Fundamentals - Prosthetic Power Play
- Core Principles:
- Efficient load transfer: Stump → prosthesis → ground.
- Dynamic stability: Balance during stance & swing phases.
- ↓ Metabolic energy expenditure.
- Socket comfort & skin integrity: Avoid pressure sores.
- Prosthetic Alignment Goals:
- Restore near-normal gait biomechanics.
- Optimize joint moments for stability & control (e.g., knee extension moment).
- Achieve even pressure distribution within the socket.
- Key Biomechanical Terms:
- Ground Reaction Force (GRF): Force exerted by the ground on the prosthesis.
- Center of Pressure (CoP): Point of application of GRF on the prosthetic foot.
- Weight line (Load line): Vertical line through center of mass.
- Concepts:
- Levers & Moments: Prosthesis segments act as levers. Moment $M = F \times d$ (Force x perpendicular distance).
- Pressure: $P = F/A$ (Force / Area); critical for socket design.
⭐ The alignment of the Ground Reaction Force (GRF) vector relative to the prosthetic joint centers (e.g., knee, hip) is crucial for determining joint stability and the muscular effort required during gait.
oka
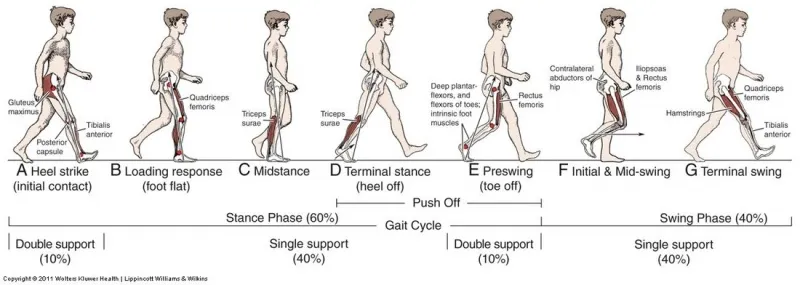
Gait & Deviations - Stepping Right, Not Wrong
Normal gait cycle: 60% stance phase, 40% swing phase. Deviations signal underlying problems, often prosthetic or anatomical.
- Common Transfemoral (AK) Deviations & Prosthetic Causes:
- Circumduction: Prosthesis too long; high knee friction; poor suspension; abduction contracture.
- Vaulting (on sound limb): Prosthesis too long; poor suspension; insufficient prosthetic knee flexion.
- Lateral Trunk Bending (to prosthetic side): Prosthesis too short; weak hip abductors (gluteus medius); pain; hip abduction contracture.
- Medial/Lateral Whip: Malrotated knee axis/bolt.
- Terminal Impact (knee hyperextension): Insufficient knee extension dampening; forceful hip extension.
- Uneven Step Length: Fear/insecurity; poor balance; hip flexion contracture.
- Common Transtibial (BK) Deviations & Prosthetic Causes:
- Excessive Knee Flexion (early stance): Socket too anterior; heel cushion too stiff/high; excessive prosthetic foot dorsiflexion.
- Insufficient Knee Flexion / Knee Hyperextension (mid-stance): Socket too posterior; heel cushion too soft/low; excessive prosthetic foot plantarflexion.
- Foot Slap (audible slap at heel strike): Heel cushion too soft; inadequate plantarflexion resistance.
- Drop Off (early heel rise/knee flexion at late stance): Keel too short; socket too anterior; excessive dorsiflexion.
- Pistoning (vertical motion of stump in socket): Inadequate suspension.
⭐ Circumduction in transfemoral amputees is frequently caused by a prosthesis that is too long, has excessive knee friction, or due to an abduction contracture of the hip.
Socket & Stump - The Perfect Fit
- Goal: Intimate stump-socket contact for optimal load transfer, stability, comfort.
- Transtibial Sockets:
- Patellar Tendon Bearing (PTB): Concentrates load on patellar tendon, flares.
- Total Surface Bearing (TSB): Even pressure distribution; often preferred.
- Transfemoral Sockets:
- Quadrilateral: Ischial weight-bearing on posterior brim.
