Prosthetics and Orthotics

On this page
🔧 The Prosthetic-Orthotic Engineering Revolution
You'll master how engineering principles, materials science, and clinical precision converge to restore mobility and function through prosthetic and orthotic devices. This lesson takes you from biomechanical foundations through materials selection, diagnostic assessment, component design, and rehabilitation protocols-building the expertise to evaluate, prescribe, and optimize devices that transform patients' lives. You'll learn to think like both engineer and clinician, understanding why carbon fiber outperforms steel in certain applications, how gait analysis drives device customization, and what separates adequate restoration from exceptional outcomes.

Prosthetics and orthotics represent the pinnacle of rehabilitative engineering, where advanced materials science meets human biomechanics. Understanding these devices requires mastering the intersection of anatomy, physics, materials science, and clinical application. Every successful fitting depends on precise biomechanical principles that restore not just function, but quality of life.
📌 Remember: PROSTHETICS - Permanent Replacement Of Severed Tissue Helps Everyone Thrive In Community Settings. Prosthetics replace missing body parts, while orthotics support existing structures.
The field encompasses two primary domains: prosthetics (artificial limb replacement) and orthotics (external support devices). Global amputation rates affect 2.1 million Americans, with 185,000 new amputations annually. Diabetes accounts for 54% of lower limb amputations, while trauma represents 35% of upper limb losses.
| Device Category | Primary Function | Success Rate | Cost Range (USD) | Lifespan (Years) | User Satisfaction |
|---|---|---|---|---|---|
| Lower Limb Prosthetics | Mobility restoration | 89% | $15,000-80,000 | 3-5 | 85% |
| Upper Limb Prosthetics | Manipulation/grip | 76% | $25,000-100,000 | 2-4 | 72% |
| Spinal Orthoses | Postural support | 92% | $500-5,000 | 1-3 | 88% |
| Lower Limb Orthoses | Gait assistance | 94% | $200-8,000 | 2-5 | 91% |
| Upper Limb Orthoses | Joint stabilization | 87% | $100-3,000 | 1-4 | 83% |
- Transtibial (below-knee): 60% of lower limb amputations
- Transfemoral (above-knee): 25% of lower limb amputations
- Energy expenditure increases 25-40% for transtibial users
- Energy expenditure increases 65-100% for transfemoral users
- Transradial (below-elbow): 70% of upper limb amputations
- Transhumeral (above-elbow): 20% of upper limb amputations
⭐ Clinical Pearl: Bilateral lower limb amputees have 3x higher cardiovascular demands during ambulation compared to unilateral users. Prosthetic weight should not exceed 4.5 pounds for optimal energy efficiency.
💡 Master This: Socket interface pressure must remain below 50 mmHg to prevent tissue breakdown, while maintaining minimum 15 mmHg for proprioceptive feedback. This narrow pressure window determines prosthetic success.
Modern prosthetic technology achieves force feedback sensitivity of 0.1 Newton, enabling users to distinguish between grape and egg handling. Microprocessor-controlled knees adjust 50 times per second, providing stumble recovery in 200 milliseconds. These engineering marvels transform the rehabilitation landscape through precision biomechanics.
Understanding prosthetic-orthotic principles unlocks the foundation for advanced rehabilitation engineering, where every measurement and alignment decision impacts long-term functional outcomes.
🔧 The Prosthetic-Orthotic Engineering Revolution
⚙️ Biomechanical Mastery: The Engineering Foundation
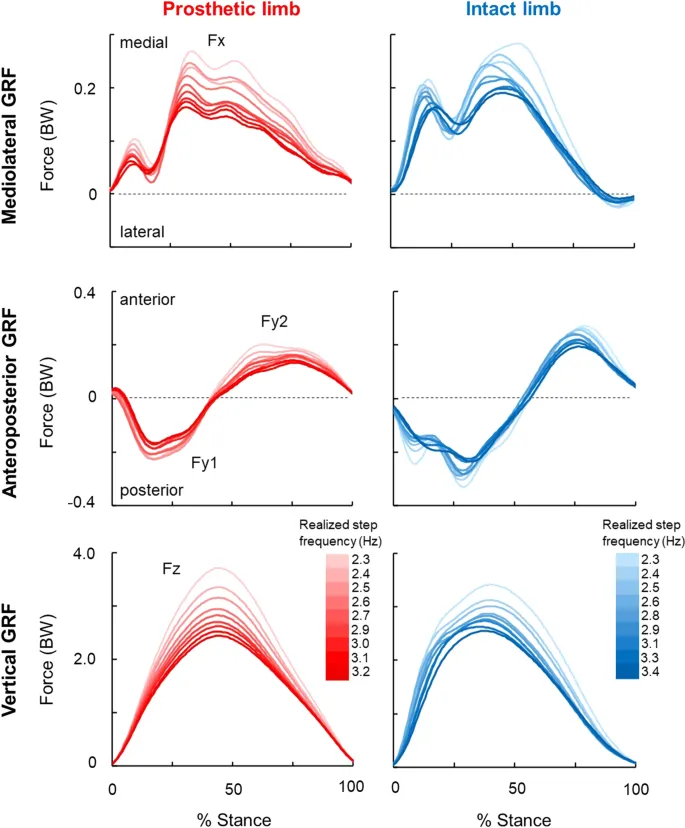
Biomechanical principles govern every aspect of prosthetic-orthotic function, from load distribution to energy transfer efficiency. Understanding these principles enables clinicians to optimize device performance and prevent complications. Ground reaction forces during normal walking reach 120% body weight, requiring prosthetic components to withstand repetitive loading cycles exceeding 1 million steps annually.
