Pre-Op MBD Assessment - Setting Stage Wisely
- Clinical Clues:
- History: Fragility fractures (hip, wrist, spine), chronic bone pain, steroid/anticonvulsant use.
- Examination: Skeletal deformities, point tenderness, gait abnormalities.
- Key Investigations:
- Labs (MBD Panel):
- Serum: Ca (total/ionized), PO₄, ALP, PTH, 25(OH)D.
- Renal Function Tests (RFTs), Liver Function Tests (LFTs).
- Imaging:
- X-rays: Osteopenia, pseudofractures (Looser's zones), cortical thinning.
- DEXA scan: T-score ≤ -2.5 indicates osteoporosis.
⭐ Always check Vitamin D (25-OH Vit D); target >30 ng/mL pre-op. Deficiency (<20 ng/mL) common.
- Labs (MBD Panel):
- Pre-Surgical Optimization:
- Correct Ca & Vitamin D levels.
- Specific MBD treatment (e.g., bisphosphonates, teriparatide).
- Multidisciplinary approach: Endocrinology, Anesthesia.
Osteoporosis Surgery - Brittle Bone Solutions
- Pre-operative Optimization:
- Correct Ca & Vit D deficiency.
- Consider teriparatide for ≥3 months pre-op in severe cases to ↑ bone density.
- Bisphosphonates: ⚠️ Hold if atypical femur fracture suspected; continue for other fragility fractures.
- Intra-operative Strategies:
- Gentle tissue handling.
- Use of locking plates/screws for better purchase in weak bone.
- Polymethylmethacrylate (PMMA) cement augmentation for screw fixation.
- Consider arthroplasty for displaced hip fractures.
- Post-operative Care:
- Aggressive DVT prophylaxis.
- Early mobilization & physiotherapy.
- Fall prevention strategies.
- Long-term anti-osteoporotic medication.
⭐ Vertebroplasty or kyphoplasty can provide significant pain relief and stabilization for painful osteoporotic vertebral compression fractures unresponsive to conservative treatment within 6-12 weeks.
- Challenges:
- Implant loosening/cut-out.
- Delayed union/non-union.
- Peri-prosthetic fractures.
- 📌 B-A-D B-O-N-E-S: Bisphosphonates, Adequate Ca/Vit D, DEXA scan, Bone cement, Optimize nutrition, No falls, Exercise, Special implants (locking plates).
Osteomalacia/Rickets Surgery - Soft Bone Strategies
- Pre-op: Correct metabolic defects (Vit D, $Ca^{2+}$, $PO_4^{3-}$); optimize nutrition.
- Intra-op:
- Gentle bone handling; avoid excessive periosteal stripping.
- Fixation: IM nails (long bones), multiple K-wires, or locking plates for better soft bone purchase.
- Bone grafting for defects or to augment healing.
- Post-op: Protected weight-bearing. Ensure continued metabolic therapy for bone mineralization.
⭐ Prophylactic fixation of Looser's zones (pseudofractures) in weight-bearing areas is often indicated to prevent complete fractures and facilitate healing.
 oka
oka
Paget's & PTH Ops - Taming Wild Bone
- Paget's Disease:
- Highly vascular bone: ↑ intra-op bleeding. Pre-op bisphosphonates (e.g., zoledronate) can ↓ vascularity.
- Deformities (e.g., bowing) & pathological fractures common.
- Surgical challenges: joint replacement (protrusio acetabuli), fracture fixation.
- Rare: osteosarcoma development.
- Hyperparathyroidism (Primary - PTH Ops):
- Brown tumors (osteitis fibrosa cystica): regress post-parathyroidectomy.
- Pathological fractures.
- ⚠️ Post-op: "Hungry Bone Syndrome" - severe hypocalcemia. Monitor $Ca^{2+}$ closely.
