Foot & Ankle Blueprint - Bones & Moves
- Bones (26 total):
- Tarsals (7): Talus, Calcaneus, Navicular, Cuboid, 3 Cuneiforms.
- Metatarsals (5).
- Phalanges (14).
- Key Joints & Primary Movements:
- Talocrural (Ankle): Tibia, Fibula, Talus. Hinge; Dorsiflexion (DF)/Plantarflexion (PF).
⭐ The talocrural joint (ankle joint proper) is a hinge joint formed by the tibia, fibula, and talus, primarily allowing dorsiflexion and plantarflexion.
- Subtalar: Talus, Calcaneus. Inversion/Eversion.
- Chopart's (Midtarsal): Talonavicular & Calcaneocuboid.
- Lisfranc's (Tarsometatarsal): Tarsals & Metatarsal bases.
- Talocrural (Ankle): Tibia, Fibula, Talus. Hinge; Dorsiflexion (DF)/Plantarflexion (PF).
- Stabilizers:
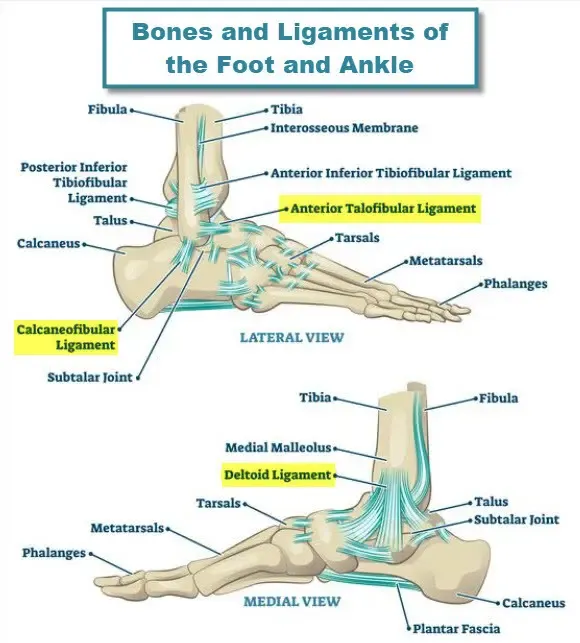
- Ligaments: Deltoid (medial), ATFL, CFL, PTFL (lateral), Spring.
- Arches: Medial & Lateral Longitudinal, Transverse.
- Combined Movements (Triplanar):
- Pronation: Eversion + Abduction + DF.
- Supination: Inversion + Adduction + PF.
Walking the Walk - Gait Mechanics
- Gait Cycle: Two main phases:
- Stance Phase (60%): Foot contacts ground. Key for shock absorption, stability, propulsion.
- Swing Phase (40%): Foot airborne. Essential for limb advancement.
- Foot's Role:
- Shock absorption & terrain adaptation (pronation).
- Rigid lever for push-off (supination).
- Phases of Gait:
⭐ The windlass mechanism, involving tightening of the plantar fascia, is crucial for arch elevation and creating a rigid lever for propulsion during the toe-off phase of gait.

Arch Support System - Springs & Struts
Foot arches (Medial & Lateral Longitudinal, Transverse) vital for locomotion, weight-bearing.
- Static Stabilizers (Springs): Ligaments.
- Plantar Calcaneonavicular (Spring) Ligament: Key for Medial Longitudinal Arch (MLA).
- Plantar Aponeurosis: Supports MLA; Windlass mechanism.
- Long & Short Plantar Ligaments: Support Lateral Longitudinal Arch (LLA).
- Dynamic Stabilizers (Struts): Muscles/Tendons.
- Tibialis Posterior: Main dynamic MLA support.
- Peroneus Longus: Supports LLA & Transverse Arch.
- Intrinsic muscles: Fine-tune support.
- Functions: Shock absorption, terrain adaptation, propulsion lever.
- Clinical: Pes Planus (Flatfoot): ↓ arch height; Pes Cavus (High Arch): ↑ arch height.

⭐ The medial longitudinal arch is primarily supported by the plantar calcaneonavicular (spring) ligament, tibialis posterior tendon, and plantar aponeurosis. Its integrity is vital for shock absorption.
When Things Go Wrong - Injury Biomechanics
Forces exceeding tissue tolerance or repetitive microtrauma cause injury. Altered mechanics predispose to pathologies.
- Ankle Sprains:
- Common: Inversion injury (ATFL).
⭐ The anterior talofibular ligament (ATFL) is the most commonly injured ligament in inversion ankle sprains, typically occurring with combined plantarflexion and inversion.
- Plantar Fasciitis:
- Repetitive tensile overload of plantar aponeurosis.
- Risks: Pes planus/cavus, tight Achilles.
- Achilles Tendinopathy:
- Overuse, eccentric loading; watershed zone (2-6 cm proximal to insertion) vulnerable.
- Stress Fractures:
- Repetitive submaximal loading → fatigue failure.
- Sites: Metatarsals (March), Tibia, Navicular.
- Hallux Valgus:
- Lateral toe, medial 1st metatarsal deviation.
- Risks: Footwear, genetics.

High‑Yield Points - ⚡ Biggest Takeaways
- Windlass mechanism: Plantar fascia tightens with MTP dorsiflexion, elevating the arch for propulsion.
- Subtalar joint: Dominant for inversion/eversion; Ankle (tibiotalar) joint: Primarily for dorsiflexion/plantarflexion.
- Foot arches (longitudinal & transverse): Essential for shock absorption and weight distribution.
- Achilles tendon: Strongest tendon, crucial for plantarflexion power during push-off.
- Lisfranc (TMT) & Chopart (transverse tarsal) joints: Key for midfoot stability and motion.
- Gait: Foot transitions from flexible shock absorber to rigid lever for propulsion_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