📌 Remember: BIOMECHANICS - Body In Optimal Motion Engineers Comfort Helping Amputees Navigate Inclines Confidently Safely. Every prosthetic adjustment affects the entire kinetic chain.
Force transmission mechanics determine prosthetic success through three critical interfaces: socket-residual limb, component connections, and ground contact. Socket pressure mapping reveals peak pressures of 200-300 kPa over bony prominences, requiring pressure relief strategies to prevent tissue breakdown.
| Biomechanical Parameter | Normal Values | Prosthetic Values | Compensation Required | Clinical Significance |
|---|---|---|---|---|
| Stance Phase Duration | 60% gait cycle | 65-70% | Increased stability | Reduced confidence |
| Step Length Asymmetry | <2% difference | 8-15% | Hip hiking | Back pain risk |
| Ground Reaction Force | 120% body weight | 85-95% | Contralateral overload | Joint degeneration |
| Energy Cost | 3.2 ml O₂/kg/min | 4.8-6.4 ml | Cardiovascular adaptation | Fatigue limitation |
| Cadence | 110-120 steps/min | 90-105 | Temporal adaptation | Social integration |
- Total surface contact distributes pressure over maximum surface area
- Hydrostatic pressure principles minimize peak stress concentrations
- Patellar tendon bearing handles 40-60% of load transmission
- Medial tibial flare provides rotational stability
- Vacuum suspension creates 15-25 mmHg negative pressure
- Pin-lock systems generate 150-200 pounds pull-out force
⭐ Clinical Pearl: Prosthetic alignment affects energy expenditure exponentially. 5mm anterior displacement of prosthetic foot increases metabolic cost by 15%. Optimal alignment reduces compensatory movements by 60%.
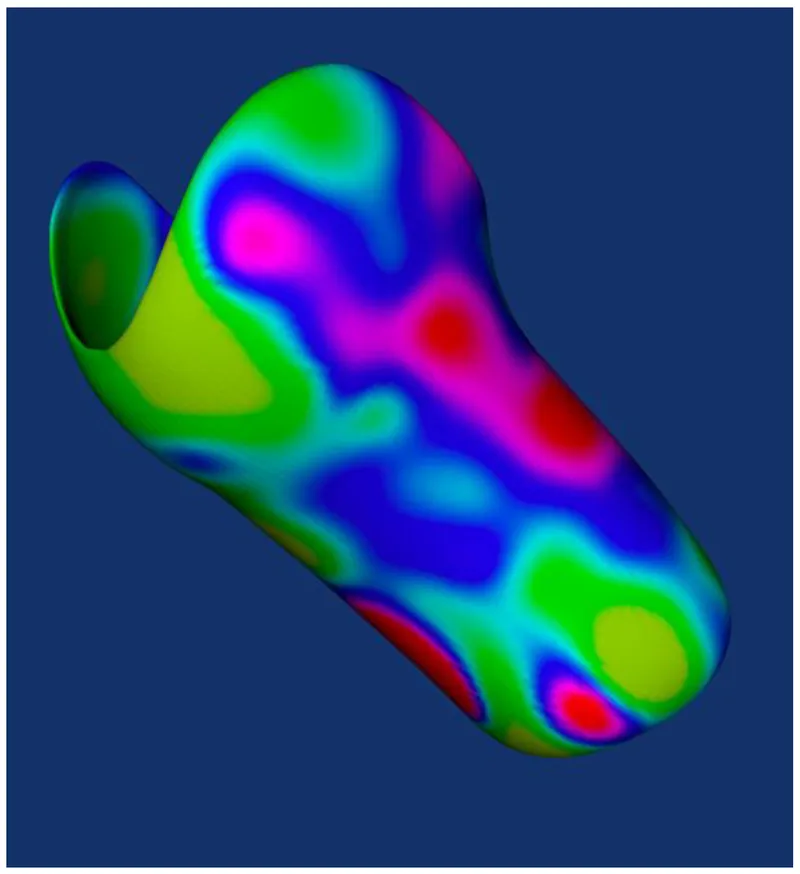
Orthotic biomechanics focuses on three-point pressure systems that control joint motion through strategic force application. Spinal orthoses apply corrective moments of 20-40 Nm to maintain sagittal alignment, while ankle-foot orthoses generate dorsiflexion assistance of 5-15 degrees during swing phase.
