BMD Basics - Density Deep Dive
- Bone Mineral Density (BMD): Areal density of bone mineral ($g/cm^2$). Key indicator of bone strength & fracture risk.
- Gold Standard: Dual-energy X-ray absorptiometry (DEXA/DXA).
- T-score: BMD vs. young, healthy, sex-matched adult mean (peak bone mass).
- Normal: ≥ -1.0 SD
- Osteopenia: < -1.0 to > -2.5 SD
- Osteoporosis: ≤ -2.5 SD
- Severe: Osteoporosis + ≥1 fragility fracture.
- Z-score: BMD vs. age-, sex-matched peers. For premenopausal women, men <50 yrs, children.
⭐ A T-score of -2.5 SD or lower is diagnostic of osteoporosis in postmenopausal women and men aged 50 and older.
Indications - Scan Signals
- Universal Screening:
- Women ≥ 65 years
- Men ≥ 70 years
- Risk-Based Screening (Younger Individuals):
- Postmenopausal women < 65 yrs with risk factors
- Men aged 50-69 yrs with risk factors
- Specific High-Risk Conditions/Factors:
- Fragility fracture (adults >50 yrs)
⭐ Glucocorticoid therapy (≥ 5 mg prednisone/day or equivalent for ≥ 3 months) is a critical indication.
- Low body weight (BMI < 19 kg/m²) or significant weight loss (>10%)
- Parental history of hip fracture
- Medical conditions: RA, hypogonadism, hyperparathyroidism, IBD
- Lifestyle: Current smoking, high alcohol intake (>3 units/day)
- Other Clinical Scenarios:
- Radiographic osteopenia or vertebral deformity
- Monitoring response to osteoporosis therapy
- Before initiating pharmacologic therapy for osteoporosis
DXA Deconstructed - Pixel Perfect PEEK
- Principle: Measures Bone Mineral Density (BMD) using dual X-ray beams.
- Key Sites:
- Lumbar spine (L1-L4)
- Hip (total, femoral neck)
- Forearm (distal radius): if spine/hip unusable or in hyperparathyroidism.
- Scores & Interpretation:
- T-score: BMD vs. young adult (sex-matched).
- Normal: T-score $\ge \textbf{-1.0}$
- Osteopenia: T-score between $\textbf{-1.0}$ and $\textbf{-2.5}$
- Osteoporosis: T-score $\le \textbf{-2.5}$
- Severe Osteoporosis: T-score $\le \textbf{-2.5}$ + fragility fracture.
- Z-score: BMD vs. age-matched (premenopausal women, men <50y, children).
- $\le \textbf{-2.0}$: "Below expected range for age".
- T-score: BMD vs. young adult (sex-matched).
- Pros: Gold standard, low radiation, precise.
- Cons: Artifacts (osteophytes, vertebral #, calcification) affect accuracy.
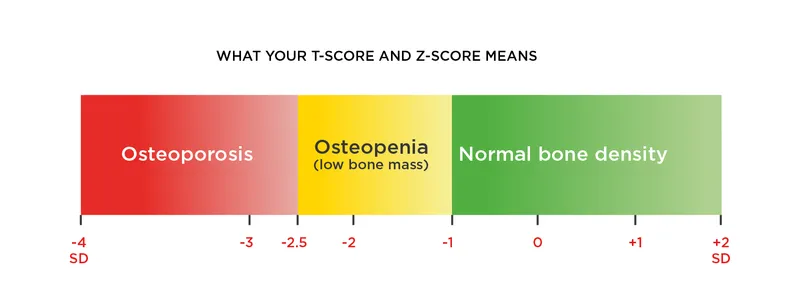
⭐ A T-score of -2.5 or lower at key sites (spine, total hip, femoral neck) diagnoses osteoporosis.
T-Scores & Z-Scores - Decoding Density
- T-Score: BMD vs. young adult (same sex). For postmenopausal women & men >50 yrs.
- Normal: ≥ -1.0 SD
- Osteopenia: -1.0 to -2.5 SD
- Osteoporosis: ≤ -2.5 SD
- Severe: ≤ -2.5 SD + fragility fracture
- Z-Score: BMD vs. age-sex-ethnicity matched peers. For premenopausal women, men <50 yrs, children.
- ≤ -2.0 SD: "Below expected range for age"; investigate secondary causes.
-
-2.0 SD: "Within expected range for age".

⭐ T-score is key for diagnosing osteoporosis in postmenopausal women and men >50 years.
FRAX & Follow-Up - Crystal Ball BMD
- FRAX: 10-yr major osteoporotic & hip fracture probability.
- Uses Clinical Risk Factors (CRFs) ± BMD.
- Key CRFs: Age, BMI, prior fracture, steroids, parental hip fracture, smoking, alcohol.
- Intervention: Based on country-specific FRAX thresholds (e.g., major ≥20%, hip ≥3%).
- Follow-Up:
- BMD check: 1-2 yrs post-therapy initiation.
- Stable/low risk: BMD every 2-5 yrs.
- Bisphosphonates: Consider drug holiday after 3-5 yrs.
⭐ FRAX is primarily for treatment-naive individuals to guide decisions on initiating therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- DEXA (Dual-energy X-ray absorptiometry) is the gold standard for BMD assessment.
- T-score: Compares patient's BMD to young, healthy, sex-matched adults.
- Z-score: Compares patient's BMD to age, sex, and ethnicity-matched peers.
- WHO diagnostic criteria for osteoporosis: T-score ≤ -2.5 SD; Osteopenia: T-score -1.0 to -2.5 SD.
- Preferred DEXA sites: lumbar spine (L1-L4), hip (femoral neck/total hip).
- FRAX tool calculates 10-year probability of major osteoporotic fracture.
- Quantitative Ultrasound (QUS) of the calcaneus is a portable screening tool, not for definitive diagnosis of osteoporosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

