Foot & Ankle Arthritis: Overview & Etiology - Joint Under Siege
- Definition: Degenerative or inflammatory joint disease affecting foot/ankle articulations, leading to pain, stiffness, and ↓ function.
- Commonly Affected Joints:
- Ankle (Tibiotalar)
- Subtalar (Talocalcaneal)
- Midfoot (Talonavicular, Calcaneocuboid)
- Forefoot (Metatarsophalangeal - MTP, esp. 1st MTP: Hallux Rigidus)
- Etiology:
- Primary Osteoarthritis (OA): Age-related, idiopathic. Less common in ankle unless predisposed.
- Secondary OA (Most common for ankle):
- Post-Traumatic Arthritis (PTA): Following fractures, severe sprains, or instability.
- Inflammatory Arthritis: Rheumatoid Arthritis (RA), Spondyloarthropathies (e.g., Psoriatic Arthritis, Ankylosing Spondylitis).
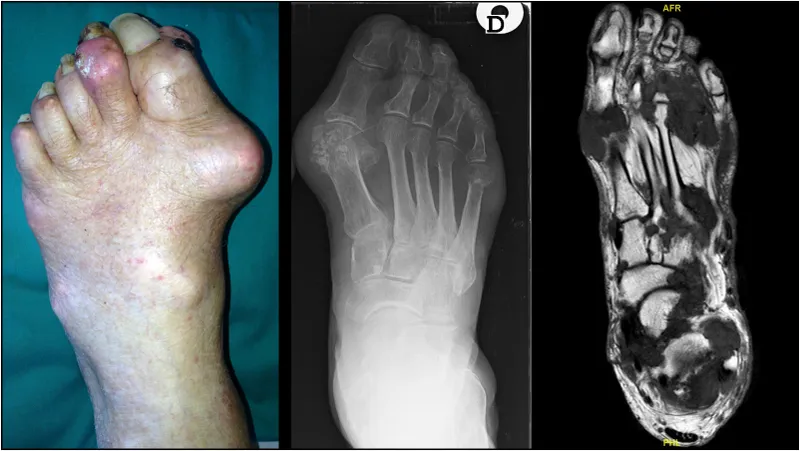
- Crystal Arthropathy: Gout (1st MTP classic - Podagra), Pseudogout (CPPD).
- Septic Arthritis: Joint infection aftermath.
- Neuropathic Arthropathy (Charcot Joint): Diabetes, nerve damage.

⭐ Post-traumatic arthritis is the leading cause of ankle arthritis, accounting for approximately 70-80% of cases, often years after the initial injury.
Foot & Ankle Arthritis: Clinical Picture - Groans & Limps
- Pain (Groans):
- Key symptom; site-specific (ankle, subtalar, midfoot, MTP).
- Nature: Aching, sharp with activity; night pain (severe).
- Timing: Activity-linked (OA); morning stiffness (OA <30 min, RA >30 min).
- Swelling & Deformity:
- Effusion, bony enlargement (osteophytes).
- Progressive deformity: valgus/varus, pes planus/cavus, hallux valgus.
- Stiffness:
- Morning or post-inactivity ("gelling").
- Functional Limitation (Limps):
- Antalgic gait (limp).
- ↓ walking distance, difficulty with uneven terrain/stairs.
- Footwear modification often needed.
- Associated Signs:
- Crepitus, locking, instability.
- Crepitus, locking, instability.
⭐ First Metatarsophalangeal (MTP) joint arthritis commonly presents with pain and stiffness, significantly impacting the push-off phase of gait (hallux rigidus if OA).
Foot & Ankle Arthritis: Diagnostic Clues - X-Ray Vision
- Weight-bearing X-rays: Key initial investigation.
- Views: Ankle (AP, Lat, Mortise), Foot (AP, Lat, Oblique).
- Harris view (axial for subtalar joint).
- Key X-Ray Signs (📌 JOSS):
- JSN (Joint Space Narrowing): Asymmetric (OA), Symmetric (RA).
- Osteophytes (bone spurs, typical in OA).
- Subchondral Sclerosis (↑ bone density).
- Subchondral cysts (fluid-filled cavities).
- Specific Patterns:
- RA: Symmetrical JSN, marginal erosions, osteopenia.
- Gout: "Rat-bite" erosions (punched-out), tophi.
- PsA: "Pencil-in-cup" deformity, periostitis.
- Advanced Imaging (if needed):
- MRI: Early cartilage/soft tissue changes, bone marrow edema.
- CT: Detailed bone anatomy, pre-op planning.

⭐ Mortise view (ankle AP with 15-20° internal rotation) is crucial for true tibiotalar joint space assessment, unmasking talar tilt or subtle JSN.
Foot & Ankle Arthritis: Management Strategies - Steps to Relief
- Conservative Management (Stepwise):
- Education & Lifestyle: Weight loss, low-impact activity.
- Pharmacological: NSAIDs, Acetaminophen. Intra-articular Corticosteroids (max 3-4/year/joint). Viscosupplementation.
- Physical Therapy: Stretching, strengthening, gait training.
- Orthotics: Shoe modifications (rocker sole), custom inserts, ankle braces (AFO).

- Surgical Interventions (If conservative fails):
- Arthroscopy: Debridement, synovectomy, loose body removal.
- Arthrodesis (Fusion): Gold standard for end-stage arthritis (e.g., ankle, subtalar). Pain relief & stability; sacrifices motion.
- Arthroplasty (Replacement): Total Ankle Replacement (TAR) preserves motion for suitable candidates.
- Osteotomy: Realigns bone to offload arthritic joint area.
⭐ Ankle arthrodesis is the gold standard for end-stage ankle arthritis, offering predictable pain relief and stability.
High-Yield Points - ⚡ Biggest Takeaways
- Ankle arthritis is predominantly post-traumatic; rheumatoid arthritis and primary OA are other causes.
- First MTP joint is the hallmark site for gout (podagra) and hallux rigidus (OA).
- Midfoot arthritis frequently follows Lisfranc injuries or occurs in Charcot neuroarthropathy.
- Conservative management includes NSAIDs, orthotics, and intra-articular injections.
- Arthrodesis (joint fusion) remains the gold standard for severe ankle and hindfoot arthritis.
- Total Ankle Replacement (TAR) is a motion-preserving option for select ankle OA cases.
- Cheilectomy (osteophyte removal) is indicated for early hallux rigidus.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

