OA Pharmacotherapy - Pain Game Plan
- Goals: Pain relief, improve function, slow progression?
- Cornerstone: Non-pharmacological (exercise, weight loss) is key.
- Stepwise Approach:
- Analgesia (Paracetamol $≤$4g/day).
- NSAIDs (topical/oral, lowest dose/duration). COXIBs for GI risk.
- IA injections (steroids for flares; hyaluronans - variable).
- Adjuncts (Duloxetine, Tramadol for refractory pain).
⭐ Weight loss and exercise are crucial non-pharmacological interventions with proven efficacy in OA.
First-Line Responders - Gentle Symptom Soothers
Initial options focus on symptom relief with favorable safety.
| Feature | Acetaminophen (Paracetamol) | Topical NSAIDs (e.g., Diclofenac gel) |
|---|---|---|
| MOA | Central analgesic, weak anti-inflammatory | Local COX inhibition (↓ prostaglandins) |
| Dosage | Max ≤3-4g/day | Per product; e.g., Diclofenac gel 2-4 times/day |
| Efficacy | Modest for OA symptoms | Good for localized OA (knee, hand) |
| Side Effects | Hepatotoxicity (high doses) | Local skin reactions; ↓ systemic SE vs oral |
| Place in Tx | Initial oral analgesic | Localized OA; if oral NSAIDs contraindicated |
NSAIDs - Inflammation Busters Inc.
NSAIDs reduce pain & inflammation by inhibiting Cyclooxygenase (COX) enzymes.
- Mechanism:
- COX-1: "Housekeeping" enzyme (maintains GI mucosal protection, platelet function, renal blood flow).
- COX-2: Inducible enzyme (upregulated during inflammation; mediates pain, fever, inflammation).
- Types & Comparison:
| Feature | Non-selective NSAIDs (e.g., Ibuprofen, Naproxen, Diclofenac) | COX-2 Selective Inhibitors (e.g., Celecoxib, Etoricoxib) |
|---|---|---|
| MOA | Inhibit both COX-1 & COX-2 | Preferentially inhibit COX-2 |
| GI Risk | ↑↑ (PUD, bleeding) due to COX-1 inhibition | ↓ (compared to non-selective, but risk is not eliminated) |
| CV Risk | ↑ (especially Diclofenac and high doses of others; MI, stroke) | ↑↑ (MI, stroke); Naproxen often considered lower CV risk among NSAIDs |
| Renal Risk | Present (AKI, Na+/water retention, hypertension) | Present (AKI, Na+/water retention, hypertension) |
- Efficacy: Generally similar for OA symptom relief at equivalent anti-inflammatory doses.
- Strategies to Minimize GI Toxicity:
- Co-prescription with a Proton Pump Inhibitor (PPI) or Misoprostol.
- Use the lowest effective dose for the shortest possible duration.
- Consider COX-2 selective inhibitors in patients at high GI risk but low CV risk.
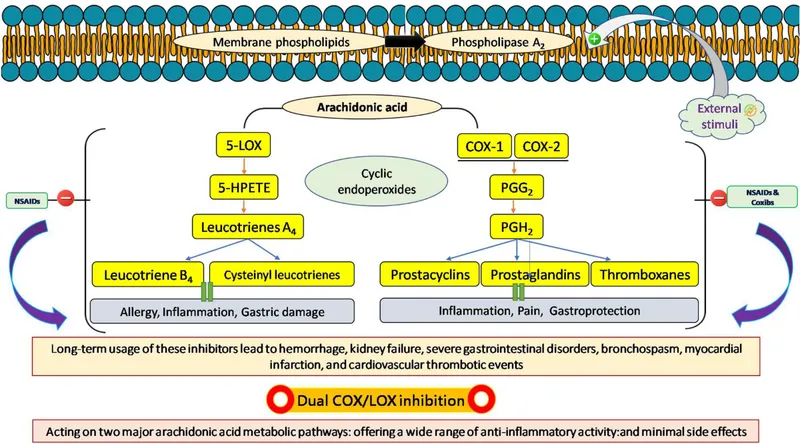
⭐ All NSAIDs, including selective COX-2 inhibitors, carry a black box warning from the FDA regarding increased risk of serious cardiovascular thrombotic events (including MI and stroke) and serious gastrointestinal adverse events (including bleeding, ulceration, and perforation).
Joint Injections & Other Players - Niche Tactics
- Intra-articular (IA) Corticosteroids (e.g., Triamcinolone, Methylprednisolone)
- Rapid pain relief (short-term: weeks to months)
- Indications: Acute flare-ups, severe pain
- Limit: ≤3-4 injections/year/joint
- ⚠️ Risk: Chondrotoxicity, infection with frequent use.
- IA Hyaluronic Acid (Viscosupplementation)
- Mechanism: Restores synovial fluid viscoelasticity, lubrication
- Delayed onset (weeks), modest, variable benefit
- Variable guideline recommendations; some do not recommend.
-
Comparison: IA Steroids vs. IA Hyaluronic Acid
Feature IA Corticosteroids IA Hyaluronic Acid Onset Rapid Delayed Duration Weeks-Months Months Use Acute Flares Chronic Pain / Mobility MOA Anti-inflammatory ↑Synovial Viscoelasticity -
Symptomatic Slow-Acting Drugs in OA (SYSADOAs)
- Examples: Glucosamine sulfate/HCl, Chondroitin sulfate. Diacerein inhibits $IL-1\beta$.
- MOA (general): Proposed chondroprotective & anti-inflammatory.
- Evidence controversial; slow onset (months), generally well-tolerated.
⭐ Diacerein, a SYSADOA, is known for its gastrointestinal side effects, particularly diarrhea, which can limit its clinical utility.
-
Other Agents
- Duloxetine (SNRI): For chronic musculoskeletal pain, including OA, especially with neuropathic component.
- Topical Capsaicin: Depletes substance P from nerve endings; for localized pain.
High‑Yield Points - ⚡ Biggest Takeaways
- Acetaminophen: First-line analgesic for mild-moderate OA pain.
- NSAIDs (oral/topical): For persistent pain/inflammation; topical NSAIDs preferred for localized OA, fewer systemic effects.
- Intra-articular Corticosteroids: Provide rapid, short-term relief for acute flares.
- Intra-articular Hyaluronic Acid: Viscosupplementation offering modest, delayed benefits.
- Duloxetine: For chronic OA pain, especially with neuropathic features or central sensitization.
- Tramadol: For moderate-severe pain unresponsive to other analgesics.
- Topical Capsaicin: Alternative for localized pain, acts by depleting Substance P; requires regular application for effect and may cause initial burning sensation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

