Pediatric Orthopaedics

On this page
🏗️ Pediatric Orthopaedics: The Growing Skeleton's Engineering Marvel
Growing bones aren't just smaller versions of adult skeletons-they're dynamic structures with unique vulnerabilities and remarkable healing capacities that demand entirely different diagnostic and therapeutic approaches. You'll master how physes absorb forces differently than mature bone, decode injury patterns that reveal mechanism and prognosis, distinguish fractures from normal variants that mimic pathology, and apply evidence-based algorithms that account for remodeling potential. By integrating biomechanics with developmental milestones, you'll build the pattern recognition skills to make confident decisions when a child's future mobility hangs in the balance.

📌 Remember: CHILD - Cartilage predominant, High remodeling potential, Incomplete ossification, Ligamentous laxity, Dynamic growth plates. These five characteristics define every pediatric orthopaedic consideration and differentiate children from "small adults."
The pediatric musculoskeletal system demonstrates remarkable plasticity with 80% of bone remodeling occurring within the first 2 years of life. Growth velocity peaks at 25 cm/year during infancy, then stabilizes to 5-7 cm/year until the pubertal growth spurt reaches 8-12 cm/year. This dynamic environment creates unique injury patterns, healing responses, and treatment considerations.
- Bone Composition Evolution
- Birth: 55% water, 25% organic matrix, 20% minerals
- Adolescence: 25% water, 35% organic matrix, 40% minerals
- Increased flexibility in younger children
- Progressive stiffening with age
- Higher greenstick fracture risk under 8 years
- Growth Plate Physiology
- 4 distinct zones: Reserve, proliferative, hypertrophic, calcification
- Peak growth velocity: 0.5-1.0 mm/week
- Closure sequence: Distal radius (16-18 years), proximal humerus (18-20 years)
| Age Group | Bone Characteristics | Fracture Pattern | Healing Time | Remodeling Potential |
|---|---|---|---|---|
| 0-2 years | 80% cartilage | Plastic deformation | 2-3 weeks | Excellent (>90%) |
| 3-8 years | High water content | Greenstick/buckle | 3-4 weeks | Very good (70-90%) |
| 9-12 years | Transitional | Complete/physeal | 4-6 weeks | Good (50-70%) |
| 13-16 years | Adult-like | Adult patterns | 6-8 weeks | Limited (20-50%) |
| >16 years | Mature cortex | Adult fractures | 8-12 weeks | Minimal (<20%) |
💡 Master This: The 2-year rule governs remodeling potential - significant angular correction occurs only within 2 years of remaining growth. Calculate remaining growth by subtracting current age from expected physeal closure age to predict remodeling capacity.
Connect these foundational principles through biomechanical analysis to understand how pediatric bone responds differently to stress, loading, and injury patterns.
🏗️ Pediatric Orthopaedics: The Growing Skeleton's Engineering Marvel
⚙️ Biomechanical Foundations: The Pediatric Loading System
📌 Remember: PLASTIC - Periosteum thick, Low modulus elasticity, Angled forces cause bending, Stress concentrates at metaphysis, Tension side fails first, Incomplete fractures common, Cortex-cancellous ratio low. This mnemonic captures the essential biomechanical differences in pediatric bone.
Pediatric bone demonstrates a lower elastic modulus (12-15 GPa) compared to adult bone (18-20 GPa), creating increased flexibility but reduced ultimate strength. The thick periosteum provides 60-70% of bone strength in children under 10 years, explaining why periosteal stripping significantly weakens pediatric fractures.
- Age-Related Biomechanical Properties
- 0-5 years: Cortical thickness 2-3 mm, high plasticity
- 6-10 years: Cortical thickness 3-5 mm, transitional properties
- 11-16 years: Cortical thickness 5-8 mm, approaching adult values
- Stress concentration at metaphyseal-diaphyseal junction
- Growth plate represents 2-5x weaker than surrounding bone
- Ligaments stronger than growth plates until age 14
| Loading Pattern | Pediatric Response | Adult Response | Clinical Significance |
|---|---|---|---|
| Compression | Buckle/torus | Comminution | Stable, minimal treatment |
| Bending | Greenstick | Complete | Reduction often required |
| Tension | Avulsion | Ligament tear | Growth plate involvement |
| Torsion | Spiral | Oblique | High instability risk |
| Shear | Physeal separation | Metaphyseal | Growth disturbance potential |
💡 Master This: Growth plate biomechanics follow the weakest link principle - shear forces preferentially disrupt the hypertrophic zone where large chondrocytes create structural weakness. This zone fails at 30-40% of the force required to fracture adjacent metaphyseal bone.
