Intro to Mobility Aids - First Steps
- Assistive Devices for Mobility (ADMs): External devices enhancing movement for individuals with mobility impairments.
- Primary Goals: 📌 S.A.F.E.R.
- Stability & balance improvement
- Assist ambulation, promote independence
- Functional ability ↑ (e.g., ADLs)
- Energy conservation during movement
- Reduce weight-bearing on limbs, alleviate pain
- Broad Classification:
- By Support: Canes, crutches, walkers
- By Mobility: Wheeled (e.g., wheelchairs) vs. Non-wheeled
- Prescription Principles: Patient assessment (strength, balance, cognition, environment, goals).

⭐ Proper patient education and training are crucial for safe and effective ADM use.
Canes & Crutches - Lean On Me
-
Canes: Mild balance/stability, unilateral weakness.
-
Types: Single-point, quad cane, hemi-walker.
-
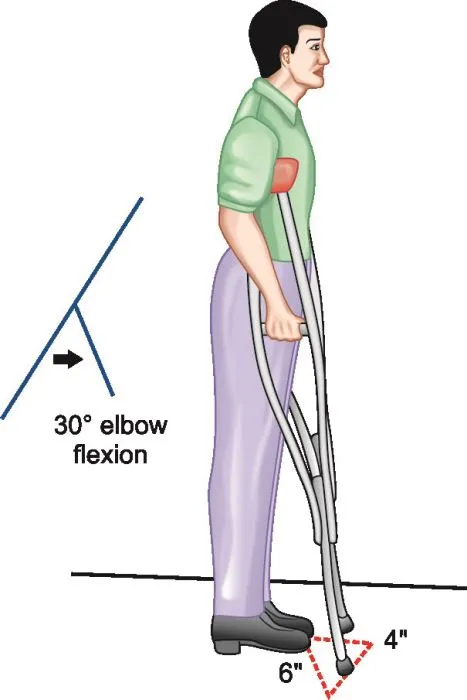
Height: Greater trochanter/ulnar styloid, 20-30° elbow flexion.
-
Usage: Use contralateral (📌 COAL: Cane Opposite Affected Leg).
-
-
Crutches: ↓ Weight-bearing, ↑ stability.
- Types: Axillary, Forearm (Lofstrand/Canadian).
- Axillary:
- Fit: 2-3 fingers below axilla; handpiece for 20-30° elbow flexion.

- ⚠️ Complication: Crutch palsy (Radial nerve).
- Fit: 2-3 fingers below axilla; handpiece for 20-30° elbow flexion.
- Forearm: Cuff: proximal 1/3 forearm, 1-1.5 in. below elbow.
- Stairs: 📌 "Up with the Good, Down with the Bad".
⭐ Radial nerve palsy: most common neuro complication from ill-fitted axillary crutches.
-
Crutch Gaits:
-
2-point: Mild bilateral weakness.
-
3-point: NWB one limb.
-
4-point: Severe bilateral weakness/incoordination (stable).
-
Swing-to/Swing-through: Bilateral LL weakness (paraplegia), needs good upper body strength.
-
-
Gait Selection Flowchart:
Walkers & Frames - Steady Go
- Types & Indications:
- Standard (Pick-up): Max stability; for severe balance/weakness.
- Wheeled (2-wheel front): Balance support, less energy than standard.
- Rollator (4-wheel): Balance, ↑gait speed; not for significant weight-bearing. Has brakes, seat, basket.
- Hemi-walker: For hemiplegia, more stable than quad cane.
- Height: Handgrip at greater trochanter/ulnar styloid; 20-30° elbow flexion.
- Gait: Walker → Affected leg → Unaffected leg (WWAL).
- Pros: Wide base, high stability.
- Cons: Slow, bulky, stairs/uneven terrain difficult.

⭐ Standard walkers provide the most stability but require more energy expenditure than wheeled walkers.
Wheelchairs & Orthoses - Mobile Support
- Wheelchairs: Aid non-ambulatory patients, conserve energy, enable long-distance mobility, provide pressure relief.
- Types:
- Manual: Self-propelled or attendant-propelled.
- Powered (Electric): For users unable to self-propel or for long distances.
- Prescription: Correct fit (seat width/depth/height, back height, armrests, footrests) prevents pressure sores, postural issues.
- Specialized: Sports, standing, reclining.
- Types:
- Lower Limb Orthoses: Goal: Stabilize joints, assist movement, prevent deformity, protect, reduce pain.
- AFO (Ankle-Foot Orthosis):
- Indications: Foot drop, ankle instability, mediolateral control.
- Types: Solid, Hinged, Posterior Leaf Spring (PLS), Ground Reaction.
⭐ A Posterior Leaf Spring (PLS) AFO is for isolated foot drop with good mediolateral ankle stability, aiding dorsiflexion in swing phase.
- KAFO (Knee-Ankle-Foot Orthosis):
- Indications: Significant knee weakness/instability (e.g., quadriceps paralysis post-polio, SCI, muscular dystrophy).
- AFO (Ankle-Foot Orthosis):
High‑Yield Points - ⚡ Biggest Takeaways
- Axillary crutches: Risk of radial nerve palsy; fit 2-3 fingerbreadths below axilla, elbow 20-30° flexion.
- Canes: Held contralateral to affected limb; handle at greater trochanter height.
- Walkers: Offer maximum stability among ambulatory aids; standard type requires lifting.
- Three-point gait: For non-weight bearing on one leg, used with crutches or a walker.
- AFO (Ankle-Foot Orthosis): Primary orthotic intervention for foot drop.
- PTB (Patellar Tendon Bearing) socket: Standard design for Below-Knee Amputation (BKA) prostheses.
- Energy expenditure: Significantly ↑ with more proximal amputation levels and greater device support (Walker > Crutches > Cane).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