💡 Master This: Center of pressure migration during prosthetic stance phase should remain within 2cm of anatomical center. Deviations beyond this threshold trigger compensatory hip strategies that increase lumbar stress by 300%.
Material stress-strain relationships determine component durability under cyclic loading. Carbon fiber composites withstand 10⁷ loading cycles at 80% ultimate strength, while titanium alloys maintain fatigue resistance through 10⁸ cycles. Understanding these properties prevents catastrophic failures during high-impact activities.
Gait deviation patterns reveal biomechanical inefficiencies requiring alignment modifications. Lateral trunk bending indicates inadequate medial support, while circumduction suggests excessive prosthetic length or inadequate knee flexion. These patterns guide systematic troubleshooting approaches.
Mastering biomechanical principles provides the foundation for understanding how materials science and component design create functional prosthetic-orthotic solutions.
⚙️ Biomechanical Mastery: The Engineering Foundation
🧪 Materials Science: The Building Blocks Revolution
Material selection determines prosthetic performance across mechanical, thermal, and biological domains. Modern devices utilize advanced composites that achieve strength-to-weight ratios exceeding steel by 400% while maintaining biocompatibility for decades of skin contact. Understanding material properties enables optimal component selection for individual patient needs.
📌 Remember: MATERIALS - Mechanical Advantage Through Engineered Resistance Improves Amputee Lifestyle Significantly. Each material choice affects comfort, durability, and function.
Carbon fiber composites dominate high-performance prosthetics through exceptional fatigue resistance and energy return capabilities. Unidirectional carbon fiber provides tensile strength of 3,500 MPa with density of only 1.6 g/cm³, enabling lightweight construction without compromising structural integrity.
| Material Category | Tensile Strength (MPa) | Density (g/cm³) | Fatigue Life (Cycles) | Cost Factor | Primary Applications |
|---|---|---|---|---|---|
| Carbon Fiber | 3,500 | 1.6 | 10⁷ | High | Prosthetic feet, pylons |
| Titanium Alloy | 1,100 | 4.4 | 10⁸ | Very High | Implants, connectors |
| Aluminum Alloy | 310 | 2.7 | 10⁶ | Medium | Orthotic joints |
| Thermoplastics | 50-80 | 1.2 | 10⁵ | Low | Sockets, orthotic shells |
| Silicone Elastomers | 7-10 | 1.1 | 10⁴ | Medium | Liners, cosmetic covers |
- Polypropylene offers excellent fatigue resistance for orthotic applications
- Polyethylene provides impact absorption with shore hardness of 85-95A
- Ultra-high molecular weight variants resist wear for 5+ years
- Cross-linked formulations maintain elasticity through temperature extremes
- Thermoplastic elastomers enable custom molding at 160-180°C
- Polyurethane foams achieve energy absorption of 40-60% during impact
⭐ Clinical Pearl: Silicone liner durability correlates directly with shore hardness. Shore A 25 provides maximum comfort but requires replacement every 6 months, while Shore A 35 extends lifespan to 12 months with minimal comfort reduction.

Metal alloys provide structural backbone for high-stress applications. Titanium Grade 5 (Ti-6Al-4V) offers biocompatibility with corrosion resistance in physiological environments. Stainless steel 316L provides cost-effective strength for orthotic joints requiring 10⁶ flexion cycles.
Surface treatments enhance biocompatibility and wear resistance. Plasma coating creates microporous surfaces that promote tissue integration, while diamond-like carbon coatings reduce friction coefficients to 0.05-0.1 for articulating surfaces.