Understanding these biomechanical foundations enables prediction of fracture patterns and guides treatment decisions based on the specific loading mechanisms involved.
⚙️ Biomechanical Foundations: The Pediatric Loading System
🎯 Pattern Recognition: The Pediatric Injury Decoder
📌 Remember: AGES framework - Age-appropriate findings, Growth plate status, Epiphyseal development, Symmetry comparison. Always compare bilateral imaging and correlate findings with expected developmental milestones for accurate interpretation.
- Age-Specific Injury Patterns
- 0-2 years: Non-accidental trauma (NAT) suspicion, metaphyseal corner fractures
- Classic metaphyseal lesions (CML) - 95% specificity for abuse
- Spiral fractures in non-ambulatory children - red flag
- Multiple fractures different ages - high suspicion
- 3-8 years: Supracondylar fractures (55% of elbow injuries)
- Peak incidence 5-7 years during playground activities
- Type III extension patterns require surgical fixation
- Compartment syndrome risk 8-12% with significant swelling
- 9-16 years: Growth plate injuries (Salter-Harris classification)
- Type I-II: 85% good outcomes with proper reduction
- Type III-IV: 30-40% growth disturbance risk
- Type V: 90% growth arrest - rare but devastating
- 0-2 years: Non-accidental trauma (NAT) suspicion, metaphyseal corner fractures
| Clinical Scenario | Key Recognition Pattern | Immediate Action | Critical Threshold |
|---|---|---|---|
| Limp + fever | Septic arthritis vs osteomyelitis | Joint aspiration | WBC >50,000/μL |
| Adolescent hip pain | SCFE vs Perthes disease | Bilateral X-rays | Slip angle >30° |
| Newborn hip click | DDH screening | Ultrasound | Alpha angle <60° |
| Spinal deformity | Idiopathic vs congenital | Full spine X-ray | Cobb angle >20° |
| Limb length difference | Growth disturbance | Scanogram | Difference >2 cm |
💡 Master This: Symmetry comparison reveals 90% of developmental abnormalities. Always obtain bilateral imaging for unilateral complaints in children under 10 years - the contralateral side serves as the patient's own control for normal development.
These recognition patterns form the foundation for systematic evaluation and guide appropriate imaging, consultation, and treatment decisions.
🎯 Pattern Recognition: The Pediatric Injury Decoder
🔬 Differential Diagnosis: The Systematic Discriminator
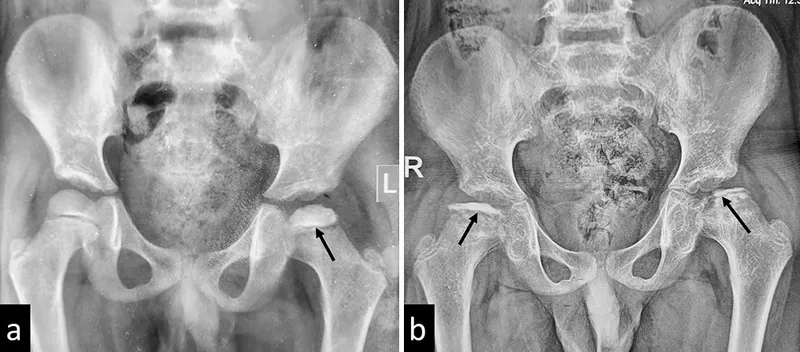
📌 Remember: DISCO method - Demographics (age/sex), Imaging findings, Symptoms duration, Clinical examination, Outcome patterns. This systematic approach ensures comprehensive evaluation of similar-appearing conditions.
