Within 1-2 weeks)
- Radiculopathy with >4/5 motor weakness
- Failed conservative management after 6 weeks
- Surgical candidate evaluation
- Delayed/Unnecessary Imaging
- Acute mechanical back pain without red flags
- Chronic pain without neurological symptoms
- Routine screening in asymptomatic patients
📌 Remember: RAPID imaging indications - Red flags, Age >50 with new pain, Progressive neurological deficit, Infection suspected, Drugs (steroids/immunosuppression). These account for <5% of presentations but >90% of serious pathology.
Advanced Imaging Selection Strategy
Choosing the optimal imaging modality depends on clinical question, anatomical region, and suspected pathology. MRI provides superior soft tissue contrast but costs 3-5x more than CT and requires 45-60 minutes vs 5-10 minutes.
| Imaging Modality | Best Applications | Sensitivity | Specificity | Cost Ratio | Time Required |
|---|---|---|---|---|---|
| X-ray | Alignment, instability, fracture | 60-70% | 85-90% | 1x | 5 minutes |
| CT | Bone detail, acute trauma | 90-95% | 80-85% | 3x | 10 minutes |
| MRI | Soft tissue, neural compression | 95-98% | 90-95% | 5x | 45 minutes |
| CT Myelography | Post-surgical anatomy | 85-90% | 95-98% | 4x | 60 minutes |
| Bone Scan | Infection, metastases | 80-85% | 70-75% | 2x | 3 hours |
💡 Master This: T2-weighted sagittal MRI provides the highest yield for spine pathology screening. Bright CSF signal highlights dark pathology (disc herniation, stenosis, tumor) with >95% sensitivity for clinically significant lesions.
Electrodiagnostic Testing Integration
Nerve conduction studies (NCS) and electromyography (EMG) provide functional assessment of neural pathways, distinguishing anatomical abnormalities from physiologically significant compression. EMG changes appear 2-3 weeks after nerve injury, making early testing falsely negative.
- EMG Indications in Spine Disorders
- Radiculopathy vs peripheral neuropathy differentiation
- Multiple level involvement assessment
- Chronic vs acute nerve injury timing
- Surgical planning for multilevel disease
- EMG Limitations
- Normal study in 15-20% of surgical radiculopathy cases
- Cannot localize exact anatomical level
- Requires 3+ weeks for abnormalities to develop
- Operator-dependent interpretation
Connect these diagnostic approaches through evidence-based treatment algorithms to optimize patient outcomes and resource utilization.
🔬 Systematic Diagnostic Approaches: The Investigation Architecture
⚖️ Evidence-Based Treatment Algorithms: The Therapeutic Decision Engine
Conservative Management Optimization Framework
Conservative treatment achieves equivalent outcomes to surgery for 85% of spine disorders at 6-month follow-up, with significantly lower complication rates (<1% vs 5-15%) and cost savings of $30,000-50,000 per patient.
- First-Line Conservative Management (0-6 weeks)
- NSAIDs: Ibuprofen 600mg TID or naproxen 500mg BID
- Physical therapy: 2-3x weekly for 6-8 weeks
- Activity modification: Avoid bed rest >48 hours
- Patient education: >80% resolve within 6 weeks
- Second-Line Interventions (6-12 weeks)
- Muscle relaxants: Cyclobenzaprine 10mg at bedtime
- Neuropathic agents: Gabapentin 300-900mg TID
- Epidural injections: 70% short-term relief for radiculopathy
- Manipulation therapy: Moderate evidence for acute low back pain
📌 Remember: PRICE-M for acute spine pain - Protect from further injury, Relative rest (not bed rest), Ice 15-20 minutes every 2-3 hours, Compression garments if helpful, Elevation when possible, Movement and early mobilization.

