Pre-Prosthetic Management - Stump Smart Start
- Patient Assessment (Holistic):
- Medical status (comorbidities like DM, PVD).
- Functional goals (ADLs, mobility).
- Psychological readiness (coping, body image).
- Vocational needs (return to work).
- Stump Assessment (Thorough):
- Length & Shape: Aim for conical/cylindrical.
- Skin: Integrity, scars, infection signs, sensation (neuroma).
- Joints: Range of Motion (ROM), Muscle Power (MMT).
- Stump Care & Conditioning (Key to Success):
- Edema Control: Figure-of-eight elastic bandaging, shrinker socks.
- Shaping: Achieve mature stump for prosthetic interface.
- Desensitization: Tapping, massage, texture exposure.
- Hygiene: Daily cleaning and skin inspection.
- Exercises: Strengthening (proximal muscles), ROM.
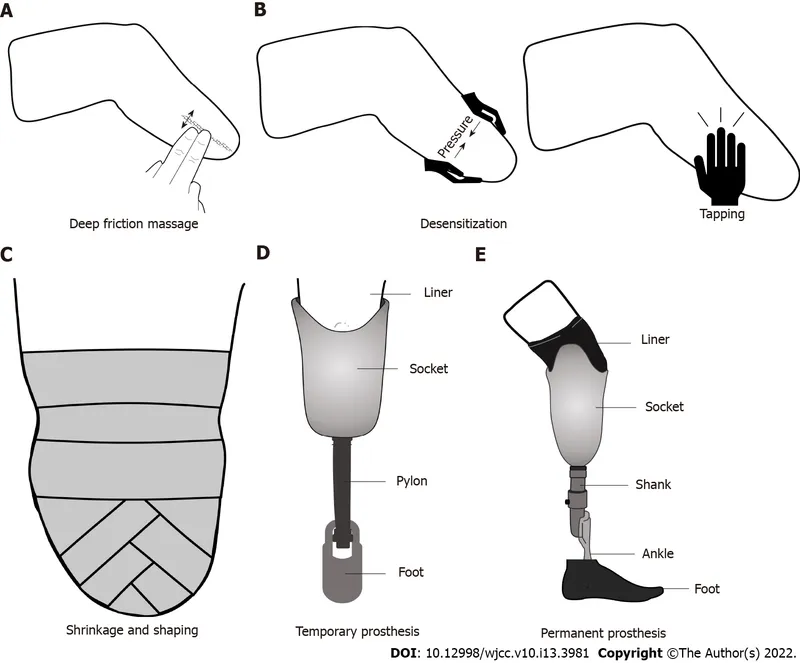
⭐ Stump volume fluctuation is greatest in the initial 3-6 months post-op; consistent compression is vital for optimal prosthetic fitting and to prevent stump edema related complications such as pain and skin breakdown.
Prosthetic Components & Prescription - Limb Lego Logic
- Principles: Maximize function, comfort, cosmesis; match patient's activity level & goals.
- Core Components:
- Socket: Critical interface with residual limb. Key types:
- Transtibial: Patellar Tendon Bearing (PTB), Total Surface Bearing (TSB).
- Transfemoral: Quadrilateral, Ischial Containment.
- Suspension: Secures prosthesis (e.g., suction, pin/lock, vacuum, straps).
- Joints: Knee units (single-axis, polycentric, microprocessor-controlled), Ankle-foot assemblies (e.g., SACH, dynamic response/energy-storing feet).
- Terminal Device (UL): Hooks (functional, durable), Hands (cosmetic, functional - e.g., myoelectric).
- Socket: Critical interface with residual limb. Key types:
- Prosthesis Types (Examples):
- Upper Limb: Body-powered (harness & cable), Myoelectric (EMG signals).
- Materials: Lightweight, strong, durable: Carbon fiber, titanium, aluminum alloys, thermoplastics.