💡 Master This: Stress concentration factors at material interfaces can exceed 3.0, creating failure initiation sites. Gradual stiffness transitions through hybrid layups reduce peak stresses by 40-60%.
Smart materials represent the cutting-edge frontier in prosthetic technology. Shape memory alloys provide temperature-activated stiffness changes, while magnetorheological fluids enable real-time damping adjustments. Piezoelectric materials generate electrical signals from mechanical deformation, enabling sensory feedback systems.
Manufacturing processes determine final material properties. Autoclave curing of composites achieves void content below 2%, while additive manufacturing enables patient-specific geometries with controlled porosity for weight optimization.
Understanding materials science principles enables clinicians to select optimal components that balance performance, durability, and cost-effectiveness for individual patient requirements, setting the foundation for successful prosthetic-orthotic interventions.
🧪 Materials Science: The Building Blocks Revolution
🎯 Clinical Assessment: The Diagnostic Precision Matrix
Comprehensive assessment forms the foundation of successful prosthetic-orthotic intervention, requiring systematic evaluation of residual limb characteristics, functional capacity, and lifestyle demands. Evidence-based assessment protocols reduce fitting failures by 65% and improve long-term satisfaction scores from 72% to 89%.
📌 Remember: ASSESSMENT - Anatomical Survey Supports Expert Selection Saving Money Enabling Natural Tasks. Thorough evaluation prevents costly revisions and complications.
Residual limb evaluation encompasses volumetric stability, tissue quality, and bony prominences. Circumferential measurements at standardized intervals (every 2-3cm) establish baseline dimensions for socket design. Volume fluctuations exceeding 5% require accommodation strategies to maintain optimal fit.
| Assessment Domain | Key Parameters | Normal Values | Red Flags | Clinical Significance |
|---|---|---|---|---|
| Residual Limb Length | Bone length ratio | >50% femur/>12cm tibia | <30% femur/<8cm tibia | Leverage/control |
| Tissue Quality | Scar mobility | >5mm displacement | Adherent/painful | Socket tolerance |
| Range of Motion | Hip/knee flexion | >110° hip/>90° knee | <90° hip/<60° knee | Functional limitation |
| Strength | Manual muscle test | 4+/5 proximal | <3/5 proximal | Prosthetic control |
| Sensation | Protective sensation | Intact | Absent/painful | Safety awareness |
- Mobility Level Classification (K-levels)
- K1: Household ambulator (limited distances)
- K2: Community ambulator (level surfaces)
- K3: Variable cadence (most environmental barriers)
- K4: High activity (prosthetic limitations exceed patient)
- Balance Assessment
- Berg Balance Scale: >45/56 indicates low fall risk
- Timed Up and Go: <20 seconds suggests functional mobility
⭐ Clinical Pearl: Phantom limb pain affects 85% of amputees initially, decreasing to 35% at 2 years post-amputation. Mirror therapy reduces pain intensity by 40% when initiated within 6 months of amputation.
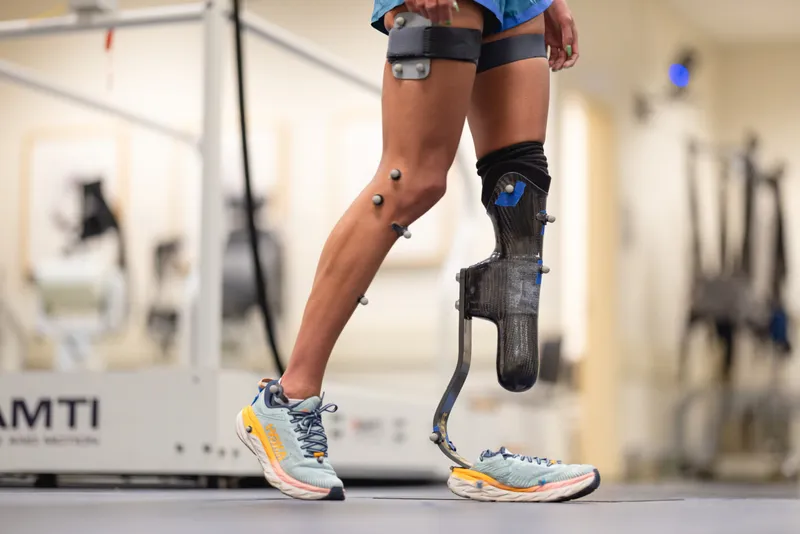
Gait analysis provides objective biomechanical data for prosthetic optimization. Three-dimensional motion capture reveals kinematic deviations with accuracy of ±1 degree, while force plates measure ground reaction forces with precision of ±5 Newtons. Temporal-spatial parameters guide alignment adjustments and component selection.