- Ischial Containment: Encases ischium & ramus; enhances stability, control.
- Interface Dynamics:
- Liners (gel, silicone): Cushion, reduce shear, aid suspension.
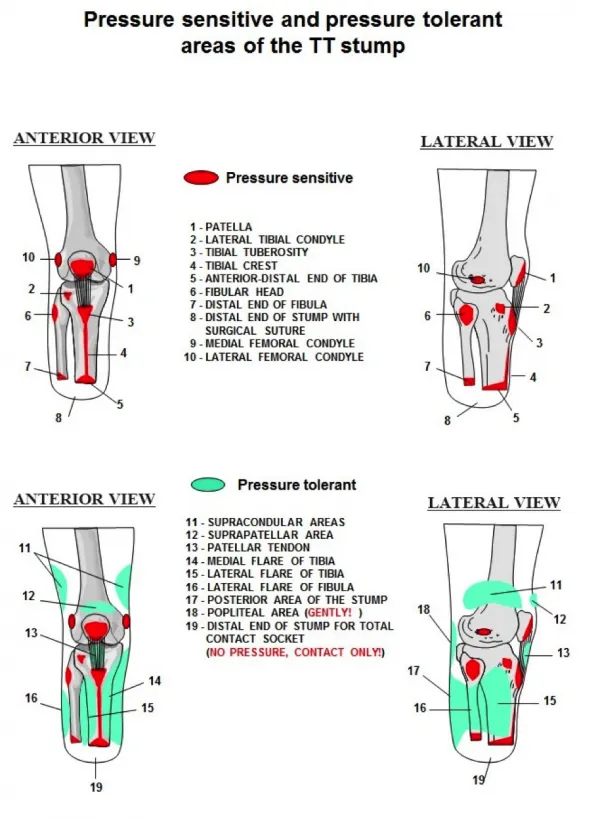
- Pressure Management: Load tolerant areas (patellar tendon, flares); relieve sensitive areas (fibular head, tibial crest).
- Minimize pistoning (stump movement in socket).
⭐ Improper socket fit is the most common cause of prosthetic discomfort and skin breakdown.
Alignment & Balance - Standing Tall, Walking Strong
- Prosthetic Alignment: Optimizes interaction between prosthesis & body.
- Goals: Stability (stance), controlled mobility (swing), comfort, energy conservation, cosmesis.
- Types:
- Static (Bench) Alignment: Initial setup using anatomical landmarks.
- Dynamic Alignment: Fine-tuning based on gait analysis.
- Key Reference:
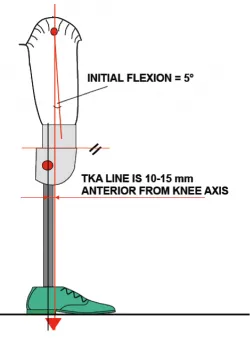
- TKA Line (Trochanter-Knee-Ankle): Ideal weight-bearing line.
- Transtibial (TT): Passes through knee center & prosthetic foot's ankle bolt.
- Transfemoral (TF): Passes anterior to knee joint axis, posterior to hip.
- TKA Line (Trochanter-Knee-Ankle): Ideal weight-bearing line.
- Balance: Essential for safe ambulation; achieved via optimal alignment & socket fit.
⭐ Correct prosthetic alignment is paramount to reduce gait deviations and minimize oxygen consumption (energy expenditure) during ambulation by up to 20% compared to malaligned prostheses.
High‑Yield Points - ⚡ Biggest Takeaways
- Socket design dictates load transmission, comfort, and suspension.
- Prosthetic alignment (static & dynamic) is crucial for efficient gait and reduced energy cost.
- Ground Reaction Force (GRF) manipulation is vital for prosthetic stability and control.
- Lever arm mechanics influence joint moments and overall prosthetic function.
- Energy Storing and Returning (ESAR) feet improve gait dynamics and shock absorption.
- Identify pressure-tolerant areas (e.g., patellar tendon, medial tibial flare) for optimal weight bearing.
- Avoid pressure-sensitive areas (e.g., fibular head, tibial crest) to prevent skin breakdown and pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

