Conservative Rx of Degenerative Disorders - Joint Reality Check
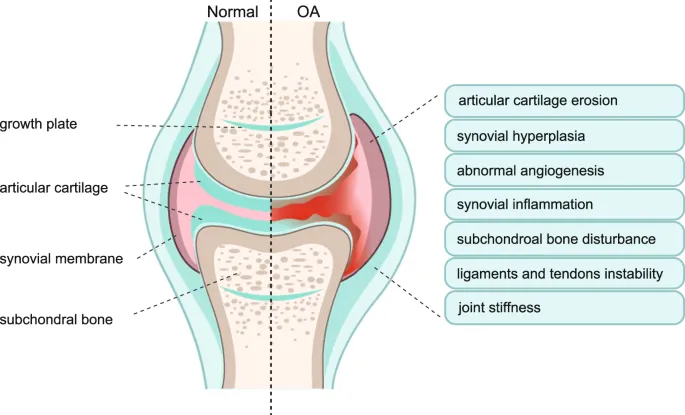
- Osteoarthritis (OA): Most common degenerative joint disorder. Progressive cartilage loss, subchondral bone changes, osteophyte formation.
⭐ Osteoarthritis is the most common type of arthritis, primarily characterized by cartilage degeneration and osteophyte formation.
- Clinical Impact: Chronic pain, stiffness (especially morning/inactivity), ↓ range of motion (ROM), functional limitation, impaired Quality of Life (QoL).
- Commonly Affected Joints: Knees, hips, hands (DIP, PIP, CMC1), spine (facet, intervertebral discs).
- Conservative Management Goals:
- Pain control & symptom relief
- Maintain/improve joint function & mobility
- Patient education on disease & self-care
- Enhance overall QoL
- Delay or avoid surgery.
- Approach: Holistic, patient-centered, multimodal_approach tailored to individual needs and disease severity, focusing on non-pharmacological and pharmacological interventions before considering surgery_ (This part makes it slightly over 100, let's re-evaluate the last point for conciseness).
Conservative Rx of Degenerative Disorders - Lifestyle & Motion Magic
- Lifestyle Modifications:
- Weight Loss: 5-10% body weight reduction ↓ pain, ↑ function in knee/hip OA.
- Activity Modification: Low-impact (e.g., swimming, cycling); avoid overuse, joint stressing activities.
- Patient Education: Disease understanding, self-management, joint protection techniques.
- Exercise Therapy ("Motion Magic"):
- Goals: ↓ Pain, ↑ Function, ↑ Range of Motion (ROM), ↑ Muscle strength.
- Key types: Strengthening (esp. quadriceps, hip abductors), ROM exercises, low-impact aerobic conditioning (e.g., walking, aquatic).
⭐ Quadriceps strengthening is crucial for knee OA, significantly improving pain and function.
- Assistive Devices:
- Canes (used in contralateral hand), walkers, crutches to offload joint.
- Braces (e.g., unloader knee brace for varus/valgus deformity), orthotics (e.g., shock-absorbing insoles).

-
Exercise in OA: Types & Benefits
Exercise Type Benefit(s) in OA Strengthening ↑ Joint stability, ↓ Pain, ↑ Function, Muscle support Range of Motion (ROM) Maintains/↑ joint mobility, ↓ Stiffness Aerobic (Low-Impact) ↑ Cardiovascular fitness, Weight control, Mood boost Hydrotherapy ↓ Joint load, Pain relief, Eases movement
Conservative Rx of Degenerative Disorders - Pill Power Plays
Key Drug Classes for Osteoarthritis (OA) Management
| Class | MOA | Examples | ADRs | Key Points |
|---|---|---|---|---|
| Analgesics | Central analgesic | Paracetamol | Hepatotoxicity (high dose) | Max 3-4g/day. Generally first-line for mild-moderate OA. |
| Weak opioid, SNRI | Tramadol | Nausea, dizziness, seizure risk | Adjunct for moderate to severe pain. | |
| NSAIDs | COX inhibition | Ibuprofen, Diclofenac (topical/oral), Celecoxib | GI, renal, CV risk | Lowest dose, shortest duration. Topical for localized OA. Consider PPI with oral. |
| IA Corticosteroids | Potent anti-inflammatory | Triamcinolone | Local pain, infection (rare) | Rapid relief (lasts 4-8 wks). Max 3-4/yr/joint. |
| IA Hyaluronic Acid | Viscosupplementation | Sodium Hyaluronate | Local reaction | Modest benefit, often delayed onset. |
| Duloxetine | SNRI | Duloxetine | Nausea, dry mouth, fatigue | For chronic pain, esp. if neuropathic component. |
Conservative Rx of Degenerative Disorders - Support & Struts
- Purpose: ↓Pain, ↑Stability, ↓Joint load, ↑Function.
- Knee Braces:
- Unloader (Valgus/Varus): For unicompartmental OA.
⭐ Unloader braces shift the weight-bearing axis from the damaged to the healthy cartilage compartment.
- Patellofemoral: For patellofemoral OA/pain.
- Hinged: Provides mediolateral stability.
- Unloader (Valgus/Varus): For unicompartmental OA.
- Spinal Orthoses:
- Cervical collars (soft/rigid): Limit motion, provide support.
- Lumbosacral corsets/belts: Support, proprioception, limit gross movement.
- Foot & Ankle Orthotics:
- Arch supports, heel wedges, MCR insoles.
- AFOs (Ankle-Foot Orthoses): For foot drop, instability.
- Hand & Wrist Splints:
- Thumb spica (CMC OA), wrist splints (e.g., carpal tunnel, wrist OA).
- Assistive Devices:
- Canes, walkers, crutches: Reduce joint loading, improve balance.
- Cane: Used in contralateral hand. 📌 (COAL: Cane Opposite Affected Leg)
- Canes, walkers, crutches: Reduce joint loading, improve balance.
High‑Yield Points - ⚡ Biggest Takeaways
- Lifestyle modification (weight loss, activity adjustment) is first-line management.
- NSAIDs and acetaminophen are key analgesics; COX-2 inhibitors for GI safety.
- Intra-articular corticosteroids offer short-term pain relief (weeks to months).
- Viscosupplementation (hyaluronic acid) shows variable efficacy for knee OA.
- Physical therapy (strengthening, ROM exercises) is crucial for function.
- Patient education and joint protection techniques are vital.
- Assistive devices (canes, braces) reduce joint load and improve mobility.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