Surgical Intervention Decision Matrix
Surgical intervention shows superior outcomes for specific indications with appropriate patient selection. Lumbar discectomy achieves >90% good-excellent results for radiculopathy with concordant imaging, while fusion surgery shows 60-70% satisfaction rates for degenerative conditions.
| Condition | Conservative Success | Surgical Indication | Success Rate | Complication Rate |
|---|---|---|---|---|
| Disc herniation | 85% at 6 months | Progressive weakness >4/5 | 90-95% | 2-5% |
| Spinal stenosis | 60% at 2 years | Neurogenic claudication | 80-85% | 5-10% |
| Spondylolisthesis | 40% at 1 year | Progressive slip >50% | 75-80% | 10-15% |
| Degenerative disc | 70% at 6 months | Failed conservative + concordant pain | 60-70% | 15-20% |
| Cervical myelopathy | 30% at 6 months | Progressive neurological deficit | 85-90% | 5-15% |
💡 Master This: The 50-50 rule for lumbar fusion - patients with >50% disc height loss and >50% facet joint arthritis show better fusion outcomes than those with preserved anatomy. This explains why younger patients often have worse surgical results.
Minimally Invasive Surgery Evolution
Minimally invasive spine surgery (MISS) techniques reduce tissue trauma by 60-80%, decrease blood loss by 70-90%, and enable same-day discharge for selected procedures. However, learning curves require 50-100 cases for proficiency, and complication rates may be higher during initial experience.
- MISS Advantages
- Reduced muscle damage: <2cm incisions vs 8-12cm open approaches
- Faster recovery: 2-4 weeks vs 6-12 weeks return to work
- Lower infection rates: <1% vs 2-4% for open surgery
- Reduced blood loss: <50ml vs 200-500ml average
- MISS Limitations
- Limited visualization: Higher revision rates in complex cases
- Steep learning curve: Increased complications during initial 50 cases
- Equipment costs: $5,000-15,000 additional per case
- Patient selection: Not suitable for severe deformity or instability
Connect these treatment algorithms through comprehensive rehabilitation strategies to achieve optimal long-term functional outcomes.
⚖️ Evidence-Based Treatment Algorithms: The Therapeutic Decision Engine
🔗 Comprehensive Rehabilitation Integration: The Recovery Architecture
The Biopsychosocial Recovery Model
Chronic spine pain affects >100 million Americans with annual costs exceeding $100 billion, largely due to inadequate integration of psychological and social factors in treatment planning. The biopsychosocial model addresses all dimensions of spine disorders, achieving 30-50% better outcomes than biomedical approaches alone.
- Biological Factors (Tissue healing and structural restoration)
- Acute phase (0-72 hours): Inflammation control and tissue protection
- Subacute phase (3 days-6 weeks): Mobility restoration and strength building
- Chronic phase (>6 weeks): Functional optimization and conditioning
- Psychological Factors (Pain perception and behavioral adaptation)
- Fear-avoidance beliefs: Strongest predictor of chronic disability
- Catastrophizing: Increases pain intensity by 40-60%
- Self-efficacy: Correlates with functional outcomes (r=0.7)
- Social Factors (Environmental support and occupational demands)
- Work satisfaction: >80% return-to-work if high job satisfaction
- Family support: Reduces disability by 25-35%
- Healthcare utilization: Appropriate education reduces visits by 40%
📌 Remember: FABQ (Fear-Avoidance Beliefs Questionnaire) scores >34 predict chronic disability with 85% accuracy. Early identification enables targeted cognitive-behavioral interventions that reduce chronicity risk by 50%.

Progressive Loading and Functional Restoration
Tissue adaptation follows Wolff's Law - structures strengthen in response to progressive loading but weaken with disuse. Optimal loading protocols achieve tissue remodeling without re-injury, following specific progression parameters based on healing timelines and individual capacity.
| Rehabilitation Phase | Duration | Load Progression | Functional Goals | Success Metrics |
|---|---|---|---|---|
| Acute Protection | 0-72 hours | Pain-free ROM | Basic ADLs | Pain <5/10 |
| Early Mobilization | 3-14 days | 50% pain-free load | Walking 30 minutes | ROM >75% normal |
| Strengthening | 2-8 weeks | Progressive resistance | Lifting 20-30 lbs | Strength >80% normal |
| Functional Training | 6-12 weeks | Sport/work specific | Full activity tolerance | Function >90% baseline |
| Maintenance | Ongoing | Periodized loading | Injury prevention | <10% recurrence rate |
💡 Master This: The tissue healing timeline governs progression safety. Collagen synthesis peaks at 3-5 days, tensile strength reaches 50% at 3 weeks, and full remodeling requires 12-16 weeks. Premature loading increases re-injury risk by 300%.