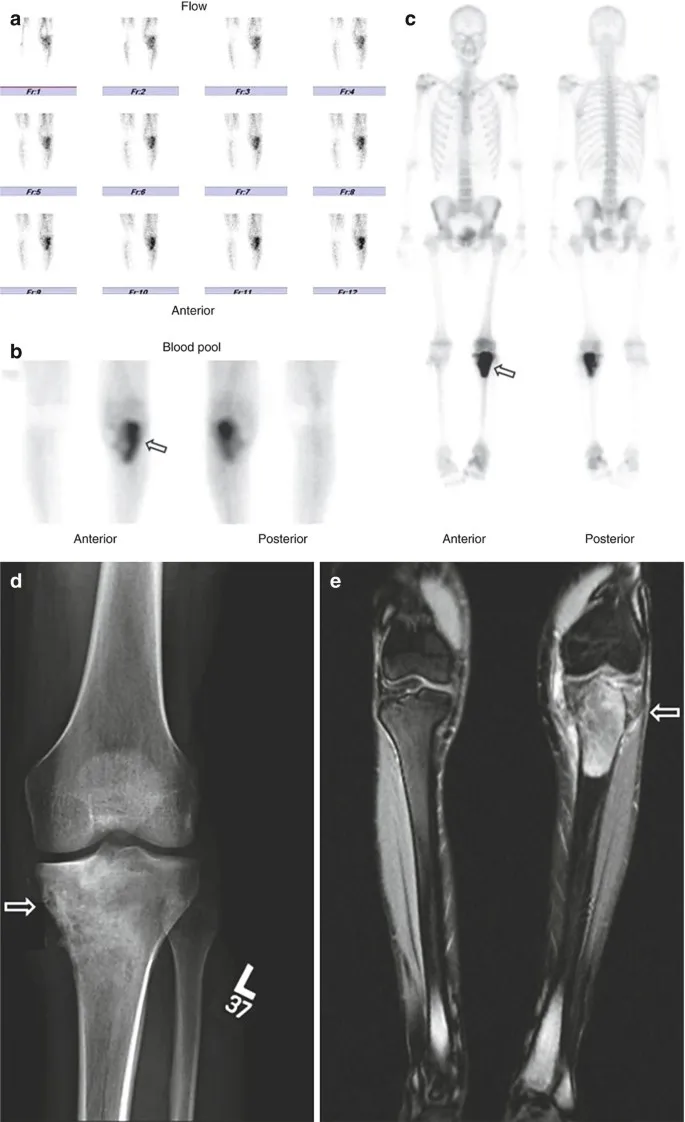
⭐ In Paget's disease, prophylactic internal fixation may be considered for fissures in long bones to prevent complete fractures, especially in weight-bearing areas.
MBD Post-Op Care - Healing & Holding Strong
- Optimize nutrition: adequate Calcium, Vitamin D, protein intake.
- Prolonged immobilization & protected weight-bearing often necessary.
- High risk: delayed union, non-union, implant failure due to poor bone quality.
- VTE prophylaxis essential, especially with prolonged immobility.
- Early, cautious physiotherapy to prevent stiffness, aid recovery.
- Manage underlying MBD: continue/initiate specific medical treatment.
⭐ For patients on long-term bisphosphonates presenting with atypical femoral fractures, teriparatide use post-operatively can promote fracture healing.
High‑Yield Points - ⚡ Biggest Takeaways
- Osteoporosis: ↑ fracture risk necessitates pre-op Ca/Vit D optimization and augmented fixation (cement/locking plates).
- Osteomalacia: Soft bones cause delayed union; correct Vit D deficiency pre-surgery.
- Paget's Disease: ↑ vascularity/bleeding risk; pre-op bisphosphonates mitigate this during surgery.
- Pathological fractures: Common in MBDs; consider prophylactic fixation for impending lesions, especially in weight-bearing bones.
- Hyperparathyroidism: Manage brown tumors and bone resorption; parathyroidectomy for primary HPTH improves bone mass.
- General: Nutritional support (Protein, Vit D, Ca) is vital for optimal healing and surgical outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