- Hip Pain Differential by Age
- 2-6 years: Transient synovitis vs septic arthritis
- Kocher criteria: 4 factors = 99.6% septic arthritis probability
- Temperature >38.5°C, non-weight bearing, ESR >40 mm/hr, WBC >12,000
- Transient synovitis: self-limiting, 7-10 days resolution
- 4-8 years: Legg-Calvé-Perthes disease vs septic arthritis
- Perthes: insidious onset, bilateral 10%, male predominance 4:1
- Lateral pillar classification guides prognosis and treatment
- Group A: >90% good outcomes, observation only
- 10-16 years: SCFE vs Perthes (late stage)
- SCFE: acute vs chronic based on 3-week symptom duration
- Stable vs unstable - ability to bear weight determines AVN risk
- Unstable SCFE: 47% AVN rate vs <5% in stable slips
- 2-6 years: Transient synovitis vs septic arthritis
| Condition | Peak Age | Gender Ratio | Key Imaging | Bilateral Risk | Treatment Priority |
|---|---|---|---|---|---|
| Transient synovitis | 3-8 years | M:F 2:1 | Joint effusion | Rare (<5%) | Observation |
| Septic arthritis | Any age | M:F 1.5:1 | Effusion + destruction | 10-15% | Emergency surgery |
| Perthes disease | 4-8 years | M:F 4:1 | Fragmentation | 10-20% | Containment |
| SCFE | 10-16 years | M:F 1.5:1 | Posterior slip | 25-40% | Immediate fixation |
| Osteomyelitis | Any age | M:F 1.2:1 | Metaphyseal changes | Rare | Antibiotics + surgery |
💡 Master This: Time-sensitive diagnoses in pediatric orthopaedics include septic arthritis (<6 hours for joint preservation), unstable SCFE (<24 hours to minimize AVN), and compartment syndrome (<6 hours for tissue viability). Delayed recognition results in permanent disability in >80% of cases.
Understanding these differential frameworks enables rapid, accurate diagnosis and prevents the devastating consequences of missed time-sensitive conditions.
🔬 Differential Diagnosis: The Systematic Discriminator
⚕️ Treatment Algorithms: The Evidence-Based Decision Tree
📌 Remember: GROWTH principles - Guided by remaining growth, Remodeling potential, Optimal timing, Weight-bearing status, Tissue healing capacity, Hardware considerations. These factors determine treatment selection and timing in pediatric patients.
- Age-Specific Treatment Considerations
- 0-5 years: Maximum remodeling potential
- Angular deformities <20 degrees - observation
- Fracture reduction tolerance: 15 degrees angulation, 1 cm shortening
- Spica casting preferred over internal fixation
- Complication rate <5% with conservative management
- 6-12 years: Transitional treatment approaches
- Flexible nailing for diaphyseal fractures
- Growth plate preservation priority
- Remodeling decreases 50% every 2 years after age 8
- Surgical indications become more stringent
- 13-18 years: Adult-pattern treatment
- Rigid fixation appropriate for metaphyseal fractures
- Limited remodeling potential requires anatomic reduction
- Growth plate closure allows adult techniques
- Complication rates approach adult levels
- 0-5 years: Maximum remodeling potential
| Condition | Conservative Success | Surgical Indications | Optimal Timing | Long-term Outcomes |
|---|---|---|---|---|
| DDH | 95% (age <6 months) | Failed Pavlik harness | Before walking | 90% normal hips |
| Clubfoot | 85% (Ponseti method) | Resistant deformity | Birth to 2 years | 95% functional feet |
| Scoliosis | 70% (curves <25°) | Progressive curves >45° | Before peak growth | 85% curve control |
| SCFE | 0% (requires fixation) | All cases | Immediate diagnosis | 95% if stable |
| Growth plate injury | 80% (Types I-II) | Displaced Types III-V | <7 days post-injury | 70% normal growth |
💡 Master This: Growth-friendly techniques preserve physeal function while correcting deformity. Guided growth using 8-plates can correct 1 degree per month of angular deformity, while growing rods control spinal deformity with 70-80% curve correction and continued growth.
These treatment algorithms provide systematic approaches to complex pediatric orthopaedic decisions, optimizing outcomes while minimizing intervention-related complications.
⚕️ Treatment Algorithms: The Evidence-Based Decision Tree
🌐 Multi-System Integration: The Developmental Network
📌 Remember: SYSTEMS approach - Skeletal primary, Yet Systemic connections, Time-dependent interactions, Endocrine influences, Metabolic factors, Synergistic treatments. This framework ensures comprehensive evaluation beyond isolated orthopaedic findings.
