Foot & Ankle Bones - Skeletal Blueprint
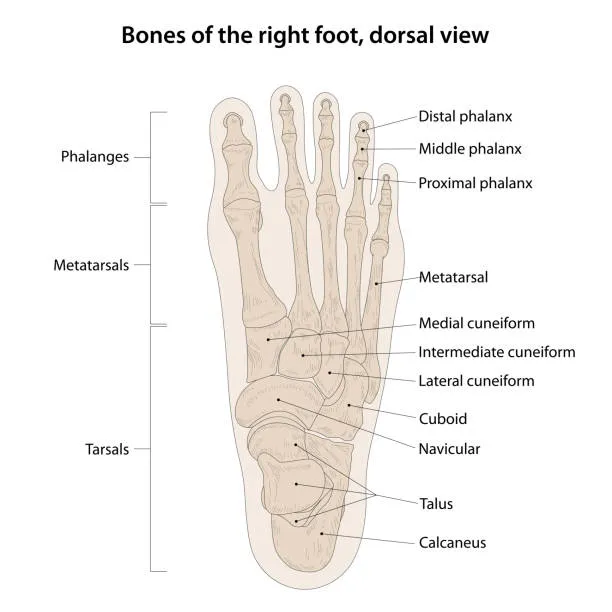
- Tarsal Bones (7): Hindfoot (Talus, Calcaneus); Midfoot (Navicular, Cuboid, 3 Cuneiforms - Medial, Intermediate, Lateral).
- 📌 Mnemonic: Tiger Cubs Need MILC. (Talus, Calcaneus, Navicular, Medial, Intermed, Lat cuneiforms, Cuboid).
- Metatarsals (5): Numbered I-V (medial to lateral).
- 1st: shortest, thickest.
- 5th: styloid process (peroneus brevis; avulsion #).
- Phalanges (14):
- Great Toe (Hallux): 2 (proximal, distal).
- Lesser Toes (II-V): 3 each (proximal, middle, distal).
- Sesamoids: Typically 2, under 1st metatarsal head.
⭐ Talus: no muscle attachments; blood supply via neck (↑AVN risk with #).
Foot & Ankle Joints & Ligaments - Stability Straps

- Ankle (Talocrural) Joint: Hinge; Tibia, Fibula, Talus.
- Movements: Dorsiflexion/Plantarflexion.
- Ligaments:
- Medial (Deltoid): Tibionavicular, Tibiocalcaneal, Ant. & Post. Tibiotalar. Very strong.
- Lateral: Anterior Talofibular (ATFL) 📌, Calcaneofibular (CFL), Posterior Talofibular (PTFL).
⭐ ATFL: Most commonly injured in ankle sprains (inversion injury). Weakest lateral ligament.
- Subtalar (Talocalcaneal) Joint: Plane; Talus, Calcaneus.
- Movements: Inversion/Eversion.
- Ligament: Interosseous talocalcaneal (strongest).
- Midtarsal (Chopart's) Joint: Talonavicular & Calcaneocuboid.
- Ligament: Bifurcate (Calcaneonavicular, Calcaneocuboid parts).
- Tarsometatarsal (Lisfranc's) Joint Complex:
- Ligament: Lisfranc (Medial cuneiform to 2nd Met base). Key for midfoot arch.
- Spring Ligament (Plantar Calcaneonavicular): Supports medial arch.
Foot & Ankle Muscles & Tendons - Motion Masters
- Anterior (Dorsiflexion):
- Tibialis Anterior: Main dorsiflexor, inverts.
- EHL, EDL: Toe extensors.
- Lateral (Eversion):
- Peroneus Longus & Brevis: Primary evertors, assist plantarflexion.
- Posterior (Plantarflexion):
- Superficial: Gastrocnemius, Soleus (Achilles tendon).
- Deep: Tibialis Posterior (main invertor, arch support), FDL, FHL. 📌 Medial Malleolus (ant→post): Tibialis post., FDL, Artery (post. tibial), Vein, Nerve (tibial), FHL. (Tom, Dick And Very Nervous Harry)

⭐ Thompson test: Squeeze calf; no plantarflexion = Achilles rupture. Often with palpable gap.
Foot & Ankle Neurovascular Supply - Lifeline Network

- Arteries:
- Anterior Tibial → Dorsalis Pedis (DP). Pulse: lateral to EHL.
- Posterior Tibial → Medial & Lateral Plantar Arteries. Pulse: posterior to medial malleolus.
- Plantar arteries + DP branch form Deep Plantar Arch.
- Nerves:
- Tibial N. → Medial & Lateral Plantar Nerves (sole: sensory/motor).
- Common Peroneal N.:
- Deep Peroneal: Ant. compartment motor; 1st web sensory.
- Superficial Peroneal: Lat. compartment motor; dorsum sensory (most).
- Sural N.: Lateral foot/heel sensory.
- Saphenous N.: Medial ankle/foot sensory.
⭐ Tarsal Tunnel Syndrome: Tibial Nerve (or branches) compression under flexor retinaculum, causing pain/paresthesia.
Foot Arches & Biomechanics - Spring in Step
- Three Arches: Medial Longitudinal (MLA), Lateral Longitudinal (LLA), Transverse.
- MLA Support: Tibialis posterior, spring ligament, plantar aponeurosis, FHL.
- Function: Weight bearing, shock absorption, propulsion (windlass mechanism).
- Deformities: Pes planus (fallen MLA), Pes cavus (exaggerated MLA).

⭐ The integrity of the spring ligament (plantar calcaneonavicular ligament) is paramount for static support of the medial longitudinal arch.
High‑Yield Points - ⚡ Biggest Takeaways
- Ankle joint (talocrural): tibia, fibula, talus; main movements are dorsiflexion/plantarflexion.
- Subtalar joint: crucial for inversion and eversion of the foot.
- Medial Deltoid ligament is strong; lateral ATFL is most commonly sprained.
- Tibialis Posterior tendon is key dynamic support for the medial longitudinal arch.
- Lisfranc joint: tarsometatarsal articulation. Chopart joint: talonavicular and calcaneocuboid joints.
- Deep Peroneal nerve injury: foot drop and 1st web space sensory loss.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

