Intro & Risks - Bone Basics & Breakers
- Definition: Low bone mass, microarchitectural decay, ↑ fracture risk.
⭐ WHO: Osteoporosis = BMD T-score ≤ -2.5 (spine, hip, femoral neck).
- Epidemiology: Common in postmenopausal women, elderly. India: High; ~1/3 women, ~1/8 men >50 yrs.
- Risk Factors:
- Non-Modifiable: Age, female, genetics, early menopause (<45 yrs), prior fracture.
- Modifiable: 📌 ACCESS
- Alcohol
- Corticosteroids (≥5mg pred/day, ≥3 mo)
- Calcium low
- Estrogen low
- Smoking
- Sedentary
- Others: Vit D deficiency, low BMI, some meds (anticonvulsants, PPIs).
 oka
oka
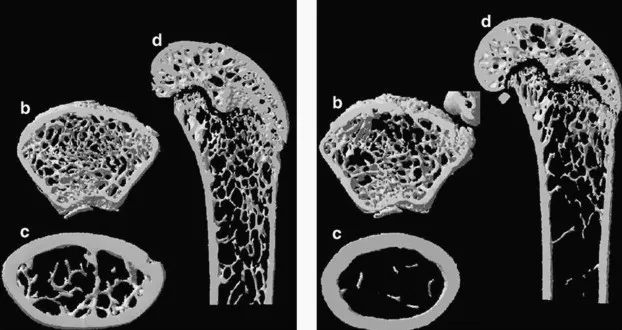
Pathophys & Types - How Bones Weaken
-
Pathophysiology: Bone remodeling imbalance: ↑osteoclast activity (resorption), ↓osteoblast activity (formation).
- RANKL/OPG Pathway:
- ↑RANKL (Receptor Activator of Nuclear factor Kappa-B Ligand) → ↑osteoclast differentiation & activity.
- OPG (Osteoprotegerin - decoy receptor for RANKL) → ↓osteoclast activity.
- Estrogen ↓ (e.g., postmenopause) → ↑RANKL & ↓OPG → ↑bone resorption.
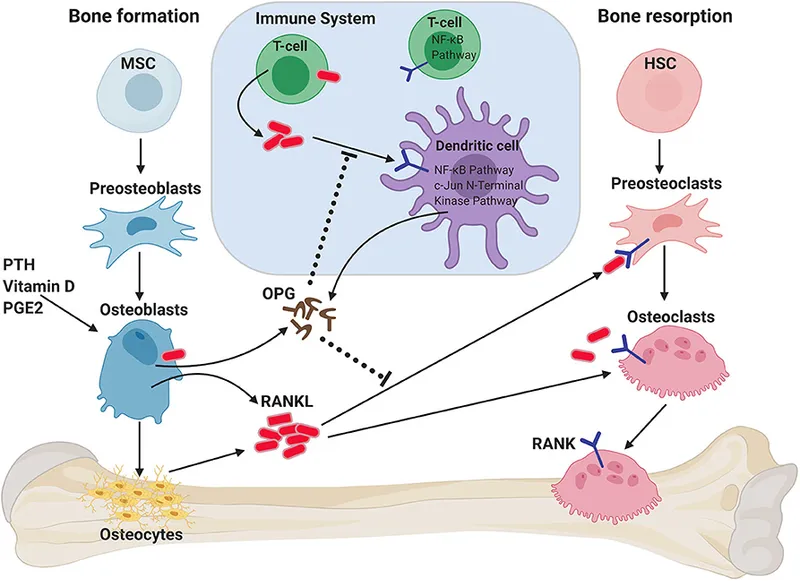
⭐ In postmenopausal osteoporosis, estrogen deficiency leads to increased expression of RANKL and decreased OPG, tipping the balance towards bone resorption.
- RANKL/OPG Pathway:
-
Types of Osteoporosis:
- Primary Osteoporosis:
- Type 1 (Postmenopausal): Estrogen ↓. Affects mainly trabecular bone.
- Type 2 (Senile): Age-related (typically > 70 years). Affects trabecular & cortical bone.
- Secondary Osteoporosis: Result of other conditions or medications.
- Key Causes: Corticosteroids (most common drug-induced), hyperparathyroidism, anticonvulsants, malabsorption syndromes, Chronic Kidney Disease (CKD).
- Primary Osteoporosis:
Diagnosis & Workup - Spotting Brittle Bones
- Clinical Features: Often silent until fragility fracture.
- Common sites: Hip, vertebra, wrist.
- Signs: Height loss, kyphosis.
- Diagnosis:
- DEXA Scan: Gold standard.
- T-score: Osteopenia (-1.0 to -2.4), Osteoporosis (≤ -2.5).
- Z-score: For premenopausal women, men <50 yrs, children.
- FRAX Tool: Calculates 10-year fracture probability.
- DEXA Scan: Gold standard.
- Key Investigations (to exclude secondary causes):
- Serum Calcium, Phosphate, ALP.
- Vitamin D (25-OHD).
- PTH.
⭐ A DEXA T-score of -2.5 or lower at the lumbar spine, total hip, or femoral neck is diagnostic of osteoporosis. A history of fragility fracture also diagnoses clinical osteoporosis irrespective of T-score.

Treatment & Prevention - Building Bone Armor
- Non-Pharmacological & Prevention Strategies:
- Calcium & Vitamin D supplementation (e.g., Calcium 1000-1200mg/day, Vitamin D 800-1000 IU/day)
- Regular weight-bearing & muscle-strengthening exercise
- Smoking cessation & alcohol moderation (≤1-2 drinks/day)
- Fall prevention measures (home safety, balance training)
- Pharmacological Therapy:
- Antiresorptives: Target osteoclast activity
- Bisphosphonates: Alendronate (70mg/week orally), Risedronate (35mg/week orally or 150mg/month orally), Zoledronic acid (5mg IV annually)
- Denosumab (RANKL inhibitor): 60mg SC every 6 months
- SERMs (e.g., Raloxifene 60mg/day orally - esp. for younger postmenopausal women with spinal osteoporosis)
- Anabolics: Stimulate osteoblast activity
- Teriparatide (PTH analogue): 20mcg SC daily (max 2 years)
- Antiresorptives: Target osteoclast activity
⭐ Oral bisphosphonates (e.g., Alendronate) are generally first-line pharmacological therapy. Must be taken on an empty stomach with a full glass of water, remaining upright for at least 30-60 minutes to prevent esophagitis. 📌 Alendronate: All Alone (empty stomach), Ample wAter, Afterwards Avoid recumbency.
High‑Yield Points - ⚡ Biggest Takeaways
- Osteoporosis is defined by low bone mass and microarchitectural deterioration, leading to ↑ fracture risk.
- Most common fractures: Vertebral compression fractures (most frequent), hip, and distal radius (Colles').
- Gold standard diagnosis: DEXA scan with a T-score ≤ -2.5.
- Serum calcium, phosphate, and ALP are typically normal in uncomplicated osteoporosis.
- Key risk factors include postmenopausal state, prolonged corticosteroid use, and vitamin D deficiency.
- Bisphosphonates (e.g., alendronate) are first-line treatment; teriparatide for severe cases.
- The FRAX score is a tool used to estimate the 10-year probability of major osteoporotic fracture.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