Technology-Enhanced Rehabilitation Strategies
Digital health technologies enhance rehabilitation outcomes through objective monitoring, real-time feedback, and personalized progression algorithms. Wearable sensors provide continuous activity tracking with >95% accuracy, while virtual reality reduces pain perception by 30-40% during exercise sessions.
- Wearable Technology Integration
- Accelerometers: Movement quality assessment and compliance monitoring
- EMG sensors: Muscle activation patterns and fatigue detection
- Heart rate variability: Autonomic function and recovery optimization
- Sleep tracking: Recovery quality affects pain sensitivity by 25%
- Virtual Reality Applications
- Pain distraction: 40% reduction in perceived exertion during exercise
- Movement retraining: Visual feedback improves motor learning by 50%
- Exposure therapy: Gradual return to feared movements
- Gamification: Increases adherence by 60-80% vs traditional exercise
Connect these rehabilitation strategies through long-term maintenance protocols to achieve sustained functional improvement and injury prevention.
🔗 Comprehensive Rehabilitation Integration: The Recovery Architecture
🎯 Clinical Mastery Arsenal: The Spine Expertise Toolkit
The Essential Clinical Commandments
These evidence-based principles guide every spine encounter, preventing common pitfalls that lead to diagnostic errors in 15-20% of cases and treatment failures in 30-40% of patients.
📌 Commandment 1: Red flags rule - Cauda equina, progressive neurological deficit, infection, and malignancy require immediate action. Missing these creates medicolegal liability and permanent disability.
📌 Commandment 2: Imaging correlation - 30-40% of asymptomatic adults show disc abnormalities. Treat the patient, not the MRI findings. Clinical symptoms must correlate with imaging findings.
📌 Commandment 3: Conservative first - 85% of spine disorders resolve with appropriate conservative management. Surgery should be last resort except for specific indications with clear benefit.
📌 Commandment 4: Function over pain - Functional improvement predicts long-term success better than pain reduction. Focus on activity tolerance and quality of life.
📌 Commandment 5: Biopsychosocial approach - Psychological factors predict outcomes better than anatomical findings. Address fear-avoidance, catastrophizing, and social support.
Rapid Assessment Protocol Matrix
Time-efficient evaluation protocols enable comprehensive assessment within 10-15 minutes while maintaining >95% diagnostic accuracy for common spine presentations.
| Assessment Component | Time Allocation | Key Elements | Diagnostic Yield |
|---|---|---|---|
| History | 5 minutes | Red flags, pain pattern, functional impact | 80% diagnostic accuracy |
| Physical Exam | 5 minutes | Neurological screen, provocative tests | 15% additional yield |
| Decision Making | 3 minutes | Imaging needs, treatment plan | 5% refinement |
| Patient Education | 2 minutes | Prognosis, expectations, next steps | Outcome optimization |
💡 Master This: Waddell signs identify non-organic pain behaviors but should never be used to dismiss patients. >3 positive signs suggest psychological distress requiring biopsychosocial intervention, not malingering.
Evidence-Based Outcome Predictors
Prognostic factors enable accurate outcome prediction and appropriate treatment selection, optimizing resource allocation and patient expectations.
- Positive Prognostic Factors (>80% good outcomes)
- Age <40 years with acute onset <6 weeks
- High self-efficacy and positive coping strategies
- Good job satisfaction and supportive work environment
- Absence of fear-avoidance behaviors
- Normal psychological screening scores
- Negative Prognostic Factors (<50% good outcomes)
- Chronic pain >6 months with multiple failed treatments
- High catastrophizing scores (>30 on PCS)
- Pending litigation or disability claims
- Comorbid depression or anxiety disorders
- Poor social support and job dissatisfaction
⭐ Clinical Pearl: The STarT Back Tool stratifies patients into low, medium, and high-risk groups with >85% accuracy. Matched treatment based on risk stratification improves outcomes by 30-40% compared to standard care.
💡 Master This: Yellow flags (psychological risk factors) predict chronicity better than red flags (serious pathology) or imaging findings. Early identification and targeted intervention reduce chronic disability by 50%.
Connect this clinical mastery toolkit through continuous learning and outcome monitoring to achieve sustained excellence in spine disorder management while advancing the field through evidence-based practice.
🎯 Clinical Mastery Arsenal: The Spine Expertise Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