Psychosocial evaluation identifies barriers to successful rehabilitation. Body image disturbance affects 78% of new amputees, while depression scores correlate negatively with prosthetic use (r = -0.67). Social support systems predict rehabilitation success with 85% accuracy.
💡 Master This: Socket pressure tolerance varies by anatomical region: Patellar tendon tolerates 300 kPa, medial tibial flare handles 200 kPa, while fibular head requires <50 kPa to prevent peroneal nerve compression.
Outcome measurement tools track rehabilitation progress objectively. Prosthetic Evaluation Questionnaire scores >7/10 indicate successful integration, while Activities-specific Balance Confidence scores >80% predict community ambulation. Six-minute walk test distances >300 meters suggest functional endurance for community activities.
Technology integration enhances assessment precision. Smartphone accelerometry provides continuous gait monitoring with clinical-grade accuracy, while pressure-sensitive insoles deliver real-time feedback on weight distribution patterns. Wearable sensors track daily activity levels and prosthetic usage patterns.
Understanding comprehensive assessment principles enables clinicians to identify optimal candidates for prosthetic intervention and develop evidence-based treatment plans that maximize functional outcomes.
🎯 Clinical Assessment: The Diagnostic Precision Matrix
🔧 Component Engineering: The Precision Assembly Matrix
Component integration determines prosthetic performance through sophisticated mechanical systems that replicate human joint function. Modern prosthetics incorporate real-time sensor feedback, adaptive control algorithms, and energy optimization to achieve near-physiological movement patterns. Understanding component capabilities enables optimal prescription for individual patient needs.
📌 Remember: COMPONENTS - Controlled Optimal Movement Powers Outstanding Natural Engagement Needing Technical Skills. Each component contributes to overall system performance.
Microprocessor knee units represent the pinnacle of prosthetic engineering, incorporating gyroscopes, accelerometers, and load sensors that sample data 50 times per second. Stance phase control prevents knee buckling through hydraulic resistance, while swing phase optimization adjusts flexion resistance for natural cadence.
| Component Type | Control Method | Response Time | Battery Life | Weight (grams) | Cost Range (USD) |
|---|---|---|---|---|---|
| Microprocessor Knee | Real-time sensors | 20 milliseconds | 24-48 hours | 1,200-1,800 | $40,000-80,000 |
| Hydraulic Knee | Fluid resistance | Immediate | N/A | 800-1,200 | $8,000-15,000 |
| Energy-Return Foot | Carbon fiber spring | Passive | N/A | 400-800 | $3,000-8,000 |
| SACH Foot | Heel cushion | Passive | N/A | 300-500 | $200-500 |
| Vacuum Suspension | Negative pressure | Continuous | 8-12 hours | 200-400 | $2,000-5,000 |
- Energy-Storing and Return (ESAR) feet
- Carbon fiber construction stores 15-20 Joules during loading
- Energy return efficiency reaches 85-95% in elite designs
- Heel-to-toe transition occurs over 40-60% of stance phase
- Multi-axial feet provide ±15 degrees of inversion/eversion
- Hydraulic ankle units offer powered dorsiflexion assistance
- Dorsiflexion range: 10-15 degrees active assistance
- Plantarflexion control: Variable resistance 0-100%
⭐ Clinical Pearl: Microprocessor knee stumble recovery activates within 200 milliseconds of unexpected perturbation, providing maximum extension resistance to prevent falls. Success rate exceeds 95% for forward stumbles on level surfaces.
Suspension systems maintain prosthetic attachment through mechanical, vacuum, or magnetic mechanisms. Elevated vacuum systems create 15-25 mmHg negative pressure, reducing pistoning to <3mm and improving proprioceptive feedback by 40%. Magnetic suspension provides 150+ pounds of retention force with quick-release capability.
Socket interface technology optimizes pressure distribution and comfort. Thermoplastic sockets achieve intimate fit through heat molding at 160-180°C, while carbon fiber construction reduces weight by 30% compared to conventional materials. Silicone liners with gel cushioning distribute pressure over maximum surface area.
💡 Master This: Prosthetic alignment affects component longevity exponentially. Optimal alignment extends component life by 200-300%, while misalignment creates stress concentrations that cause premature failure within 6-12 months.