- Neurological-Orthopaedic Interactions
- Cerebral palsy: 80% develop orthopaedic complications
- Spastic diplegia: Hip subluxation 35%, scoliosis 25%
- GMFCS Level IV-V: 90% require orthopaedic intervention
- Single-event multilevel surgery (SEMLS) optimizes outcomes
- Gait analysis guides surgical planning in ambulatory patients
- Spina bifida: Level-dependent orthopaedic manifestations
- L3-L4 lesions: Hip flexion contractures, knee instability
- L5-S1 lesions: Foot deformities, ankle instability
- Tethered cord: Progressive scoliosis, neurological deterioration
- Hydrocephalus: 15% develop spinal deformity
- Cerebral palsy: 80% develop orthopaedic complications
| Neurological Condition | Orthopaedic Manifestation | Prevalence | Treatment Approach | Outcome Predictor |
|---|---|---|---|---|
| Cerebral palsy | Hip displacement | 35-40% | Soft tissue + bony | GMFCS level |
| Spina bifida | Scoliosis | 60-90% | Growing rods | Neurological level |
| Muscular dystrophy | Contractures | 90% | Stretching + surgery | Ambulation status |
| Spinal muscular atrophy | Spinal deformity | 80% | Bracing + fusion | Respiratory function |
| Charcot-Marie-Tooth | Foot deformities | 70% | Tendon transfers | Disease progression |
💡 Master This: Metabolic bone disease affects fracture healing and surgical outcomes. Vitamin D deficiency (<20 ng/mL) delays fracture healing by 30-40%, while rickets increases deformity recurrence after correction by 60%. Optimize metabolic status before elective procedures.
Understanding these multi-system interactions enables comprehensive care planning and improves long-term functional outcomes in complex pediatric patients.
🌐 Multi-System Integration: The Developmental Network
🎯 Clinical Mastery Arsenal: The Rapid Reference Toolkit
📌 Remember: RAPID assessment - Recognize patterns, Assess urgency, Prioritize interventions, Implement protocols, Document outcomes. This systematic approach ensures nothing is missed during high-pressure clinical situations.
- Emergency Recognition Thresholds
- Septic arthritis: 4 Kocher criteria = 99.6% probability
- Temperature >38.5°C, non-weight bearing, ESR >40, WBC >12,000
- Joint aspiration within 6 hours prevents cartilage destruction
- Empiric antibiotics: Clindamycin 40 mg/kg/day + Ceftriaxone 100 mg/kg/day
- Compartment syndrome: Pressure >30 mmHg or ΔP <30 mmHg
- 5 P's: Pain, Pallor, Paresthesias, Pulselessness, Paralysis
- Pain with passive stretch - earliest and most reliable sign
- Fasciotomy within 6 hours prevents permanent damage
- Unstable SCFE: Inability to bear weight regardless of pain level
- Emergency reduction within 24 hours minimizes AVN risk
- AVN rate: 47% unstable vs <5% stable slips
- Prophylactic pinning of contralateral hip in high-risk patients
- Septic arthritis: 4 Kocher criteria = 99.6% probability
| Clinical Scenario | Recognition Time | Action Window | Success Rate | Failure Consequence |
|---|---|---|---|---|
| Septic arthritis | <2 hours | <6 hours | 95% normal joint | Permanent damage |
| Compartment syndrome | <1 hour | <6 hours | 90% function | Amputation risk |
| Unstable SCFE | Immediate | <24 hours | 85% AVN prevention | Hip collapse |
| Open fracture | <30 minutes | <6 hours | 95% union | Infection/nonunion |
| Neurovascular injury | <15 minutes | <4 hours | 90% recovery | Permanent deficit |
💡 Master This: Growth remaining calculation guides all treatment decisions: Girls - menarche + 2 years, Boys - voice change + 3 years, or Risser 4-5 on X-ray. Remaining growth <2 years eliminates remodeling potential and requires adult treatment approaches.
These rapid-reference tools enable confident decision-making in high-pressure pediatric orthopaedic situations, ensuring optimal outcomes through systematic, evidence-based approaches.
🎯 Clinical Mastery Arsenal: The Rapid Reference Toolkit
Continue reading on Oncourse
Sign up for free to access the full lesson, plus unlimited questions, flashcards, AI-powered notes, and more.
CONTINUE READING — FREEor get the app
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Practice Questions: Pediatric Orthopaedics
Test your understanding with these related questions
What is the most common bone fractured in children?