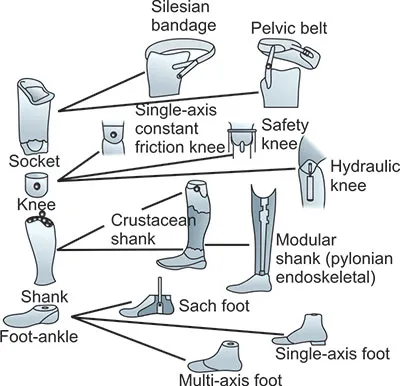
⭐ The SACH (Solid Ankle Cushion Heel) foot is a basic, non-articulated, durable, and widely prescribed prosthetic foot, especially suitable for initial fittings and lower activity users due to its simplicity and stability during early stance phase of gait.
Prosthetic Fitting & Alignment - Socket Fit Feats
- Socket Casting & Fabrication:
- Transtibial (TT): Patellar Tendon Bearing (PTB) socket.
- Key landmarks: patellar tendon, medial tibial flare.
- Pressure tolerant: patellar tendon, medial/lateral flares.
- Pressure sensitive: fibular head, tibial crest, distal tibia.
- Transfemoral (TF): Ischial Containment (IC) socket. Encloses ischial tuberosity & pubic ramus for stability.
- Transtibial (TT): Patellar Tendon Bearing (PTB) socket.
- Alignment Principles:
- Static (Bench): Initial setup. LL: Plumb line from greater trochanter to mid-heel.
- Dynamic: Gait observation. Adjust for comfort, function, energy efficiency.
- Prosthetic Checkout:
- Sequence: Bench → Static (standing) → Dynamic (walking).
- Criteria: Comfort, stability, no pistoning, good skin integrity post-use.
- Common Fit Issues & Adjustments:
- Pressure areas (modify socket), pistoning (improve suspension), bell-clapping (add distal padding), rotation (check alignment/suspension).
⭐ For PTB sockets, approximately 60% of weight is borne by the patellar tendon bar, with additional support from tibial flares.

Prosthetic Training & Rehabilitation - Gait & Grip Glory
-
Goals: Maximize functional independence, safety, QoL with prosthesis.
-
Lower Limb (LL) Training:
- Donning/doffing independently.
- Balance, weight transfer, proprioception.
- Gait phases: Parallel bars → walker/crutches → cane → independent ambulation.
- Obstacles: Stairs (step-to/step-over), ramps, uneven surfaces.
-
Common LL Gait Deviations & Corrections:
Deviation Cause(s) Correction(s) Abducted Gait Prosthesis long; hip contracture Length; stretch; training Vaulting Prosthesis long; ↓ knee flex Length; ↑ knee motion; training Circumduction Prosthesis long; ↓ knee flex; fear Length; ↑ knee flex; confidence -
Upper Limb (UL) Training:
- Donning/doffing.
- Controls: Body-powered (harness), Myoelectric (EMG).
- Functional use: ADLs, vocational tasks.
-
Patient Education:
- Wear schedule: Gradual increase to prevent skin issues.
- Skin care: Daily inspection, hygiene, sock management.
- Prosthesis care & maintenance.
⭐ Phantom limb sensation (non-painful) is common; phantom pain needs active management.
High‑Yield Points - ⚡ Biggest Takeaways
- Pre-prosthetic care focuses on stump maturation, muscle strengthening, and contracture prevention.
- Socket design (e.g., Patellar Tendon Bearing (PTB), Ischial Containment) is critical for optimal fit and function.
- Correct static and dynamic alignment is crucial for an efficient gait pattern and stability.
- Gait training progresses through balance, weight transfer, and ambulation practice with the prosthesis.
- Differentiate phantom limb pain (neuropathic origin) from residual limb pain (often mechanical or ischemic).
- Signs of poor prosthetic fit include pistoning (vertical movement) or socket rotation.
- Successful prosthetic rehabilitation requires a coordinated multidisciplinary team approach including the patient an prosthetist
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