Upper limb prosthetic systems utilize myoelectric control through surface EMG signals ranging 10-500 microvolts. Pattern recognition algorithms distinguish between 8-12 distinct grip patterns with 95% accuracy. Force feedback systems provide tactile sensation through vibrotactile stimulation at 200-300 Hz.
Modular component systems enable customization for individual patient needs. Pyramid connectors provide ±7 degrees of angular adjustment, while torque adapters accommodate rotational forces up to 150 Nm. Quick-disconnect mechanisms facilitate component exchange for activity-specific optimization.
Understanding component engineering principles enables clinicians to prescribe optimal prosthetic systems that maximize function while ensuring long-term reliability and user satisfaction.
🔧 Component Engineering: The Precision Assembly Matrix
🎯 Clinical Mastery: The Rehabilitation Command Center
Rehabilitation mastery transforms mechanical devices into functional extensions of human capability through evidence-based training protocols and systematic progression. Successful rehabilitation achieves community ambulation in 85% of transtibial and 70% of transfemoral amputees, with energy efficiency approaching 90% of normal values.
📌 Remember: REHABILITATION - Restoring Everyday Human Abilities Builds Independence Lifelong Improving Tasks And Training Integrated Optimally Naturally. Success requires systematic progression and patient dedication.
Pre-prosthetic conditioning establishes foundational strength and range of motion essential for prosthetic success. Residual limb strengthening targets hip abductors (achieving 5/5 strength), hip extensors (maintaining 110+ degrees flexion), and core stability (demonstrating 60-second plank hold). Cardiovascular conditioning reduces prosthetic energy costs by 15-25%.
| Training Phase | Duration (Weeks) | Key Milestones | Success Criteria | Functional Goals |
|---|---|---|---|---|
| Pre-Prosthetic | 4-8 | Wound healing, strength | 5/5 proximal strength | Independence preparation |
| Initial Fitting | 2-4 | Socket tolerance, balance | 8-hour wear time | Static balance >30 sec |
| Basic Gait | 4-6 | Level surface walking | 150m continuous | Household ambulation |
| Advanced Training | 6-12 | Stairs, uneven terrain | Community distances | Unlimited ambulation |
| Maintenance | Ongoing | Skill refinement | Activity participation | Lifestyle integration |
- Parallel bar training (weeks 1-2)
- Weight shifting exercises: 10 repetitions each direction
- Step-to pattern: 20 steps forward/backward
- Balance challenges: Eyes closed for 30 seconds
- Walker assistance (weeks 2-4)
- Continuous walking: 50-100 meters initially
- Cadence training: 90-110 steps/minute target
- Independent ambulation (weeks 4-8)
- Distance goals: 300+ meters for community access
- Speed targets: >0.8 m/s for functional mobility
⭐ Clinical Pearl: Socket pressure tolerance develops progressively over 6-8 weeks. Initial wear time of 30 minutes increases by 1-2 hours daily until 8-hour tolerance is achieved. Skin breakdown occurs when progression exceeds tissue adaptation.
Functional training protocols address activity-specific challenges through task-oriented practice. Stair negotiation requires hip flexor strength >4/5 and prosthetic knee control for safe descent. Uneven terrain training develops anticipatory balance strategies and adaptive gait patterns for environmental challenges.
Technology-assisted training enhances rehabilitation outcomes through real-time feedback and objective monitoring. Pressure-sensitive insoles provide weight-bearing feedback with ±2% accuracy, while accelerometry tracks gait symmetry and step count for home exercise compliance.
💡 Master This: Prosthetic abandonment correlates strongly with inadequate training duration. Minimum 40 hours of structured therapy reduces abandonment rates from 35% to 12%. Peer mentorship programs improve long-term success by additional 25%.
Outcome measurement guides rehabilitation progression through validated assessment tools. Prosthetic Evaluation Questionnaire scores >7/10 indicate successful integration, while Timed Up and Go tests <20 seconds predict community ambulation. Six-minute walk distances >300 meters suggest functional endurance for daily activities.
Advanced training techniques prepare users for high-level activities. Plyometric exercises develop power generation for running and jumping, while sport-specific training enables return to athletics. Occupational integration addresses workplace demands and ergonomic considerations.
Mastering rehabilitation principles enables clinicians to guide patients through systematic progression from initial fitting to optimal functional independence, maximizing both physical capabilities and psychosocial adaptation.
🎯 Clinical Mastery: The Rehabilitation Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















